Psoriasis: Symptoms, Causes, Diagnosis, and Prevention
What Is Psoriasis?
Psoriasis is a chronic autoimmune skin disorder in which skin cells multiply up to 10 times faster than normal, leading to a buildup of thick, scaly plaques. These patches are typically pink or red on lighter skin tones and purple or dark brown on darker skin, often topped with white, gray, or silvery scales. The most common areas affected include the elbows, knees, scalp, and lower back.
While psoriasis can develop at any age, it most often appears between ages 20–30 and again between ages 50–60, affecting men and women equally. In mild cases, only small patches of skin are involved, but severe psoriasis can be painful, itchy, and widespread.
According to the International Classification of Diseases (ICD-10), psoriasis is classified under the code L40, with specific subtypes assigned additional codes (such as plaque psoriasis, pustular psoriasis, and psoriatic arthritis).
Common Signs and Symptoms
Typical symptoms of psoriasis include:
- Patchy rashes of varying shapes and sizes, ranging from small flakes resembling dandruff to large lesions covering wide areas.
- Color variations depending on skin tone — reddish-pink on fair skin, purplish or dark brown on darker tones, often with silvery scaling.
- Small scaly spots, more common in children.
- Dry, cracked skin that may bleed.
- Itching, burning, or soreness around affected areas.
- Cyclic flare-ups — symptoms may worsen for weeks or months, then subside before recurring.
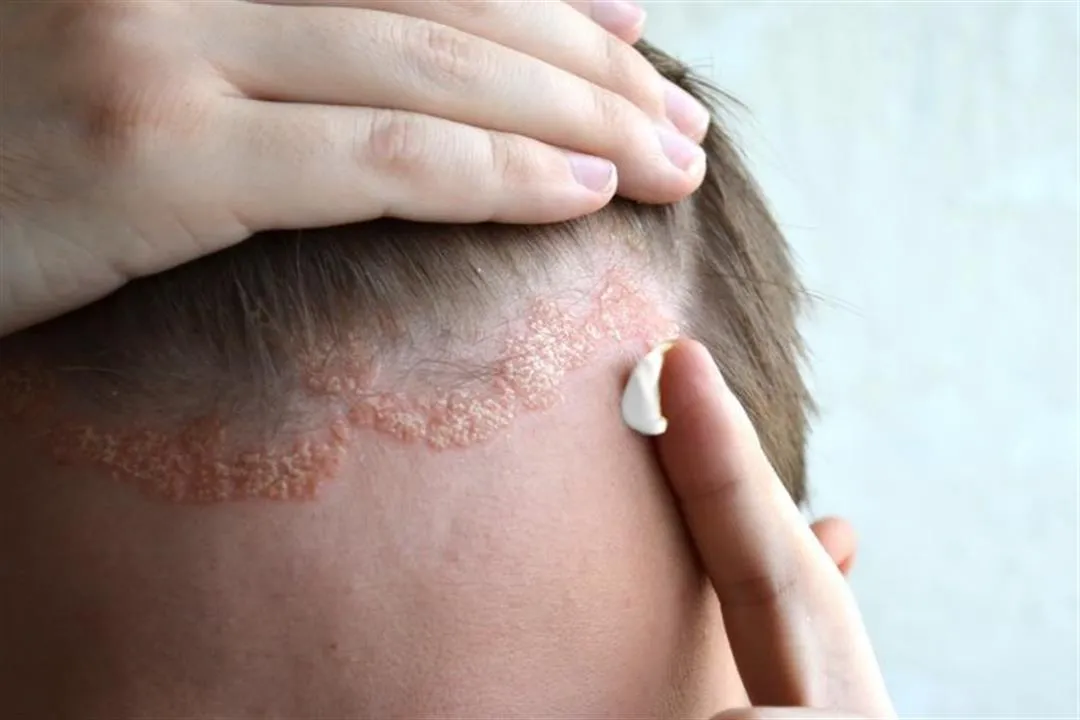
Major Types of Psoriasis
Dermatologists classify psoriasis into several clinical subtypes, each with distinct features and triggers:
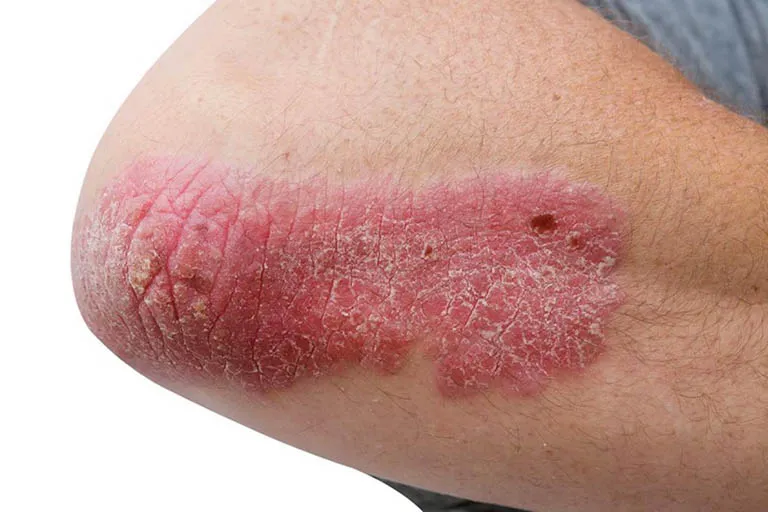
1. Plaque Psoriasis (Psoriasis Vulgaris): This is the most common type, accounting for about 90% of all cases. It manifests as raised, inflamed patches of red skin covered with silvery-white scales, typically found on the elbows, knees, lower back, and scalp. The severity and coloration of plaques may vary depending on skin type and environmental factors.
2. Guttate Psoriasis: Characterized by small, drop-shaped lesions scattered on the torso, arms, or legs. It primarily affects children and young adults and is often triggered by bacterial infections, especially streptococcal throat infections. Symptoms typically appear 1–3 weeks after infection.
