What Is Seborrheic Dermatitis? Causes and Prevention Principles
Understanding Seborrheic Dermatitis
Seborrheic dermatitis (also known as seborrheic eczema or seborrhea) is a chronic relapsing inflammatory skin condition characterized by erythematous (reddish) patches with greasy, yellowish scales. The lesions typically occur in sebaceous gland–rich areas such as the scalp, face, and chest.
However, the disease can also affect other parts of the body, particularly where sebaceous glands are active, including:
- The back and chest
- The forehead and sides of the nose
- The eyebrows and behind the ears
- The armpits, groin, and umbilicus
The condition is common in infants, often within the first three months of life (commonly called cradle cap), and in adults aged 30–70 years.
Several factors can influence the onset or severity of seborrheic dermatitis:
- Genetic predisposition
- Emotional or physical stress
- Cold or dry weather
- Hormonal changes
- Neurological or immune system disorders
In some cases, seborrheic dermatitis may coexist with or precede psoriasis, a combination sometimes referred to as seborrhiasis. The disease tends to be more severe in individuals with Parkinson’s disease, HIV/AIDS, or compromised immune systems. Rarely, it may spread widely across the body, leading to generalized erythroderma.
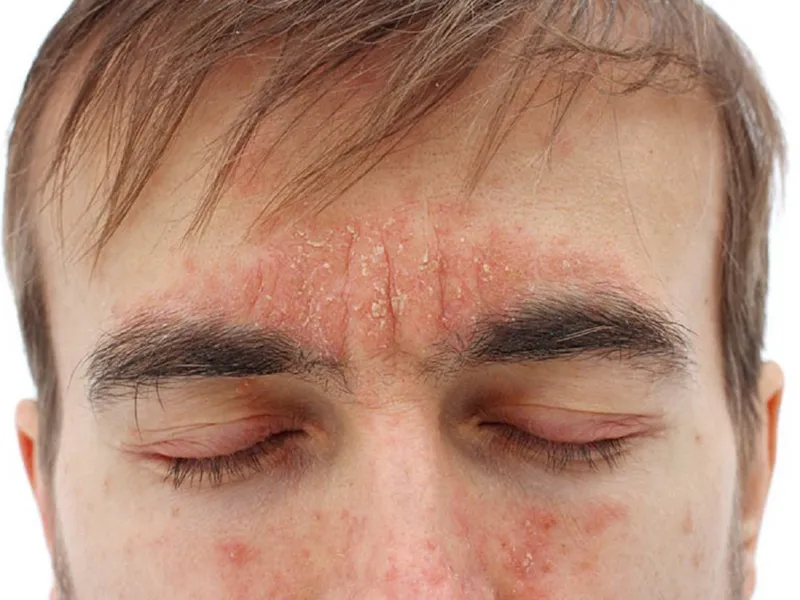
Symptoms of Seborrheic Dermatitis
Symptoms usually develop gradually and may vary in intensity. The most common presentation is flaky, greasy scales or dandruff on the scalp, accompanied by itching or burning sensations.
In more severe cases, yellowish-red papules or plaques can appear along:
- The hairline and forehead
- The sides of the nose and eyebrows
- The ear canals and behind the ears
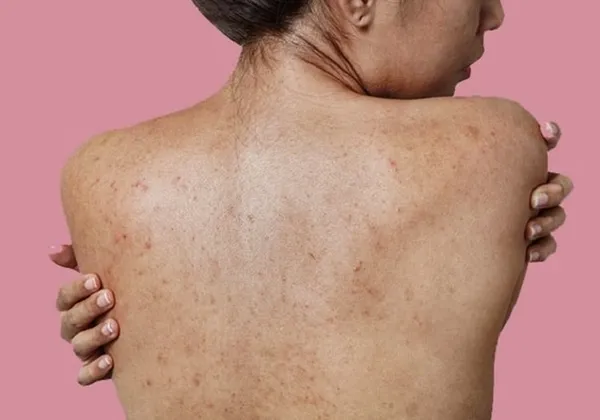
- The chest (sternum) and armpits
Some patients may develop eyelid inflammation (blepharitis), with yellow crusts and mild conjunctival irritation. Importantly, seborrheic dermatitis does not cause hair loss, although the scaling and inflammation may make the scalp appear unhealthy.
In infants, seborrheic dermatitis often presents as thick, yellowish, greasy crusts on the scalp, sometimes accompanied by redness or cracking behind the ears and diaper rash.
In older children and adults, the lesions may form thick, scaly patches about 1–2 cm in diameter.
Impact on Health and Quality of Life
Although seborrheic dermatitis is not life-threatening, it can significantly affect emotional well-being and quality of life.
Persistent itching, burning, or visible flaking can lead to self-consciousness, embarrassment, and social anxiety, particularly when lesions appear on the face or scalp.
