Toothache: Causes, Symptoms, Treatment Principles, and Prevention
Overview
What Is a Toothache?
A toothache is discomfort or sharp pain arising inside or around a tooth, usually triggered when the nerves within the dental pulp become inflamed or irritated. Pain patterns vary widely—some people experience intermittent twinges, while others suffer from nonstop, throbbing pain even without any obvious trigger.
Mild gum-related irritation may resolve with home care. However, persistent or severe toothache almost always indicates an underlying dental condition that requires prompt professional evaluation to prevent complications.

Symptoms
Common Signs and Symptoms of Toothache
A toothache may present with:
- Sharp, throbbing, or constant pain
- Discomfort that worsens with biting or chewing
- Sensitivity to hot, cold, or sweet foods
- Swelling around the affected tooth
- Fever or headache
- Foul-smelling discharge from an infected tooth
- Bad breath
Symptoms Suggesting Complications
If the infection spreads beyond the tooth, the following may occur:
- Dental abscess or sinus involvement: facial pain, facial swelling
- Submandibular space infection (Ludwig’s angina): painful swelling below the tongue, difficulty swallowing, elevation of the tongue
- Sinusitis secondary to dental infection: pain that worsens when bending forward
- Cavernous sinus thrombosis: severe headache around the eyes, fever, visual disturbances
Red Flags – Seek Emergency Care Immediately
- High fever
- Severe headache
- Rapidly spreading facial swelling
- Difficulty breathing or swallowing
- Changes in vision or neurological symptoms
- Swelling or firmness in the floor of the mouth
Health Impact of Untreated Toothache
A toothache isn’t just uncomfortable—it can significantly lower the quality of daily life:
- Persistent pain disrupts eating, sleeping, and concentration
- Long-term infection may damage surrounding bone and soft tissues
- Advanced abscesses can spread to the neck, sinuses, or even the bloodstream
- Rare but severe complications (e.g., Ludwig’s angina, cavernous sinus thrombosis) can be fatal if not promptly treated
Possible Complications
Although uncommon, untreated tooth infections may lead to:
Sinus Infection (Odontogenic Sinusitis)
Infections from upper back teeth can extend into the maxillary sinus, causing symptoms that mimic sinus disease and complicate diagnosis.
Ludwig’s Angina
A rapidly progressing, dangerous infection of the floor of the mouth.
Symptoms include swelling under the jaw, difficulty breathing, difficulty swallowing, and drooling. This condition is a medical emergency.
Cavernous Sinus Thrombosis
A rare clot formation in the cavernous sinus near the brain, typically beginning with a dental or facial infection.
Symptoms include high fever, vision changes, severe headache, and swelling around the eyes.
When to See a Doctor or Dentist
You should seek medical or dental care as soon as possible if:
- Toothache lasts longer than 24–48 hours
- Pain worsens despite using pain relievers
- You have swelling, pus, fever, or difficulty opening your mouth
- The pain interferes with eating or sleeping
- Any red-flag symptoms appear

Causes of Toothache
Common Causes of Tooth Pain
Toothache typically originates from irritation or injury to the dental pulp—the soft tissue inside the tooth containing blood vessels and nerves. Below are the most frequent underlying causes, grouped for easier understanding:
1. Infections and Inflammation
Periapical abscess – A pocket of pus forming at the root tip due to untreated cavities or trauma.
Pulpitis (reversible or irreversible) – Inflammation of the dental pulp causing sensitivity or severe throbbing pain.
Periodontal disease – Infection and inflammation of the gums and supporting tissues, sometimes spreading to the bone.
2. Structural Damage
Dental caries (cavities) – Damaged enamel exposes sensitive inner layers, causing pain with hot, cold, sweet foods, or brushing.
Cracked tooth or fractured crown – Pain appears when chewing or applying pressure.
Vertical root fracture – Often subtle but may lead to persistent discomfort and gum swelling.
3. Eruption-related Problems
Wisdom tooth (third molar) eruption – Impacted or partially erupted teeth can irritate surrounding tissue and cause pericoronitis.
Normal tooth eruption (frequent in children).
