Scabies: Symptoms, Causes, and Treatment
Overview of Scabies
Scabies is characterized by intense itching caused by an infestation of the skin by the human itch mite Sarcoptes scabiei. The female mites burrow into the outer layer of the skin to lay eggs, leading to severe itching, especially at night.
Scabies is highly contagious and can spread rapidly in close-contact environments such as households, childcare centers, schools, nursing homes, or prisons. Because of its high transmission rate, it is essential to limit close contact with infected individuals until they have completed treatment.
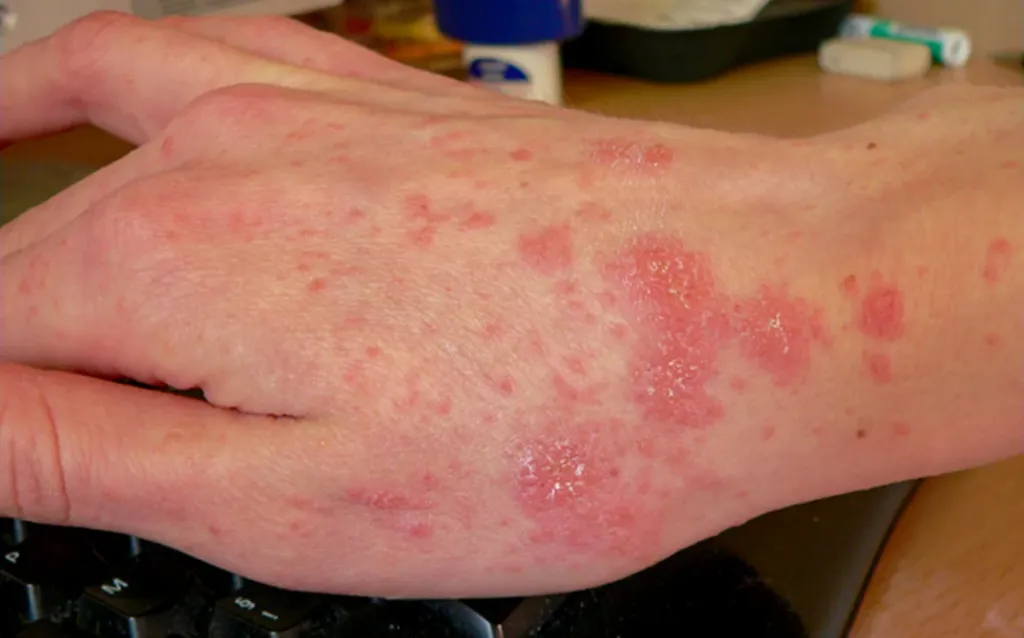
Symptoms of Scabies
Common signs and symptoms include:
- Severe itching, often worsening at night.
- Thin, irregular burrow tracks formed by tiny blisters or raised bumps on the skin.
- Wavy lines or scaly lesions measuring a few millimeters to 1 cm, most commonly found in skin folds.
In adults and older children, burrows are typically located in:
- Between the fingers
- Armpits
- Around the waist
- Inner wrists
- Inner elbows
- Soles of the feet
- Around the nipples (in women)
- Around the male genital area
- Buttocks
- Knees
In infants and young children, affected areas may also include:
- Scalp
- Palms of the hands
- Soles of the feet
When to See a Doctor
Causes of Scabies
Scabies is caused by a parasitic mite known as Sarcoptes scabiei. These microscopic mites burrow into the outer layer of the skin (epidermis), where they create tunnels, lay eggs, and trigger an intense allergic reaction that leads to severe itching.
Risk Factors
Who is at risk of scabies?
Scabies can affect anyone regardless of age, gender, or living conditions. However, the risk of infection is higher among individuals who have close physical contact with an infected person or share personal items such as clothing, bedding, blankets, or towels.
Factors that increase the risk of scabies
Several factors may increase the likelihood of developing scabies, including:
- Living in a household with many children
- Low-income or limited access to healthcare
- Crowded living environments with poor hygiene
- Poor personal hygiene or infrequent bathing
- Weakened immune system or severe malnutrition
- Keeping pets without proper grooming or hygiene

Diagnosis and Treatment of Scabies
Diagnostic Methods
The diagnosis of scabies is primarily based on clinical findings, especially the presence of burrows on the skin and intense itching that seems disproportionate to the visible skin lesions. Diagnosis is also supported when similar symptoms appear among close contacts of the patient.
