Atopic Dermatitis – Overview, Causes and Prevention
What is Atopic Dermatitis?
General Understanding
Atopic dermatitis can affect individuals of all ages but is most common in infants and young children, particularly those under 2 years old. About 80% of affected children develop symptoms before age 6, and the disease may persist into adolescence and adulthood. Prevalence among young adults up to age 26 ranges from 5–15%.
It is estimated that more than 230 million people worldwide suffer from atopic dermatitis, and lifetime prevalence exceeds 15%. Although there is no definitive cure, proper treatment and self-care can significantly control symptoms and prevent flare-ups. Regular moisturizing, avoiding harsh soaps, and using medicated creams or ointments are essential components of management.
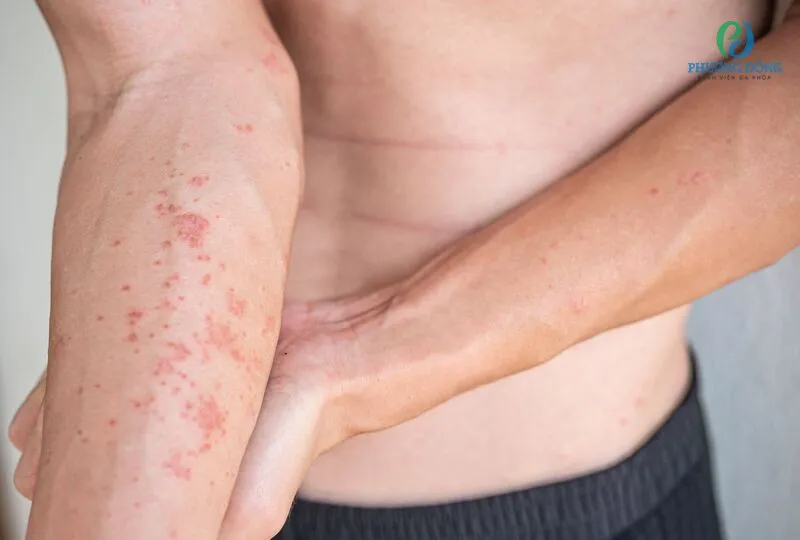
Symptoms of Atopic Dermatitis
Signs and Symptoms
In Infants (<2 years old)
Often begins between 2–3 months of age. Typical lesions progress through stages:
- Erythema (Redness) Stage: Skin becomes red, itchy, with tiny papules like millet seeds.
- Vesicular Stage: Small fluid-filled blisters cluster on inflamed skin.
- Oozing Stage: Blisters rupture, releasing fluid, forming “eczema wells,” with swelling and a high risk of secondary infection.
- Crusting Stage: Fluid dries into yellowish crusts; if infected, the crusts may thicken and turn brown.
- Desquamation Stage: Crusts peel, leaving thin fragile skin that gradually returns to normal.
Commonly affected areas include the cheeks, forehead, and chin, but lesions may also spread to the arms, legs, back, or abdomen, typically symmetrically.
In Children (2–12 years old)
Most frequent in children aged 2–5 years.
- Skin lesions appear as raised papules grouped into plaques or scattered.
- Chronic scratching causes thickened, rough skin (lichenification).
- Lesions commonly occur in flexural areas: the elbows, knees, wrists, eyelids, and often appear bilaterally.
In Adolescents and Adults
May persist from childhood or begin later in life.
- Characterized by papules and plaques, sometimes with small vesicles and excoriations due to itching.
- Lesions typically localize to skin folds: neck, elbow creases, knee folds, wrists, nipple area, and perianal region.
Atypical Symptoms
In addition to the classic presentation, patients may also experience:
- Generalized dry skin (xerosis)
- Dermatographism (skin writing reaction)
- Hand and foot dermatitis
Disease Progression
Acute Stage: Common in children under 2 years. Symptoms include intense itching, redness, swelling, and oozing.
Subacute Stage: Reduced inflammation and exudation, skin becomes drier.
Chronic Stage: Seen in older children (>10 years). Lesions become thickened, darkened, extremely itchy, and persistent, sometimes lasting into old age.