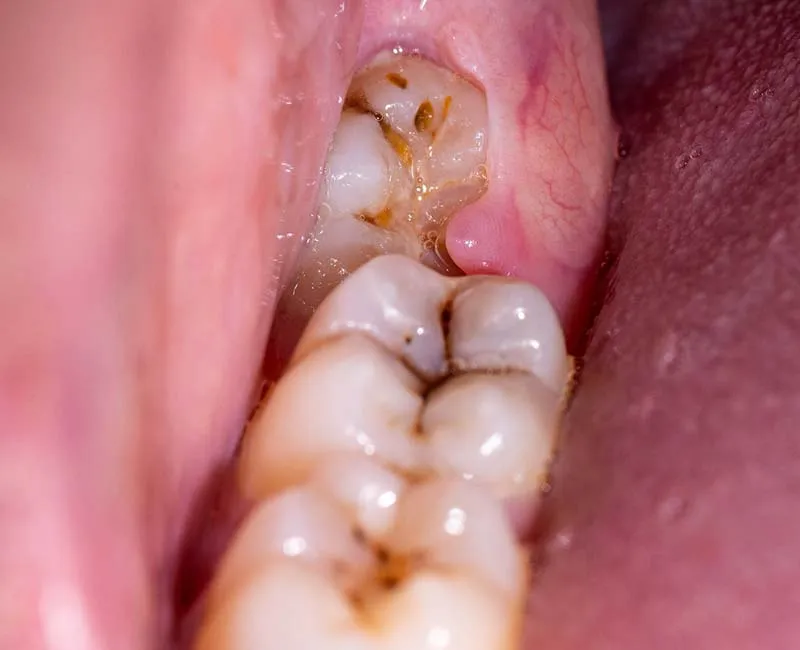
4. Trauma
Pulp injury from an accident – A blow to the face can damage nerve tissue without obvious external signs.
5. Other medical conditions
Sinusitis, especially maxillary sinus infection – Can mimic upper tooth pain due to shared nerve pathways.
Who Is at Risk of Developing Tooth Pain?
Toothache can occur at any age, but certain groups face a much higher risk.
Key Risk Factors
- Poor oral hygiene Not brushing twice daily, not using floss, or skipping dental check-ups increases the risk of cavities and gum disease.
- High-sugar diet Frequent consumption of sweets, desserts, and sugary beverages promotes bacterial overgrowth and enamel breakdown.
- Dry mouth (xerostomia) Common among older adults or individuals taking medications such as antihypertensives, sedatives, antihistamines, or antidepressants.
Saliva protects teeth—when it’s reduced, cavity risk spikes. - History of dental issues Previous cavities, gum disease, or dental procedures raise recurrence risk.
Diagnostic Approach: How Dentists Evaluate Tooth Pain
Accurate diagnosis is essential because toothache can involve multiple causes, sometimes unrelated to the teeth themselves.
1. Medical and Dental History (SOCRATES Method)
Dentists often use a structured interview to pinpoint the problem:
- S – Site: Where exactly does it hurt?
- O – Onset: When did the pain start?
- C – Character: Sharp? Throbbing? Dull?
- R – Radiation: Does the pain spread to the jaw, ear, or head?
- A – Associations: Any swelling, fever, bad breath, or gum bleeding?
- T – Time course: Is the pain constant or intermittent?
- E – Exacerbating/relieving factors: What triggers or improves pain?
- S – Severity: How intense is the pain on a scale of 1–10?
2. Clinical Examination
Identify whether the pain is spontaneous or triggered by temperature, sweets, or pressure.
Check for gum swelling, redness, or visible cavities.
Evaluate for localized swelling at the tooth base, which often indicates a periapical abscess.
Test teeth individually using:
- Percussion tests (tapping gently)
- Cold test (ice/cold spray)
- Healthy tooth: Pain stops immediately.
- Prolonged pain: Suggests irreversible pulpitis or pulp necrosis.
Palpate the floor of the mouth for firm swelling, which may signify a deep-space infection.
Perform a neurological exam (cranial nerves) if the patient has fever, facial swelling, or severe headache—important to rule out complications like sinus thrombosis.
3. Imaging Studies
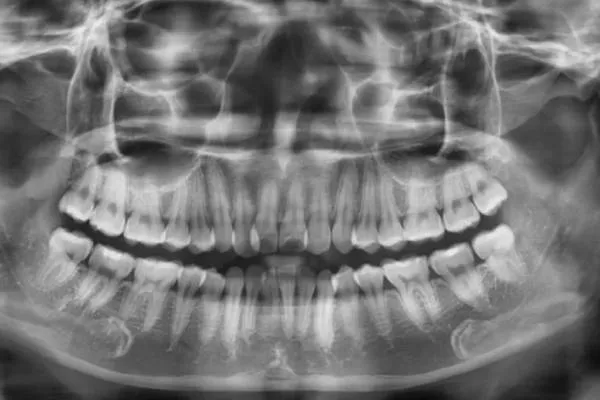
Dental X-rays (periapical or panoramic)
– First-line imaging for most tooth problems.