3. Pustular Psoriasis: A rare but severe form, presenting as noninfectious pustules (blisters filled with sterile pus). These can appear in localized areas such as the palms or soles, or spread more widely across the body. The condition can develop rapidly and may require urgent medical attention.
4. Inverse (Flexural) Psoriasis: Found in skin folds such as the armpits, groin, under the breasts, and around the genitals. It appears as smooth, shiny, red patches that worsen with friction, sweating, or heat. This type is often aggravated by fungal infections or skin irritation.
5. Erythrodermic Psoriasis: A rare but potentially life-threatening form that can cover over 90% of the body surface. The skin becomes bright red, scaly, itchy, and severely painful. This form can develop suddenly or as a progression from another psoriasis type. Hospitalization is sometimes necessary to restore fluid balance and prevent infection.
6. Nail Psoriasis: Causes pitting, thickening, discoloration, or crumbling of the nails. In severe cases, the nail may detach from the nail bed — a condition that can resemble a fungal infection (onychomycosis).
7. Infantile (Diaper) Psoriasis: Appears in infants as red, scaly patches in the diaper area, sometimes extending to the torso or limbs. It may be mistaken for common diaper rash but tends to persist longer and requires dermatological evaluation.
8. Oral Psoriasis: A very rare type, presenting as white or grayish patches inside the mouth or on the tongue. Some patients develop fissured tongue, which is often asymptomatic but may accompany other psoriasis forms.
9. Seborrheic Psoriasis (Sebopsoriasis): This hybrid condition shares features of both psoriasis and seborrheic dermatitis. It causes oily, red, flaky patches in areas rich in sebaceous glands — such as the scalp, forehead, nasolabial folds, chest, and upper back.
Causes of Psoriasis
Psoriasis occurs when skin cells regenerate much faster than normal. Under typical conditions, the skin renews itself about once every 3–4 weeks. In individuals with psoriasis, this process accelerates drastically, taking only 3–7 days. As a result, new skin cells accumulate before the old ones can shed, forming thick, scaly plaques that characterize the disease.