Possible Complications
If not treated properly, atopic dermatitis may lead to:
- Secondary bacterial infection
- Impetiginization
- In rare cases, acute glomerulonephritis due to untreated infection
When to See a Doctor
Causes of Atopic Dermatitis
The exact cause of atopic dermatitis (AD) remains unclear, but it is widely believed to result from a combination of genetic susceptibility, immune system dysregulation, and environmental triggers. Most people with AD have a family history of allergic conditions, particularly eczema, asthma, or allergic rhinitis—often referred to as the “atopic triad.”
Key contributing factors include:
- Genetic predisposition – Impaired skin barrier due to filaggrin gene mutation makes the skin more sensitive and prone to dryness and irritation.
- Immune system imbalance – Overactivation of the Th2 (T-helper 2) immune response causes chronic inflammation.
- Environmental irritants and allergens – Such as harsh soaps, detergents, dust mites, pet dander, or polluted air.
- Microbial imbalance on the skin – Overgrowth of Staphylococcus aureus can worsen flare-ups.

Who Is at Risk of Atopic Dermatitis?
Atopic dermatitis can occur at any age, but it most commonly begins in infancy or early childhood. Genetics play a major role—statistics show:
- If both parents have atopic dermatitis, the child has up to an 80% chance of developing the condition.
- If one parent is affected, the risk is around 40–50%.
- Individuals with atopic dermatitis are also more likely to develop other allergic diseases later in life, such as asthma or allergic rhinitis (a progression known as the “atopic march”).
Risk Factors for Atopic Dermatitis
Several internal (endogenous) and external (exogenous) factors increase the likelihood of developing or aggravating atopic dermatitis.
Internal Factors
- Psychological stress – Stress can trigger or worsen flare-ups by weakening the immune system.
- Hormonal changes – Fluctuations in hormones (e.g. pregnancy, menstrual cycle) may worsen symptoms.
- Metabolic disorders – Some people with nutrient deficiencies or impaired skin lipid production have a weaker skin barrier.
External Factors
- Allergens – Dust mites, pollen, animal fur, mold, certain foods (e.g. eggs, milk, nuts), bacteria, viruses, and fungi.
- Environmental conditions – Dry or cold climates, sudden temperature changes, exposure to chemicals or pollution.
- Irritants – Soaps, fragrances, harsh detergents, wool or synthetic fabrics, cigarette smoke.
Role of Immunoglobulin E (IgE)
Many patients with atopic dermatitis show elevated levels of IgE antibodies in their blood. IgE binds to mast cells in the skin. When allergens enter the body, they trigger these cells to release histamine and inflammatory mediators, resulting in itchiness, redness, and swelling.
Immune System Changes in Atopic Dermatitis
- Local immune changes – Chronic inflammation damages the skin barrier, making it easier for irritants and microbes to penetrate.
- Systemic immune response – Increased Th2 cytokines (IL-4, IL-13) contribute to persistent skin inflammation and itching.
Diagnosis and Treatment of Atopic Dermatitis
Diagnostic Methods
The diagnosis of atopic dermatitis (AD) is primarily clinical, based on a combination of symptoms, medical history, and typical lesion patterns. Laboratory tests are not always required but may support diagnosis in certain cases.
UK Working Party Diagnostic Criteria (1994)
A diagnosis of atopic dermatitis is made when itching (pruritus) is present along with at least three of the following five features:
- History of flexural eczema (or cheek involvement in children under 10 years old)
- Personal history of atopic disease (such as asthma or allergic rhinitis)
- History of generally dry skin
- Current flexural dermatitis (cheeks/forehead in children under 4)
- Onset before 2 years of age
This set of criteria is simple, widely used, and suitable for clinical practice even in community settings.