The gold standard for diagnosis is the identification of the mite, its eggs, or fecal pellets (scybala) under a microscope from skin scrapings collected from burrows. Additional diagnostic tools include:
- Dermoscopy – a handheld skin magnification device that can detect burrows and mite activity
- Polymerase Chain Reaction (PCR) – detects Sarcoptes scabiei DNA from skin flakes
In many cases, mites may not be found even with testing. Therefore, diagnosis often relies heavily on clinical presentation and epidemiological factors.
Effective Treatment Options for Scabies
The primary treatment for scabies involves topical or oral scabicidal medications (anti-mite therapy).
1. Permethrin
First-line topical treatment
Adults and older children: Apply permethrin cream over the entire body from the neck down, leave on for 8–14 hours, then rinse; repeat after 7 days
Infants and young children: Apply to the head and neck as well, avoiding the eyes and mouth. Pay special attention to fingers, toes, nails, and navel. Infants should wear gloves to prevent ingestion
Lindane may be used as an alternative but is less preferred due to neurotoxicity risk; contraindicated in children under 2 years or patients with seizure disorders
2. Spinosad 0.9% Topical Suspension
- Approved for adults and children over 4 years
- Apply to the entire body from the neck down, including soles of the feet
- In bald patients, also apply to the scalp and hairline
- Allow to dry for 10 minutes before dressing; leave on for 6 hours before washing off
- Use once weekly for 1 week
3. Precipitated Sulfur 6–10% in Petrolatum
- Safe and effective, especially for infants under 2 months of age
- Apply over the entire body and leave on for 24 hours, repeated daily for 3 consecutive days
4. Ivermectin (Oral Therapy)
Recommended for patients who:
- Fail topical treatment
- Cannot comply with topical regimens
- Have immunosuppression or Norwegian (crusted) scabies
Typically given as a single dose and repeated after 7–14 days
5. Symptomatic Relief
Topical corticosteroids and oral antihistamines (e.g., Hydroxyzine 25 mg, 4 times daily) help relieve itching
Secondary bacterial infections (e.g., honey-colored crusts or oozing lesions) should be treated with appropriate topical or systemic antibiotics targeting Staphylococcus species
Treatment Considerations
Symptoms such as itching and skin lesions may take up to 3 weeks to fully resolve, even after successful treatment. Reasons for treatment failure include drug resistance, improper application, reinfestation, or hidden burrows. In persistent cases, repeat skin scrapings may be necessary to confirm ongoing infestation.
Lifestyle Modifications & Prevention of Scabies
Healthy Habits to Support Treatment and Prevent Recurrence
Follow medical treatment as prescribed by your doctor, including topical creams or oral medications.
Maintain good personal hygiene to limit the spread and reinfestation of mites.
Avoid scratching intensely to prevent secondary skin infections.
Trim nails short and keep them clean to reduce the risk of spreading mites to other body areas.
Wash personal items such as towels, clothes, bed sheets, and pillowcases in hot water (≥ 60°C) and dry on high heat.
Clean and disinfect living spaces regularly, especially bedding and frequently touched surfaces.
Isolate potentially contaminated items in sealed plastic bags for at least 3 days if washing is not possible.
Seek medical advice promptly if itching persists after treatment or if new rashes appear.
Schedule medical follow-ups to monitor treatment response and prevent recurrence.
Maintain a healthy mental state during treatment; itching may affect sleep and quality of life. Mental relaxation helps improve recovery.
Nutrition Recommendations
Consume foods that boost immunity, such as fruits, vegetables, lean protein, and whole grains.
Drink enough water to support skin health.
Limit sugary and highly processed foods that may aggravate skin inflammation.
Effective Prevention Methods for Scabies
To reduce the risk of infestation and prevent outbreaks in families or communities:
| Prevention Tips | Description |
| Maintain personal hygiene | Shower daily, keep nails clean, change clothes frequently |
| Avoid sharing personal items | Do not share towels, bedding, pillows, or clothing |
| Early treatment | Treat infected individuals promptly to prevent spread |
| Treat close contacts | Household members or people with close skin contact should also be treated |
| Wash fabrics properly | Use hot water and high-heat drying |
| Sun exposure for fabrics | Sunlight helps kill mites |
| Clean living spaces | Vacuum mattresses, carpets, and sofas |

