What Is Hair Loss? Causes, Treatment Options, and Prevention Principles
Understanding Hair Loss
Definition
Hair loss refers to a condition in which hair growth is reduced or interrupted, resulting in more hair falling out than being produced.
Hair grows in cycles, and each cycle consists of three main phases:
- Anagen (Growth phase): The active growing period lasting 2–6 years.
- Catagen (Transition phase): A short transitional period lasting about 3 weeks, during which hair growth slows and follicles shrink.
- Telogen (Resting phase): A resting phase lasting 2–3 months before the hair naturally falls out (exogen phase).
Normally, about 50–100 hairs fall out daily as part of the natural growth cycle. Once a hair sheds, a new one begins to grow from the same follicle, restarting the cycle.
Two major types of growth cycle disturbances can occur:
- Anagen effluvium: Sudden interruption of the growth phase, often triggered by chemotherapy, radiation, or toxins, leading to abrupt hair loss.
- Telogen effluvium: Excessive shedding of more than 100 hairs per day when many hairs prematurely enter the resting phase. This is commonly associated with stress, hormonal changes, illness, or nutritional deficiencies.

Classification of Hair Loss
By Pattern
- Localized hair loss: Occurs in one or several distinct areas.
- Diffuse hair loss: Hair thinning is widespread across the scalp.
By Follicular Damage
Cicatricial (Scarring) alopecia: Results from the destruction of hair follicles, which are replaced by scar tissue. Once the follicles are destroyed, regrowth is impossible. Causes may include inflammatory or autoimmune skin diseases such as lupus erythematosus or lichen planopilaris.
- Primary scarring alopecia: Inflammation directly targets hair follicles.
- Secondary scarring alopecia: Follicles are destroyed by non-specific inflammatory reactions, burns, or infections.
Non-cicatricial (Non-scarring) alopecia: Hair loss occurs without permanent follicle damage. Hair may regrow if the underlying cause is treated. Conditions such as androgenetic alopecia, telogen effluvium, or trichotillomania fall into this category.
Symptoms of Hair Loss
Common signs and symptoms include:
- Excessive hair shedding (more than 100 hairs per day), especially noticeable after sleeping, washing, or brushing the hair.
- New hair growth (baby hairs) appears thin, weak, or absent.
- Thinning hair that reveals more of the scalp, especially in women.
- Patchy bald spots or receding hairlines, more common in men.
When to See a Doctor
You should consult a dermatologist or healthcare professional if you experience:
- Sudden or patchy hair loss.
- Hair shedding accompanied by scalp itching, redness, or scaling.
- Hair loss following illness, childbirth, or major stress.
- Hair not regrowing after several months.
Causes of Hair Loss
Common Causes
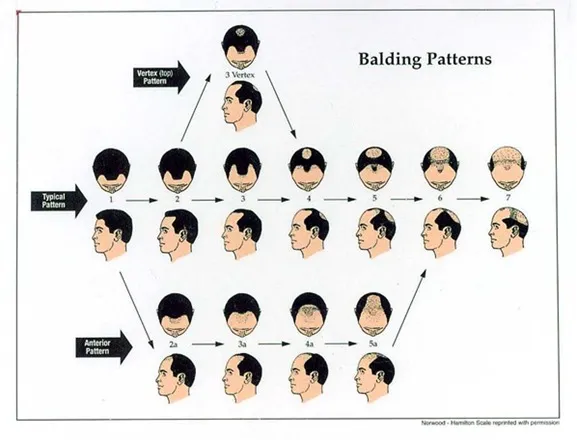
The most common cause of hair loss is androgenetic alopecia — also known as male-pattern or female-pattern baldness.
This condition is a hereditary disorder influenced by androgen hormones, particularly dihydrotestosterone (DHT). DHT shortens the hair growth phase and gradually causes miniaturization of hair follicles, leading to thinner and shorter hair.
The prevalence of androgenetic alopecia increases with age and affects:
- Over 70% of men (male-pattern hair loss)
- Up to 50% of women (female-pattern hair loss) by the age of 80
It tends to be less common among Asian, Black, and Chinese populations compared with individuals of European descent.
Other Common Causes
Medications: Certain drugs, including chemotherapy agents, anticoagulants, antidepressants, and retinoids, can trigger hair shedding.
Infections: Fungal infections of the scalp (tinea capitis) or bacterial infections like kerion can damage hair follicles.
Systemic disorders: Autoimmune diseases such as systemic lupus erythematosus, prolonged fever, nutritional deficiencies (iron, zinc, vitamin D, or protein), and endocrine imbalances (thyroid disorders) can all lead to hair loss.