American Academy of Family Physicians Criteria (1999)
Major Criteria (must meet ≥ 3)
- Persistent itching
- Chronic or relapsing dermatitis
- Typical eczema distribution
- Infants/children: Vesicles on face and extensor surfaces
- Adults: Lichenified plaques in flexural areas
- Personal or family history of atopic conditions (eczema, asthma, urticaria, allergic rhinitis)
Minor Criteria (must meet ≥ 3)
- Xerosis (dry skin)
- Hyperlinearity of palms/soles
- Allergic conjunctivitis
- Pale facial appearance
- Pityriasis alba
- Ichthyosis
- Nonspecific hand/foot dermatitis
- Nipple eczema
- Positive type I hypersensitivity reactions
- Elevated serum IgE
- Food allergies
- Skin flushing or redness
- Early onset in childhood
- Dermatographism
- Follicular keratosis
These criteria are more detailed and are often used in research and academic settings rather than routine clinical diagnosis.
Treatment Strategies for Atopic Dermatitis
Treatment aims to control symptoms, repair the skin barrier, prevent flare-ups, and reduce inflammation.
1. Topical Therapy (First-line)
Acute Stage
- Wet dressings with Jarish solution (boric acid) or normal saline to reduce exudation and itching.
Subacute Stage
- Astringent pastes such as zinc oxide paste (e.g. Brocq’s paste) to reduce inflammation and scaling.
Chronic Stage
- Topical ointments and anti-inflammatory creams, including:
- Ichthammol ointment
- Coal tar preparations
- Salicylic acid
- Topical corticosteroids (e.g. eumovate, fucicort)
- Calcineurin inhibitors: tacrolimus 0.03–0.1%, pimecrolimus 1%
- Emollients are essential to maintain moisture and repair the skin barrier.
2. Systemic Therapy
These are used in moderate to severe cases:
- Antihistamines (to relieve itching, especially at night)
- Vitamin C (supports healing and immunity)
- Antibiotics if secondary bacterial infection is present (commonly due to Staphylococcus aureus)
3. Phototherapy and Advanced Options
UV therapy: UVA, UVB, or narrowband UVB may be used in chronic lichenified eczema.
LASER therapy (He-Ne) in selected cases.
Immunosuppressive agents for severe, refractory AD:
- Systemic corticosteroids (short-term only)
- Tacrolimus, cyclosporine, or azathioprine
- These require careful monitoring due to potential side effects.

4. Patient Education & Lifestyle Management
Long-term skin care is essential to prevent relapses:
- Use gentle, fragrance-free cleansers instead of harsh soaps
- Apply moisturizers daily
- Avoid known allergens and irritants
- Reduce stress, as it is a known trigger
- Maintain proper skin hygiene and avoid scratching
Lifestyle Measures & Prevention of Atopic Dermatitis
Healthy Habits to Control Atopic Dermatitis
Daily routines play a crucial role in reducing flare-ups and preventing the condition from worsening. Consistency in lifestyle and skin care is just as important as medical treatment.
Recommended Lifestyle Practices
- Follow your treatment plan as prescribed by a dermatologist. Avoid self-medicating, especially with corticosteroids or herbal products of unknown origin.
- Maintain a positive, stress-free lifestyle. Stress is a well-known trigger for flare-ups, so stress management techniques such as yoga, meditation, or adequate sleep can be helpful.
- Seek medical advice if symptoms worsen. Early intervention may prevent severe inflammation and secondary infections.
- Schedule regular check-ups to monitor disease progression and adjust treatment when necessary.
Nutrition and Diet
Currently, there is no specific diet proven to cure atopic dermatitis. However, some individuals may notice symptom improvement when avoiding trigger foods identified through allergy testing or observation. Maintaining a balanced diet rich in vitamins, omega-3 fatty acids, and antioxidants may support skin health.
Effective Prevention Strategies
The following steps can significantly reduce flare-ups and help protect the skin barrier:
Moisturize at least twice daily. Choose fragrance-free emollients or ointments designed for sensitive or atopic skin.
Avoid triggers such as:
- Excessive sweating
- Emotional stress
- Harsh soaps and detergents
- Fragrances
- Dust, pet dander, and pollen
Monitor food triggers in children. Eggs, cow’s milk, soy, and wheat may provoke flare-ups in infants and young children with atopic tendencies.
Limit bathing to 10–15 minutes using lukewarm water (not hot).
Use mild, hypoallergenic cleansers instead of traditional soap.
Pat skin dry with a soft towel (do not rub), then apply moisturizer immediately while the skin is still slightly damp to lock in hydration.
