Acne: Causes, Symptoms and Prevention Principles
Overview of Acne
What is acne?
Acne vulgaris is a skin condition characterized by the development of comedones, papules, pustules, nodules, and/or cysts due to blockage and inflammation of the pilosebaceous unit (hair follicle and sebaceous gland). Acne commonly appears on the face, chest, shoulders, and back.
Acne is caused by four main factors:
- Overproduction of sebum by sebaceous glands
- Blockage of hair follicles by sebum and dead skin cells
- Overgrowth of anaerobic bacteria Propionibacterium acnes (now known as Cutibacterium acnes)
- Excess production of inflammatory mediators
Acne vulgaris is classified into two main types:
Non-inflammatory acne
Includes blackheads (open comedones) and whiteheads (closed comedones). These develop due to sebum and dead skin blocking the hair follicles.
- Blackheads: Follicles are open at the surface.
- Whiteheads: Follicles are closed at the surface, making them harder to extract.
Whiteheads often progress into inflammatory acne.
Inflammatory acne
Includes papules, pustules, nodules, and cysts. These form when Propionibacterium acnes proliferates inside blocked pores, breaking down sebum into irritating free fatty acids, causing inflammatory reactions involving neutrophils and lymphocytes. When inflammation penetrates deeper into the dermis, it leads to nodule and cyst formation.
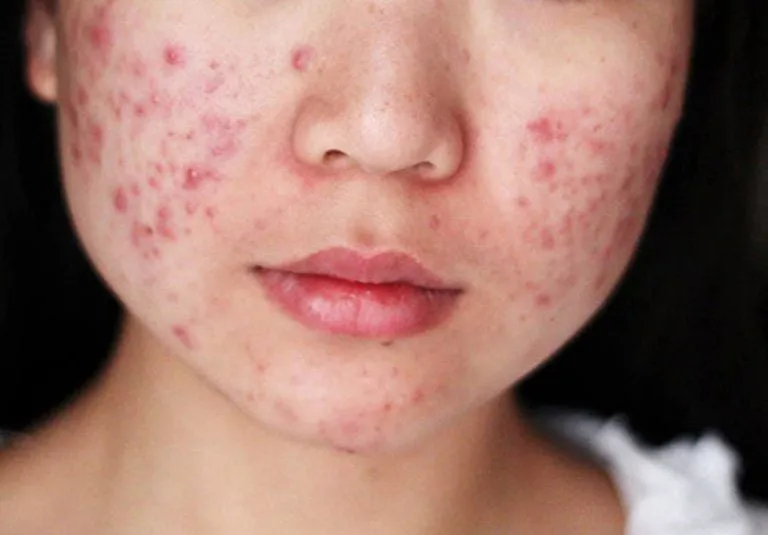
Symptoms of Acne
Signs and symptoms
- Whiteheads: Small, flesh-colored or white bumps (1–3 mm in diameter).
- Blackheads: Similar in size but with a dark center.
- Papules and pustules: Red, inflamed lesions (2–5 mm in diameter).
- Nodules: Large, painful solid lesions deep within the skin.
- Cysts: Soft, pus-filled lesions that may cause scarring if untreated.
Nodulocystic acne (severe acne) often leads to atrophic scars, hypertrophic scars, or keloids. Besides the face, the back, chest, shoulders, buttocks, arms, and scalp can also be affected.
Acne fulminans is a rare but severe form of acne characterized by sudden onset of painful ulcerative nodules, systemic symptoms such as fever, joint pain, and elevated white blood cell count.
Rosacea fulminans may resemble acne fulminans and is characterized by sudden onset of facial redness and pustules, usually in young women.
Impact of Acne on Health
Although acne is not a life-threatening disease, it can cause significant psychological stress, anxiety, and reduced self-esteem, affecting quality of life.
When to See a Doctor?
Causes of Acne
What causes acne?
During puberty, androgen hormones stimulate the activity of the sebaceous glands and cause excessive keratinization of hair follicles. In addition, several factors may trigger acne outbreaks, including hormonal changes, the use of unsuitable cosmetics, or inappropriate soaps.
Some studies suggest an association between dairy products and a high-glycemic diet with the development of acne.
Sunlight may have an anti-inflammatory effect, so acne tends to improve during the summer months.
Certain medications such as corticosteroids, phenytoin, lithium, and isoniazid may worsen acne.
Risk Factors for Acne
Who is at risk of developing acne?