Alopecia areata: An autoimmune condition in which the immune system attacks hair follicles, causing patchy bald spots.
Physical or mechanical damage: Includes traction alopecia (from tight hairstyles), trichotillomania (hair-pulling disorder), burns, radiation exposure, or hair loss triggered by severe stress or surgery (telogen effluvium).
Less Common Causes
Hair shaft abnormalities: Fragile hair shafts that break easily, as seen in trichorrhexis nodosa or monilethrix.
Autoimmune diseases: Conditions like thyroiditis or vitiligo may be associated with hair loss.
Heavy metal toxicity: Exposure to mercury, thallium, or arsenic can damage hair follicles.
Rare dermatological conditions: Such as dissecting cellulitis of the scalp, which predominantly affects men of African descent and leads to scarring alopecia.
Risk Factors for Hair Loss
Who Is at Risk?
Hair loss can affect anyone, regardless of age or gender. However, it is more common in men and in older adults.
Factors That Increase Risk
Certain factors may increase your likelihood of experiencing hair loss:
- Family history: A genetic predisposition to androgenetic alopecia.
- Aging: Hair growth slows naturally with age.
- Significant weight loss: Especially due to restrictive diets or illness.
- Chronic health conditions: Such as diabetes or systemic lupus erythematosus.
- Stress: Both emotional and physical stress can disrupt the hair growth cycle.
- Poor nutrition: Inadequate intake of protein, iron, or essential vitamins and minerals can weaken hair growth.

Diagnosis and Treatment of Hair Loss
Diagnostic Evaluation
Medical History
A detailed medical history is essential to identify the underlying cause of hair loss. The physician should inquire about:
Onset and duration: When hair loss began, how long it has persisted, whether it is worsening, and whether it is localized or diffuse.
Associated symptoms: Presence of itching, scaling, or redness.
Hair care habits: Use of hair dyes, heat styling, rollers, or tight hairstyles that may cause traction alopecia.
Exposure and stressors: Recent exposure to toxins (drugs, radiation, chemicals), physical or emotional stress, surgery, chronic illness, or high fever.
Systemic symptoms: Fatigue, cold intolerance (suggesting hypothyroidism); voice deepening, excessive hair growth, or increased libido (indicating androgen excess).
Weight loss, restrictive dieting, or compulsive behaviors (e.g., trichotillomania, substance abuse).
Family history: Any relatives with hair loss.
For female patients, a gynecologic and endocrine history should be obtained, including menstrual and obstetric details.
Physical Examination
Scalp examination: Assess the pattern and extent of hair loss, measure the width of thinning areas, note the presence of scarring, and inspect for inflammatory lesions or scaling.
General skin examination: Evaluate for hair loss in other body areas (eyebrows, eyelashes, limbs). Check for associated rashes that might suggest discoid lupus erythematosus, secondary syphilis, or fungal/bacterial infections.
Signs of virilization in women: Acne, hirsutism, deepened voice, or clitoral enlargement.
Examine for systemic signs of underlying disorders and palpate the thyroid gland for abnormalities.
Laboratory and Diagnostic Tests
Laboratory investigations are guided by clinical suspicion and may include endocrine, autoimmune, or toxicology tests.
Androgenetic alopecia usually requires no laboratory testing. However, if there is no family history, inquire about anabolic steroid use or medications.
In women with diffuse hair loss and signs of androgen excess, measure serum testosterone and dehydroepiandrosterone sulfate (DHEAS) levels.
Specific diagnostic tests include:
Hair pull test: Gently pull about 40 hairs from different areas of the scalp and count the number that come out. Normally, fewer than 3 telogen hairs are released per pull. If more than 4–6 hairs are pulled out, the test is positive, suggesting telogen effluvium.
Hair pluck (trichogram): About 50 hairs are forcibly removed and examined microscopically to determine the proportion of hairs in each growth phase and identify abnormalities in the anagen or telogen phase.
Scalp biopsy: Recommended when the diagnosis is uncertain or when scarring alopecia is suspected. Biopsies should be taken from active inflammatory areas at the margin of bald patches. Samples may also be cultured for fungi or bacteria.
Daily hair count: Patients can collect shed hairs during washing or combing over 14 days. A count exceeding 100 hairs per day is abnormal, except immediately after shampooing.
Treatment Options for Hair Loss
Medications
Minoxidil
- Dosage: Apply 1 mL of topical solution (2% for women, 2–5% for men) twice daily to the scalp.