The chronic nature of the disease and frequent relapses may also contribute to psychological stress, which in turn can worsen symptoms — forming a vicious cycle.
Possible Complications
Seborrheic dermatitis tends to recur periodically and may progress into a chronic condition. Flare-ups are common during stressful periods or cold, dry seasons.
In rare cases, widespread inflammation may lead to generalized erythroderma, requiring medical intervention.
Secondary bacterial or fungal infections (especially from Malassezia species) may develop when the skin barrier is compromised due to scratching or irritation.
When to See a Doctor
You should consult a dermatologist if you notice:
- Persistent redness, itching, or scaling that doesn’t improve with over-the-counter treatments
- Signs of infection (pain, swelling, or oozing lesions)
- Worsening of symptoms during stress or seasonal changes
Causes and Risk Factors of Seborrheic Dermatitis
What Causes Seborrheic Dermatitis?
The exact cause of seborrheic dermatitis remains unclear, but research suggests that an overgrowth of Malassezia yeast (particularly Malassezia ovale or M. furfur) and certain bacteria such as Propionibacterium acnes play a key role in its development. These microorganisms normally live on the skin but can multiply excessively under favorable conditions, triggering inflammation.
Excessive production of sebum (oil) creates an ideal environment for Malassezia to thrive, which in turn stimulates an inflammatory response. Studies have shown that people with dandruff or seborrheic dermatitis tend to have higher levels of antibodies against Malassezia compared with healthy individuals. This indicates that the immune system in affected individuals reacts abnormally to this yeast.
Additionally, an impaired skin barrier, hormonal changes, and stress can exacerbate the condition.
Who Is at Risk of Seborrheic Dermatitis?
Seborrheic dermatitis can occur at any age but is most common in infants and adults between 30 and 60 years old. Among adults and adolescents, men are more frequently affected than women, possibly due to hormonal influences on sebum production.
While the condition can appear in otherwise healthy people, it is often more severe in individuals with underlying medical or neurological conditions. Common risk groups include:
- People with oily or combination skin Excess oil production provides an optimal growth environment for Malassezia yeast.
- Those with a family history of seborrheic dermatitis or psoriasis Genetic predisposition appears to influence the risk of developing chronic inflammatory skin conditions.
- Individuals with preexisting skin disorders, such as acne or psoriasis.
- People with weakened immune systems, including patients who have undergone organ transplants, those with lymphoma, or those living with HIV/AIDS.
- Individuals with neurological or psychiatric conditions such as Parkinson’s disease, Alzheimer’s, depression, or chronic stress.
- People with endocrine disorders or obesity, which can alter hormonal balance and increase sebum production.
- Individuals with eating disorders, who may have nutritional deficiencies that affect skin health.
Additional Factors That May Aggravate Seborrheic Dermatitis
Skin injuries or trauma: Facial abrasions or irritation can trigger flare-ups.
Ultraviolet light exposure: Certain UV-based treatments (like PUVA therapy) applied to the face may worsen symptoms.
Climate: The condition tends to worsen in winter and early spring when humidity levels drop and temperatures are lower, but often improves in the summer.
Medications: Some drugs have been linked to seborrheic dermatitis flare-ups, including griseofulvin, cimetidine, lithium, methyldopa, arsenic compounds, haloperidol, and psoralen.
Cosmetic products: The use of skincare products or creams containing alcohol or irritating chemicals can damage the skin barrier and increase inflammation.

Diagnosis and Treatment of Seborrheic Dermatitis
Diagnostic Methods
1. Clinical Diagnosis
In Infants (Cradle Cap): Seborrheic dermatitis in infants often presents as cradle cap — greasy, yellowish scales that cover the scalp. The rash may spread to skin folds such as the armpits or groin, forming pink to orange patches that may flake or peel. Despite its extensive appearance, it typically causes little or no itching, so infants remain comfortable even when the rash spreads.
In Adults: Lesions usually appear as sharply demarcated, reddish plaques covered with fine or greasy scales, commonly affecting areas rich in sebaceous glands such as the face, scalp, chest, and interscapular region.
- Scalp: The earliest sign is dandruff—dry or oily flakes. As the condition progresses, inflammation develops around hair follicles, with redness extending to the forehead, behind the ears, external ear canals, and neck.
- Face: Red, scaly patches typically occur along the nasolabial folds and between the eyebrows.
- Trunk: Follicular papules with greasy scales appear on the chest and between the shoulder blades. When lesions merge, they form large plaques with a red border and thin central scales, resembling petals or rings.
- Skin Folds (axillae, under the breasts, groin, genital and anal regions): Lesions resemble intertrigo — sharply bordered, red areas covered with greasy scales.
2. Laboratory and Histopathological Tests
Histopathology: Non-specific findings include parakeratosis, mild acanthosis, and slight spongiosis (intraepidermal edema). The presence of spongiosis helps differentiate seborrheic dermatitis from psoriasis.
