What Are ALT and AST? The Transaminases Explained
ALT (formerly SGPT) and AST (formerly SGOT) are enzymes belonging to the aminotransferase group. Their primary function is to catalyze the transfer of an amino group from an amino acid to an $\alpha$-keto acid, a vital process in intermediary metabolism.
- ALT (Alanine Aminotransferase): This enzyme is predominantly and most highly concentrated in the cytoplasm of hepatocytes (liver cells). Its high specificity for the liver makes it the more reliable indicator of acute hepatocellular injury.
- AST (Aspartate Aminotransferase): While abundant in the liver, AST is less specific as it’s found in significant quantities in other organs, including the heart (cardiac muscle), skeletal muscle, kidneys, brain, pancreas, lungs, leukocytes, and erythrocytes (red blood cells). Furthermore, AST exists in two forms within the cell: cytoplasmic and mitochondrial.
Clinical Value and Interpretation of ALT and AST Levels
The reference ranges for these enzymes can vary slightly between laboratories, but generally:
-
- Normal Range: AST <40 U/L, ALT <41 U/L (These are approximate values and should always be compared to the lab’s specific reference range).
Changes in these values can be categorized based on their magnitude, each pointing toward a different spectrum of liver pathology:
Marked Elevation (>1000 U/L** or even >3000 U/L)**
Pathology: This severe spike is indicative of massive hepatocellular necrosis (widespread liver cell death).
Common Causes:
- Acute Viral Hepatitis (e.g., Hepatitis A, B, C, D, E).
- Ischemic Hepatitis (Shock Liver): Resulting from prolonged circulatory collapse/hypotension (e.g., severe heart failure or shock).
- Severe Toxin or Drug-Induced Liver Injury (DILI): Particularly acetaminophen (paracetamol) overdose.
Moderate Elevation (<300 U/L or 2−10× Upper Limit of Normal (ULN))
Pathology: Seen in less severe or chronic inflammatory processes.
Common Causes:
- Alcoholic Hepatitis: Characterized by a predominant rise in AST (often AST > ALT), where the AST/ALT ratio is typically between 2:1 and 10:1.
- Non-Alcoholic Fatty Liver Disease (NAFLD/NASH).
- Chronic Hepatitis.
Insight into Alcoholic Liver Disease: The reason AST is often higher than ALT in alcohol-related injury is twofold:
- Alcohol damages the mitochondria (where much of the AST resides), releasing more AST; and
- Alcohol metabolism depletes the liver of pyridoxal 5-phosphate (Vitamin B6), a necessary cofactor for ALT synthesis, thus artificially lowering ALT levels.

Mild Elevation (<100 U/L or <2× ULN)
Pathology: May represent early, minimal, or chronic, slow-progressing liver disease, or even non-hepatic conditions.
Common Causes:
- Non-Alcoholic Fatty Liver (Hepatic Steatosis).
- Chronic Viral Hepatitis.
- Cirrhosis (advanced scarring).
- Focal or Metastatic Liver Disease (e.g., tumors).
- Biliary Obstruction (Cholestasis): In acute obstruction (e.g., passing a gallstone), ALT may spike transiently (usually <500 U/L) and then rapidly decline as the obstruction is relieved or becomes chronic.
The De Ritis Ratio (AST/ALT Ratio)
The ratio of AST to ALT, known as the De Ritis Ratio, provides crucial diagnostic context:
| AST/ALT Ratio (O/P Ratio) | Clinical Significance / Suggested Etiology |
| < 1 | Acute Hepatocellular Necrosis, most commonly Acute Viral Hepatitis. (ALT is higher). |
| > 1 | Chronic Liver Damage/Fibrosis/Cirrhosis. (AST is higher). |
| > 2 | Strongly suggestive of Alcoholic Liver Disease. (Due to low ALT/high AST as noted above). |
| > 4 | Suggests a rare condition like Fulminant Wilson’s Disease or certain muscle disorders. |
When Are ALT and AST Tests Indicated?