- Mechanism: The exact mechanism is unclear but thought to increase blood flow and prolong the anagen phase.
- Effectiveness: Most effective for vertex (crown) hair loss in both sexes. Noticeable regrowth may take 8–12 months, and continuous use is required to maintain results.
- Side effects: Mild scalp irritation, allergic contact dermatitis, and increased facial hair growth (especially in women).
Finasteride
- Mechanism: A 5-alpha-reductase inhibitor that prevents conversion of testosterone to dihydrotestosterone (DHT), reducing follicular miniaturization.
- Dosage: 1 mg orally once daily. Results typically appear after 6–8 months of treatment.
- Side effects: Decreased libido, erectile dysfunction, and ejaculation disorders, which may persist after discontinuation; gynecomastia and hypersensitivity reactions.
- Finasteride can lower prostate-specific antigen (PSA) levels, which may affect prostate cancer screening in older men.
- Off-label use in women of reproductive age may be considered under strict medical supervision, but it is contraindicated in pregnancy due to risk of teratogenicity.
Dutasteride
- A stronger 5-alpha-reductase inhibitor than finasteride, primarily used for benign prostatic hyperplasia but occasionally prescribed off-label for androgenetic alopecia.
Hormonal Therapy (for Women)
- Oral contraceptives or spironolactone may help reduce androgen levels and slow hair loss in women.
Non-Pharmacological Treatments
Low-level laser therapy (LLLT): Stimulates hair follicles, enhances microcirculation, and may promote new hair growth.
Platelet-rich plasma (PRP) therapy: Involves injecting concentrated platelets rich in growth factors into the scalp to stimulate follicle regeneration.
Hair transplantation: Includes follicular unit transplantation (FUT) or follicular unit extraction (FUE), scalp reduction, and flap surgeries in severe cases.
Treating Underlying Causes
Alopecia areata: Treated with topical, intralesional, or systemic corticosteroids depending on severity; other options include topical minoxidil, anthralin, contact immunotherapy (DPCP or SADBE), or methotrexate.
Traction alopecia: Eliminate physical tension or traction on the scalp.
Tinea capitis: Requires systemic antifungal agents such as griseofulvin or terbinafine.
Trichotillomania: Managed with behavioral therapy and medications such as clomipramine or selective serotonin reuptake inhibitors (SSRIs).
Cicatricial alopecias (e.g., CCCA, dissecting cellulitis): Combination of oral tetracyclines and potent topical corticosteroids; intralesional triamcinolone for localized inflammation; topical retinoids or antibiotics for mild cases.
Lichen planopilaris, frontal fibrosing alopecia, and chronic cutaneous lupus: Treated with oral antimalarials, topical/intralesional corticosteroids, retinoids, topical tacrolimus, or systemic immunosuppressants.
Chemotherapy-induced (anagen effluvium): Usually temporary; hair often regrows after treatment cessation, sometimes with a different texture or color. Wearing a wig can help during the regrowth phase.
Telogen effluvium: Typically self-limiting and resolves once the triggering factor is removed.
Lifestyle & Prevention of Hair Loss
Daily Habits to Help Slow Hair Loss
Lifestyle:
Follow your doctor’s treatment plan carefully.
Maintain a positive mindset and reduce stress whenever possible.
Contact your physician promptly if you notice any unusual reactions during treatment.
Schedule regular check-ups to monitor your health status, disease progression, and allow your doctor to adjust treatment if necessary.
Wash your hair daily with a nourishing shampoo to reduce dryness and breakage.
Dietary Habits:
Incorporate plenty of fresh vegetables and herbs (such as parsley, basil, and lettuce) at least three times per week.
Eat a protein-rich diet including eggs, nuts, beans, fish, low-fat dairy products, and poultry.
Supplement with vitamin D (800–1000 IU per day) and consume foods high in vitamin A—like sweet potatoes, bell peppers, and spinach—to support hair growth.
Effective Ways to Prevent Hair Loss
To help prevent hair loss or minimize its severity, consider the following recommendations:
Wash your hair regularly with a gentle, nourishing shampoo.
Apply natural oils such as coconut oil or olive oil to help protect hair from damage caused by styling and ultraviolet (UV) exposure.
Avoid frequent use of heat-based styling tools (curlers, straighteners, blow dryers).
If you dye your hair, choose organic hair dyes or those free from ammonia, peroxide, and para-phenylenediamine (PPD) to reduce scalp irritation and hair shaft damage.