Scientific research indicates that psoriasis is primarily an immune-mediated disorder. Normally, the immune system protects the body from infection and disease. However, in psoriasis, the immune system mistakenly targets healthy skin cells, releasing inflammatory chemicals such as cytokines (e.g., TNF-α, IL-17, IL-23) that drive rapid cell turnover and inflammation.
Genetics also play a key role. About one-third of people with psoriasis have a family history of the condition. Studies of identical twins show that if one twin has psoriasis, the other has about a 70% chance of developing it, compared with only 20% among non-identical twins — a clear indication that both genetic susceptibility and environmental triggers are involved.
Common triggers that may provoke or worsen psoriasis include:
- Skin injury (scratches, burns, or surgical scars — known as the Koebner phenomenon).
- Throat infections, especially those caused by Streptococcus bacteria.
- Certain medications, such as beta-blockers, lithium, antimalarial drugs, or corticosteroid withdrawal.
- Stress, cold weather, alcohol consumption, and smoking, all of which can exacerbate inflammation.
Who Is at Risk?
Psoriasis affects an estimated 2–3% of the global population, though its prevalence varies by age, ethnicity, and geography. It can appear at any age but most commonly begins before the age of 20 or during early adulthood.
Risk factors include:
- Ethnicity: Psoriasis is more prevalent among Caucasians compared to Asian populations.
- Family history: A strong hereditary component increases the likelihood of developing the disease.
- Autoimmune conditions: Individuals with inflammatory bowel diseases such as Crohn’s disease or ulcerative colitis are at higher risk.
- Metabolic health: There is a strong association between psoriasis and obesity, type 2 diabetes, and metabolic syndrome.
- Cardiovascular disease: Chronic systemic inflammation in psoriasis contributes to hypertension, atherosclerosis, and heart disease.
Possible Complications
While psoriasis is common, it remains challenging to manage, and chronic inflammation can lead to several long-term complications:
Physical and psychological distress: Persistent itching, pain, and discomfort may cause sleep disturbances, difficulty concentrating, and reduced quality of life. Psoriasis often follows a cyclic pattern — flaring for weeks or months before improving temporarily.
Economic and treatment burden: Advances in modern medicine have introduced biologic therapies that specifically target immune pathways (like TNF or IL-17 inhibitors). These drugs are highly effective but costly, limiting access for many patients.
Psoriatic arthritis: About 30% of patients develop this inflammatory joint condition, which can cause swelling, stiffness, and potential joint damage if untreated.
Other associated conditions: Psoriasis is linked to a higher risk of lymphoma, cardiovascular disease, Crohn’s disease, and depression.
Metabolic disorders: Young individuals with psoriasis are more likely to develop type 2 diabetes, and studies suggest that people with psoriasis have a 58% higher risk of developing high blood pressure compared with those without the disease.
Diagnosis of Psoriasis
A dermatologist can usually diagnose psoriasis based on clinical examination alone, as the condition presents with very distinctive skin lesions. Typical findings include raised red plaques covered with silvery-white scales, itching or pain, and the classic Auspitz sign — pinpoint bleeding that appears when scales are scraped off. Because of these characteristic features, blood tests are rarely necessary for diagnosis.
In certain cases, however, additional tests may be performed to rule out similar conditions. For example, when joint pain or swelling is present, doctors may order X-rays or blood tests to differentiate psoriatic arthritis from rheumatoid arthritis. If uncertainty remains, a skin biopsy — removing a small sample of affected skin for microscopic examination — can confirm the diagnosis by revealing the hallmark histopathological features of psoriasis.
When psoriatic arthritis is suspected, dermatologists often collaborate with rheumatologists to manage both the skin and joint symptoms effectively.