CT or MRI
– Recommended when severe infections are suspected, such as:
- Cavernous sinus thrombosis
- Ludwig’s angina (a rapidly spreading infection under the tongue and jaw—life-threatening)
Effective Treatments for Toothache
Tooth pain can be intensely uncomfortable, and managing the symptoms properly while you wait for definitive dental care is essential. Treatment varies depending on the underlying cause, but the goals are the same: relieve pain, control infection, and prevent complications.
1. Pain Relief Options
Over-the-Counter Analgesics
While awaiting a dental evaluation, patients can take pain relievers to manage symptoms. Nonsteroidal anti-inflammatory drugs (NSAIDs) are typically the first-line choice because they address both pain and inflammation—two major contributors to toothache.
- Ibuprofen is often preferred.
- Evidence consistently shows that combining ibuprofen with acetaminophen provides stronger analgesia than either medication alone.
However, opioids generally do not relieve dental pain as effectively as NSAIDs and pose risks such as sedation, constipation, and dependence. They should be prescribed minimally and for short duration only.
Topical Anesthetics
Short-term numbing agents may help when the gums or oral mucosa are ulcerated or irritated:
- Lidocaine gel 2%
- Benzocaine gel 7.5–10%
Local Anesthetic Nerve Blocks
For severe or persistent toothache, a clinician may perform a nerve block using bupivacaine with epinephrine, which can provide hours of relief. This is particularly beneficial in emergency care settings.
2. Antibiotic Therapy
Antibiotics are not routine for toothache and should be used only when there is evidence of systemic or progressive infection. Overuse can promote resistance and may even delay appropriate dental procedures.
Indications for Antibiotics
- Fever, malaise
- Enlarged or tender lymph nodes
- Spreading cellulitis, facial swelling
- Trismus (difficulty opening the mouth)
- Suspected Ludwig’s angina (rapidly progressive infection under the tongue)
- Immunocompromised patients
Commonly Used Antibiotics
- Penicillin V or amoxicillin
- Amoxicillin + metronidazole for anaerobic coverage
- Amoxicillin–clavulanate or clindamycin for broader-spectrum or penicillin-allergic patients
Emergency Warning:
If the patient has rapidly spreading swelling, difficulty breathing, drooling, or signs of sepsis, immediate transfer to an emergency department is critical.
Prophylactic Antibiotics
Current guidelines recommend prophylaxis only for high-risk patients undergoing invasive dental procedures, such as those with:
- Prosthetic heart valves
- Prior infective endocarditis
- Specific congenital heart diseases
- Cardiac transplant recipients with valvular disease
- High-risk rheumatic heart conditions
3. Mouth Rinses
Simple rinses can reduce inflammation and bacterial load while awaiting treatment:
- Chlorhexidine 0.12% rinse
- Warm hypertonic saline (1 tablespoon salt in a cup of warm water)
Hold the solution on the affected side until it cools, then expel. Repeat several times.
Use 3–4 times daily to manage mild swelling and gum irritation.
4. Dental or Surgical Treatment
Drainage of Dental Abscess
If a periapical abscess has softened, incision and drainage are required to remove pus and relieve pressure.
Management of Serious Infections
- Ludwig’s angina and
- Cavernous sinus thrombosis
are life-threatening conditions. Treatment often includes:
- Removal of the infected tooth
- IV antibiotics
- Possible airway management
Lifestyle Measures & Prevention
Healthy Habits to Reduce Tooth Pain Progression
- Follow your dentist’s instructions closely.
- Manage stress levels—stress can worsen jaw clenching and grinding.
- Seek medical care promptly if symptoms worsen.
- Schedule routine dental check-ups to detect early disease.
- Eat soft foods and apply a cold compress to the cheek for 15–20 minutes each hour to reduce mild pain and inflammation.
Nutrition Tips for Oral Health
A balanced diet plays a major role in preventing dental disease:
Recommended Foods
- Calcium- and phosphorus-rich foods:
dairy products, nuts, chicken, leafy greens. - High-water, crunchy fruits such as apples, pears, and watermelon to dilute sugars and stimulate saliva.
- Combine acidic foods with other dishes to reduce the acid load on teeth.
Effective Prevention Strategies
To minimize the risk of toothache and dental disease:
- Visit the dentist every 6 months for professional cleaning and evaluation.
- Limit sugary foods and beverages as much as possible.
- Avoid smoking—tobacco accelerates gum disease and tooth decay.
- Brush twice daily for at least 2 minutes with fluoride toothpaste.
- Clean interdental spaces with floss or interdental brushes daily.
