What Is Urticaria (Hives)? Symptoms, Causes, and Treatment
Hives can develop for many reasons — including allergic reactions, stress, infections, or adverse responses to certain medications. While most episodes are temporary and mild, some can become chronic or severe, requiring medical attention.
Understanding Urticaria
Urticaria manifests as red or skin-colored welts that may appear in circular, ring-like, or irregular patterns. The condition can appear suddenly and disappear within hours, or persist and recur over weeks.
In some cases, hives are accompanied by angioedema — a deeper form of swelling that affects the dermis, subcutaneous tissue, or mucous membranes. Angioedema often involves the face, lips, eyelids, hands, feet, or genitals. When it affects the throat or larynx, it can cause airway obstruction and become life-threatening. Abdominal pain can also occur if the swelling involves the intestinal walls.
While acute hives often resolve with antihistamines or disappear on their own, chronic urticaria — defined as outbreaks lasting more than six weeks — can significantly impact quality of life and may indicate an underlying health issue or autoimmune response.
Signs and Symptoms
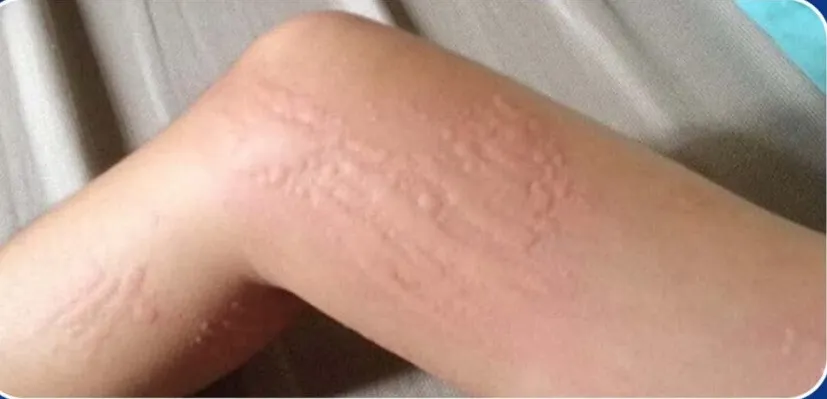
The hallmark symptom of urticaria is the appearance of itchy welts on the skin. These welts may:
- Be red or flesh-colored, round, ring-shaped, or irregular.
- Change shape or size rapidly, sometimes merging to form larger patches.
- Move around the body, disappearing in one area and appearing in another.
- Turn pale or whitish when pressed (known as blanching).
Each individual hive typically lasts from 30 minutes to 24 hours, but new ones can continue to appear. The rash may flare up repeatedly before subsiding completely.
How Hives Affect Daily Life
Although hives are not contagious, their symptoms — itching, swelling, and discomfort — can be disruptive. Persistent itching often leads to scratching or rubbing, which can further irritate the skin and interfere with sleep, concentration, and daily activities. Chronic urticaria can also cause emotional distress, especially when visible areas like the face or arms are affected.
When to See a Doctor
Most cases of hives clear up within 24–48 hours. However, if symptoms persist, recur for weeks, or are accompanied by severe allergic signs, immediate medical evaluation is necessary.
Seek emergency medical care if hives occur with any of the following:
- Wheezing or shortness of breath
- Tightness in the throat or chest
- Difficulty swallowing or speaking
- Swelling of the face, tongue, or lips
- Fever or general malaise
These may indicate anaphylaxis, a serious allergic reaction that requires prompt treatment.
Causes of Urticaria (Hives)
Hives occur when certain cells in the body — primarily mast cells — release histamine and other inflammatory chemicals into the bloodstream. This release triggers swelling, redness, and itching in the skin’s small blood vessels.
In many cases, the exact cause of chronic hives remains unclear, and doctors may not always determine why an acute episode sometimes progresses into a long-term condition. However, several factors and triggers have been identified:
- Pain relievers such as aspirin, ibuprofen, or certain nonsteroidal anti-inflammatory drugs (NSAIDs)
- Insect bites or parasitic infections
- Bacterial or viral infections
- Scratching or skin irritation
- Exposure to heat or cold
- Emotional stress or anxiety
- Sunlight or ultraviolet exposure
- Physical exertion or exercise
- Consumption of alcohol or specific foods (such as shellfish, nuts, or food additives)
- Pressure on the skin, for example from tight clothing or belts
In some individuals, chronic urticaria may be linked to underlying health conditions such as thyroid disorders, autoimmune diseases, or — in rare cases — certain types of cancer.
Risk Factors for Developing Hives
Who Is More Likely to Get Hives?
Anyone can experience hives, but people with sensitive immune systems or a history of allergic reactions are at higher risk. Those who frequently experience seasonal allergies, food intolerances, or environmental sensitivities may develop hives more easily in response to triggers.