Conditions That Can Mimic Psoriasis
Psoriasis can sometimes resemble other chronic skin disorders, leading to diagnostic confusion, particularly in early or atypical cases. Differential diagnoses may include:
- Discoid eczema (nummular dermatitis)
- Seborrheic dermatitis
- Pityriasis rosea
- Tinea (fungal) infections, especially nail fungus (onychomycosis)
- Cutaneous T-cell lymphoma, a rare form of skin cancer
- Secondary syphilis, which can also present with a generalized rash
Proper evaluation by a dermatologist is essential to distinguish psoriasis from these conditions and guide appropriate treatment.
Treatment Options for Psoriasis
Like other chronic inflammatory conditions, psoriasis requires long-term management rather than a one-time cure. The goal of therapy is to control flare-ups, relieve symptoms, and improve quality of life. Modern dermatology offers a range of effective treatments, from topical creams to advanced biologic therapies.
1. Topical Treatments
For mild to moderate psoriasis, dermatologists usually start with topical therapies applied directly to the affected skin. These include:
- Corticosteroid creams or ointments to reduce inflammation and itching.
- Vitamin D analogs (such as calcipotriol or calcitriol) to slow skin cell growth.
- Coal tar preparations, salicylic acid, or emollients to soften thickened plaques.
These treatments are safe and effective for localized disease but may not be sufficient for more extensive or resistant cases.
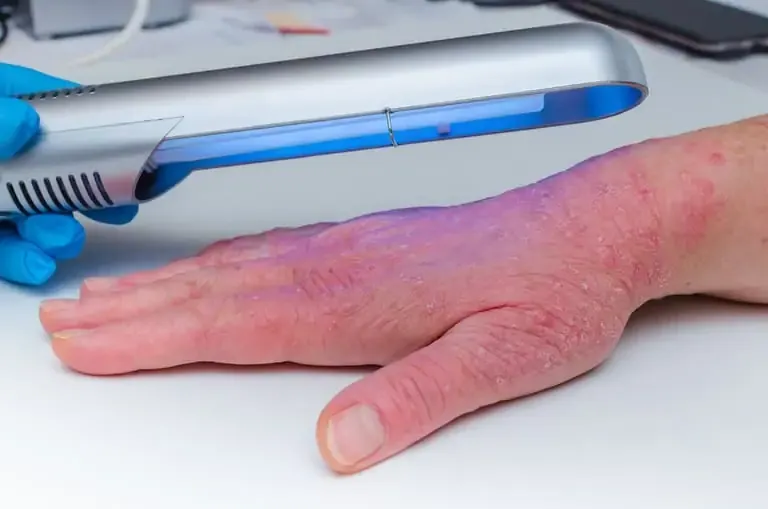
2. Phototherapy (Light Therapy)
If topical medications are inadequate, phototherapy may be recommended. This involves controlled exposure to ultraviolet (UV) light, particularly UVB or PUVA therapy (psoralen plus UVA), under medical supervision. Regular sessions can slow down the overproduction of skin cells and improve scaling and redness.
3. Systemic Medications
For moderate to severe psoriasis, or when light therapy fails, systemic treatments that act throughout the body are prescribed. These include:
- Methotrexate – suppresses immune activity and reduces inflammation.
- Cyclosporine – a potent immunosuppressant for short-term control.
- Acitretin – an oral retinoid that normalizes skin cell growth.
These drugs require careful monitoring due to potential side effects involving the liver, kidneys, or immune system.
4. Biologic Therapies
In recent years, biologic agents have revolutionized psoriasis management. These medications are engineered proteins that precisely target specific immune pathways, such as TNF-α, IL-17, IL-12/23, or IL-23 — cytokines responsible for driving inflammation in psoriasis.
Unlike traditional systemic drugs that broadly suppress the immune system, biologics act selectively, offering high efficacy and long-term safety for patients with moderate to severe psoriasis. Examples include:
- Adalimumab (Humira®)
- Secukinumab (Cosentyx®)
- Ustekinumab (Stelara®)
- Ixekizumab (Taltz®)
While biologics have shown impressive results, they come with high costs and a potential increased risk of infections, since they dampen immune responses. Regular medical follow-up and screening for tuberculosis or hepatitis are required before and during treatment.