Inflammatory Infiltrate: Mild perivascular infiltration of inflammatory cells in the dermis.
Direct Microscopy: Detection of Malassezia furfur (yeast) confirms fungal involvement.
HIV Testing: Recommended for adults with severe, recurrent, or treatment-resistant seborrheic dermatitis, as it may indicate immunodeficiency.
3. Differential Diagnosis
It is important to distinguish seborrheic dermatitis from other skin conditions that present with scaling and erythema:
Psoriasis: Characterized by thick, silvery scales on well-demarcated red plaques, typically on pressure areas such as elbows and knees. Histopathology helps confirm diagnosis.
Contact Dermatitis or Irritant Reactions: Can mimic seborrheic dermatitis but often have a clear trigger or exposure history.
Lupus Erythematosus or Photosensitive Dermatitis: Require differentiation based on distribution, histology, and serologic tests.
Treatment of Seborrheic Dermatitis
General Principles
Antifungal therapy is the cornerstone of treatment, targeting Malassezia overgrowth.
Corticosteroid creams should be used sparingly or avoided for long-term use due to risk of skin atrophy and rebound flares.
Relapse is common, often triggered by alcohol consumption, stress, or certain medications.
Maintenance therapy is essential for chronic cases to prevent recurrence.
Specific Treatment Approaches
1. Scalp Involvement (Dandruff):
Use antifungal shampoos regularly.
Shampoos containing zinc pyrithione or magnesium (0.5–2%) or pyrithione olamine (0.75–1%) are effective with prolonged use.
Selenium sulfide (1–2.5%) or imidazole antifungals such as ketoconazole, bifonazole, or econazole are also beneficial.
Rotate active ingredients to prevent resistance and maintain efficacy.
2. Facial and Body Lesions:
Use 2% zinc pyrithione (ZnP) soaps or cleansers to reduce sebum and yeast colonization.
Apply topical antifungal creams containing ketoconazole, ciclopirox olamine, or bifonazole.
Avoid oily or alcohol-based skincare products that may worsen inflammation.
3. Systemic Therapy (for Severe or Refractory Cases):
Isotretinoin may be prescribed to reduce sebum production (0.5 mg/kg/day for at least 8 months).
Monitor lipid levels and liver function during treatment.
4. Infants (Cradle Cap and Leiner–Moussous Syndrome):
The condition often resolves spontaneously by age 3–4.
Prevent secondary infections with antifungal soaps (triclocarban, chlorhexidine) or imidazole creams.
To soften thick scales on the scalp, apply 5% salicylic acid ointment or mild antibiotic ointments if secondary infection is present.
For widespread lesions, oral ketoconazole may be indicated under medical supervision.
Lifestyle and Prevention of Seborrheic Dermatitis
Healthy Habits to Control Seborrheic Dermatitis
Daily Lifestyle Tips:
Follow your doctor’s treatment plan consistently, including prescribed topical or oral medications.
Maintain a positive mindset and manage emotional or physical stress, as stress is a known trigger for flare-ups.
Practice good personal hygiene and protect your skin from external irritants. Always use gentle cleansers and lukewarm water.
Avoid prolonged sun exposure—while limited sunlight may be beneficial, excessive UV exposure can worsen inflammation or trigger irritation.
Limit the use of cosmetics and skincare products during active flare-ups, especially those containing alcohol, fragrance, or harsh chemicals.
Ensure proper scalp care: wash your hair regularly with mild or medicated shampoos to prevent oil buildup and yeast overgrowth.
Dietary Recommendations for Healthier Skin
Eat plenty of water-rich vegetables and fruits, such as leafy greens, cucumbers, oranges, and berries, to keep your skin hydrated and nourished.
Include foods rich in omega-3 fatty acids (salmon, walnuts, flaxseeds) to help regulate sebum production and reduce inflammation.
Choose whole grains, lean proteins, and probiotic-rich foods (yogurt, kefir) to support gut and immune health.
Stay well-hydrated—drink sufficient water throughout the day.

Effective Ways to Prevent Seborrheic Dermatitis
Exercise regularly: Improves blood circulation, supports detoxification, and enhances skin regeneration.
Avoid excessive sunlight: Use sunscreen or protective clothing when outdoors.
Follow a balanced, anti-inflammatory diet: Incorporate foods high in vitamins A, C, and E, as well as beta-carotene, to strengthen the skin’s protective barrier and reduce oxidative stress.
Avoid triggering foods such as seafood, beef, spicy dishes, or foods high in sodium, which can worsen itching and oil production.
Limit alcohol and caffeine, as they can dehydrate the skin and trigger flare-ups.
Maintain gentle skincare hygiene:
- Bathe regularly using mild, fragrance-free cleansers.
- Avoid scrubbing affected areas aggressively.
- Choose hypoallergenic moisturizers formulated for sensitive or oily skin.