Additionally, hives may occur as an external symptom of an internal condition, including hormonal imbalance, liver dysfunction, or autoimmune disorders.
Common Factors That Increase the Risk of Hives
Certain habits and environmental exposures can heighten susceptibility to hives, including:
- Poor personal hygiene or inadequate skin care
- Frequent contact with allergens, such as specific foods, medications, insect bites, pet dander, or pollen
- Genetic predisposition or allergic tendency, meaning individuals with a family history of allergies or asthma are more likely to develop urticaria
In general, maintaining a balanced immune system, avoiding known allergens, and practicing healthy lifestyle habits can significantly reduce the likelihood and severity of hives flare-ups.

Diagnosis and Treatment of Urticaria (Hives)
Diagnostic Tests and Evaluation
In most cases, hives (urticaria) can be diagnosed based on clinical presentation alone and do not require laboratory testing — unless there are signs suggesting an underlying condition such as infection or autoimmune disease.
For recurrent, persistent, or atypical cases, further evaluation may be necessary to identify potential causes or comorbidities. Doctors may consider:
- Allergy skin testing (skin prick or patch test) to identify allergic triggers.
- Routine blood tests, including complete blood count (CBC) and biochemistry profiles.
- Liver function tests to assess metabolic or hepatic causes.
- Thyroid-stimulating hormone (TSH) levels to screen for autoimmune thyroid disease, which is sometimes linked to chronic urticaria.
Additional investigations may be guided by symptoms or abnormal results, such as:
- Autoimmune screening (if immune disorders are suspected).
- Hepatitis serology and abdominal ultrasound to evaluate possible liver dysfunction.
- Parasitic testing in cases of elevated eosinophils.
- Cryoglobulin levels or creatinine tests for suspected systemic inflammation or renal involvement.
- Thyroid antibodies when TSH levels are abnormal.
A skin biopsy may be indicated if the diagnosis remains uncertain, or if hives persist for more than 48 hours, to rule out urticarial vasculitis or other dermal inflammatory conditions.
Effective Treatment for Hives
Treatment for urticaria focuses on relieving symptoms, identifying triggers, and preventing recurrence. The specific approach depends on the severity of the condition and the patient’s overall health.
Key management strategies include:
- Avoiding known triggers or allergens, such as certain foods, medications, insect bites, or environmental irritants.
- Using antihistamines as first-line therapy to reduce itching, redness, and swelling.
- Short-term corticosteroids may be prescribed for severe flare-ups that do not respond to antihistamines, under medical supervision.
- Immunomodulatory agents (such as omalizumab or cyclosporine) may be considered for chronic or treatment-resistant cases.
- Topical soothing agents or mild moisturizers can help reduce skin irritation and dryness.

Lifestyle and Prevention of Urticaria (Hives)
Healthy Habits to Help Manage and Prevent Hives
Maintaining a clean and balanced lifestyle plays a key role in reducing the frequency and severity of urticaria flare-ups. Simple daily habits can help protect the skin, minimize exposure to allergens, and strengthen your immune system.
Daily Lifestyle Tips:
Wash your hands regularly to reduce the risk of bacterial or viral infections that may trigger hives.
Maintain good personal hygiene and keep your skin clean and dry.
Stay up to date on vaccinations to prevent infections that could provoke immune reactions.
Avoid close contact with individuals who have contagious skin conditions or visible hives.
Use mild, fragrance-free soaps and cleansers to prevent skin irritation and dryness.
Wear loose, breathable clothing made of natural fabrics such as cotton to reduce friction and sweating.
Limit exposure to allergens like pollen, pet dander, or dust mites, especially if you have a known sensitivity.
Manage stress levels, as psychological stress can worsen chronic urticaria in some individuals.
Dietary Recommendations
Your diet can play a supportive role in preventing allergic skin reactions and promoting overall skin health.
- Avoid common trigger foods such as seafood, shellfish, beef, eggs, peanuts, or spicy dishes if you have known sensitivities.
- Incorporate anti-inflammatory foods like fresh fruits, leafy greens, and omega-3-rich sources (e.g., salmon, flaxseeds, walnuts).
- Stay hydrated by drinking enough water throughout the day to support your body’s natural detoxification.
- Limit alcohol and processed foods, which can exacerbate inflammation or histamine release.
Effective Prevention Strategies
By combining lifestyle adjustments and preventive care, you can significantly reduce the likelihood of hives or allergic flare-ups.
If you are aware of specific triggers, take proactive steps such as:
- Avoiding foods or substances that trigger allergic reactions.
- Asking your doctor for alternative medications if your current prescription contains allergens or known irritants.
- Following infection control practices, such as regular handwashing and avoiding contaminated environments.
- Strengthening your immune system through balanced nutrition, adequate sleep, and regular exercise.
Consistent preventive care and awareness of your body’s reactions can make a significant difference in managing urticaria and maintaining healthy skin.