Prevention and Lifestyle Management for Psoriasis
While psoriasis cannot be completely cured, maintaining a healthy lifestyle and consistent skin care routine can significantly help control flare-ups and slow disease progression. Below are key preventive strategies and self-care tips for different groups of individuals:
1. For People Without Psoriasis
Building a strong immune system is essential. Prioritize balanced nutrition, regular exercise, and adequate sleep. Prevent infections and skin injuries such as cuts, burns, or scrapes, as these may trigger psoriasis in genetically susceptible individuals — a phenomenon known as the Koebner response.
2. For High-Risk Individuals
Those with a family history of psoriasis should undergo regular skin evaluations and seek early medical consultation at the first sign of symptoms. Early detection enables timely treatment, preventing the condition from becoming severe or systemic.
3. For People Living with Psoriasis
If you already have psoriasis, avoid panic or excessive anxiety. Instead, maintain open communication with your dermatologist to discuss appropriate treatment plans and monitor for potential complications such as psoriatic arthritis or secondary infections.
Follow your doctor’s instructions carefully when using prescribed medications. Additionally:
- Avoid excessive sun exposure and always apply sunscreen.
- Keep your skin clean and moisturized to prevent dryness and cracking.
- Refrain from alcohol and smoking, both of which can worsen inflammation.
- Limit high-fat, processed, and fried foods.
- Incorporate anti-inflammatory nutrients like folic acid and omega-3 fatty acids found in fish such as salmon, mackerel, and sardines.

Frequently Asked Questions
1. Is Psoriasis Dangerous?
Although psoriasis itself is not contagious, it can have serious health and psychological consequences. Patients face a higher risk of:
- Skin infections due to cracks and lesions.
- Joint inflammation (psoriatic arthritis) causing pain and stiffness.
- Celiac disease, non-melanoma skin cancers, and squamous cell carcinoma.
- Emotional distress, including depression, anxiety, and social withdrawal.
- People with HIV/AIDS tend to develop more severe and extensive lesions.
Long-term systemic therapy, while beneficial, may slightly increase the risk of certain malignancies. Research has shown:
- 52% higher risk of lung and bronchial cancer.
- 205% higher risk of upper gastrointestinal cancers.
- 90% increased risk of liver cancer.
- 46% increased risk of pancreatic cancer.
These figures emphasize the need for medical supervision, lifestyle moderation, and regular cancer screening for those on prolonged immunosuppressive treatment.
2. What Foods Should Be Avoided with Psoriasis?
Diet plays a supporting role in managing psoriasis. A balanced, anti-inflammatory diet may help reduce flare-ups and improve treatment outcomes.
Recommended foods include:
- Fish rich in EPA and DHA (e.g., salmon, sardines, mackerel).
- Olive oil, legumes, leafy greens, fruits, and whole grains.
- Probiotics and vitamin D supplements to support immune health.
Foods to limit or avoid:
- Processed meats, red meat, and full-fat dairy containing saturated fats.
- Alcohol and high-calorie foods, which worsen inflammation.
- Nightshade vegetables such as tomatoes, eggplants, peppers, and white potatoes, which may trigger flares in some individuals.
- Caffeine, refined sugars, and tobacco.
Patients with celiac disease or those with anti-gliadin antibodies may benefit from a gluten-free diet, which can reduce disease severity and improve skin health.
3. When Should You See a Doctor?
You should schedule a consultation with a dermatologist if you:
- Notice persistent or spreading rashes suggestive of psoriasis.
- Experience pain, itching, or discomfort interfering with daily activities.
- Feel emotionally distressed or self-conscious about your skin condition.
- Have been treated for psoriasis but see little or no improvement.
Early and ongoing medical care not only helps control flare-ups but also prevents joint damage and systemic complications associated with advanced psoriasis.