The decision to order ALT and AST tests is based on two main categories: symptoms and risk factors.
Clinical Symptoms of Liver Dysfunction:
The tests are a standard part of a Liver Function Panel (LFP) for patients presenting with:
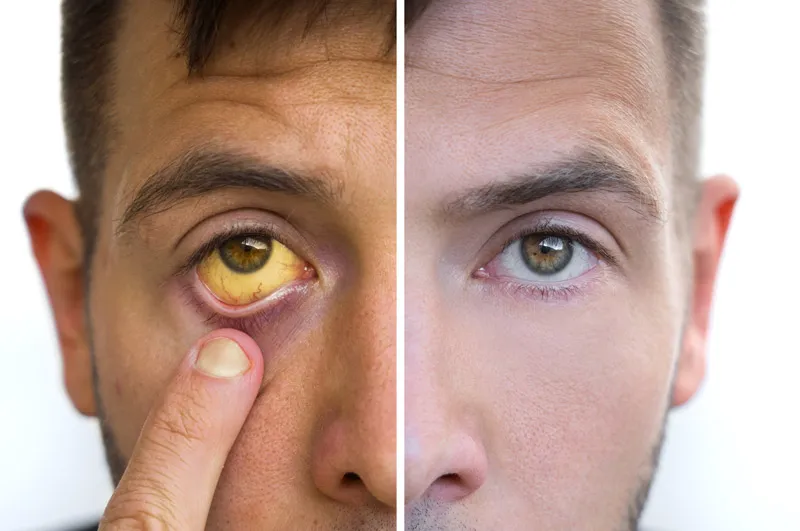
- Jaundice (yellowing of the skin/eyes).
- Nausea, vomiting, and loss of appetite (anorexia).
- Fatigue and malaise.
- Right upper quadrant (RUQ) abdominal pain or tenderness.
- Dark urine and pale-colored stools (suggestive of bile duct issues).
- Unexplained itching (pruritus).
Monitoring and Screening for Risk Factors:
These tests are also vital for screening and ongoing management of high-risk populations:
- Individuals with a history of exposure to Hepatitis viruses.
- Patients with severe or chronic alcohol use disorder.
- Individuals with metabolic risk factors: Obesity, Diabetes (Type 2), or other features of Metabolic Syndrome (often linked to NAFLD).
- People with a known family history of liver disease.
- Patients undergoing treatment with potentially hepatotoxic medications (medications known to cause liver damage).
Tracking Treatment Efficacy
Transaminase levels are essential for monitoring the effectiveness of treatment for chronic liver conditions (e.g., antiviral therapy for Hepatitis B or C). Regular testing helps determine if the therapeutic intervention is successfully reducing inflammation and minimizing liver damage.
Technical Aspects: Sample Collection and Preparation
The accuracy of the results depends heavily on proper pre-analytical procedures.
Sample Type: Serum (clot activator tube) or plasma (using anticoagulants such as Heparin or EDTA).
Fasting: Fasting is generally not required before drawing blood for ALT/AST. However, a lipemic (cloudy/fatty) or turbid serum sample can interfere with spectrophotometric analysis, potentially leading to inaccurate results.
Factors That Can Interfere with Test Results
| Effect on Transaminase Levels | Common Interfering Factors / Medications |
| Increased ALT/AST Activity | Pharmacological Agents: Acetaminophen (paracetamol), Angiotensin-Converting Enzyme (ACE) inhibitors, Anticonvulsants, certain Antibiotics, Statins (cholesterol-lowering drugs), Thiazide diuretics, and Psychiatric medications. |
| Hemolysis (Red Blood Cell Breakdown) | Because AST is present in red blood cells, a hemolyzed (broken down) blood sample will artificially increase the measured AST level, making the result unreliable. |
| Decreased AST Activity | Pharmacological Agents: Metronidazole, Trifluoperazine, and certain others. |