Acne is more likely to affect:
- Adolescents going through puberty
- Women during menopause
- Individuals frequently exposed to dust and chemicals

Factors that Increase the Risk of Acne
Several factors may increase the likelihood of developing acne, including:
- Hormonal fluctuations during pregnancy or menstrual cycles
- High humidity
- Excessive sweating
- Use of inappropriate cosmetics or soaps
- Environmental pollution
Diagnosis and Treatment of Acne
Methods of Diagnosis
Acne is primarily diagnosed clinically through:
- Evaluation of acne-causing factors
- Determination of disease severity
- Assessment of psychological impact on the patient
Differential diagnosis should exclude conditions such as rosacea (no comedones), corticosteroid-induced acne (absence of comedones, numerous pustules), perioral dermatitis (typically affects areas around the eyes and mouth), and drug-induced acneiform eruptions.
Acne Severity Classification
| Severity Level | Definition |
| Mild | < 20 non-inflammatory lesions or < 15 inflammatory lesions or total lesion count < 30 |
| Moderate | 20–100 non-inflammatory lesions or 15–50 inflammatory lesions or total lesion count 30–125 |
| Severe | > 5 nodules or > 100 non-inflammatory lesions or > 50 inflammatory lesions or total lesion count > 125 |
Effective Treatment Options for Acne
Acne treatment includes topical or systemic therapies aimed at reducing sebum production, inflammation, and bacterial colonization.
Common Treatment Approaches
- Non-inflammatory acne (comedonal acne): Topical tretinoin
- Mild inflammatory acne: Topical retinoids alone or combined with topical antibiotics, benzoyl peroxide, or both
- Moderate inflammatory acne: Oral antibiotics combined with topical therapies as used in mild acne
- Severe inflammatory acne: Oral isotretinoin
- Nodular acne: Intralesional triamcinolone
Oral contraceptives are effective for both inflammatory and non-inflammatory acne in women. Spironolactone at 50 mg/day, increased gradually to 100–150 mg/day (maximum 200 mg/day), may also be beneficial for females with hormonal acne.
Light-based therapies are effective primarily in inflammatory acne.
Treatment by Severity
Mild Inflammatory Acne
Treatment should continue for at least 6 weeks or until response is achieved. First-line therapy is daily topical tretinoin. If tretinoin is not well tolerated, adapalene, tazarotene, azelaic acid, glycolic acid, or salicylic acid may be used as alternatives.
For mild papular or pustular acne, topical tretinoin may be combined with benzoyl peroxide, topical antibiotics, or both. If topical therapy is inadequate, comedone extraction by a dermatologist or nurse may be performed. If lesions are widespread, oral antibiotics may be considered.
Moderate Inflammatory Acne
Systemic antibiotics such as minocycline, tetracycline, erythromycin, or doxycycline may be used for 12 weeks or longer. Topical agents may be used concurrently as in mild acne.
Severe Inflammatory Acne
Oral isotretinoin is the treatment of choice. The standard dose is 1 mg/kg/day for 16–20 weeks, which may be increased up to 2 mg/kg/day if necessary. In patients who cannot tolerate side effects, the dose may be reduced to 0.5 mg/kg/day.
Nodular Acne
Treated with intralesional injection of 0.1 mL triamcinolone acetonide (2.5 mg/mL).
Other Forms of Acne
- Facial pustular dermatitis: Treated with oral corticosteroids and isotretinoin
- Acne fulminans: Requires oral corticosteroids and systemic antibiotics
- Cystic acne: Treated with systemic antibiotics; if unresponsive, oral isotretinoin is recommended
- Scarring: Managed with chemical peels, laser resurfacing, subcision, dermabrasion, collagen injections, or dermal fillers
Lifestyle and Prevention of Acne
Healthy Habits to Help Control Acne Progression
Lifestyle Recommendations
Wash your face twice daily and after excessive sweating
Shave carefully to avoid skin irritation
Shampoo regularly and keep hair away from the face
Avoid touching or picking at the skin
Use skincare and cosmetics with caution; choose non-comedogenic products
Apply sunscreen daily to protect the skin
Do not squeeze or pop acne lesions

Dietary Recommendations
Drink plenty of water
Limit oily and greasy foods
Ensure adequate intake of vitamins and antioxidants
Avoid overly spicy foods
Effective Measures to Prevent Acne
To lower your risk of acne breakouts, consider the following tips:
- Maintain proper facial hygiene
- Moisturize regularly with suitable products
- Minimize makeup use; always remove it thoroughly
- Protect your skin from sun exposure
- Exercise regularly to improve circulation and detoxification
- Reduce prolonged stress through relaxation techniques
