Red Eye: Causes, Symptoms, and Effective Treatments
Understanding Red Eye
What Is Red Eye?
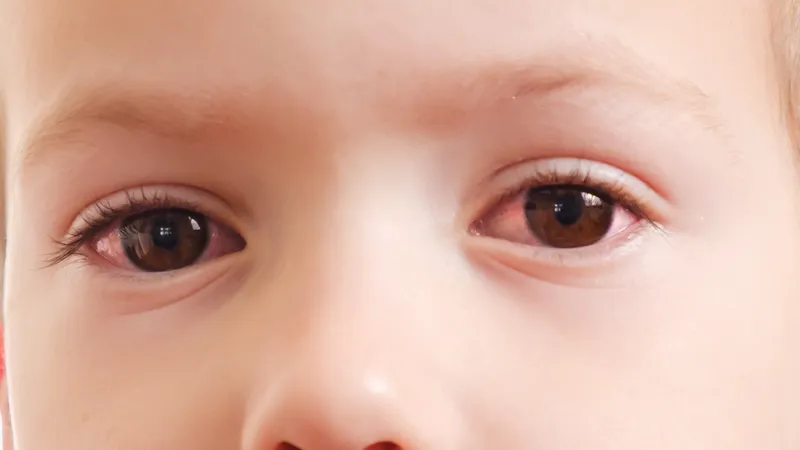
Red eye refers to the visible dilation of blood vessels on the surface of the eyeball. This condition may result from infections, allergies, inflammation, or increased intraocular pressure.
The redness typically involves the conjunctiva — the thin, transparent membrane covering the white part of your eye — but can also affect deeper structures such as the iris (uvea), episclera, or sclera.
Common Signs and Symptoms
Red eye can manifest in several ways depending on the underlying cause:
- Noticeable redness in one or both eyes
- Discharge or crusting around the eyelids (often yellow or green in bacterial infections)
- Excessive tearing or watery eyes
- Eye discomfort or pain
- Sensitivity to light (photophobia)
- A gritty or “sand-like” sensation in the eyes
- Swollen or puffy eyelids
In some cases — especially when caused by viruses such as adenovirus — patients may also experience:
- Fever or sore throat
- Fatigue
- Swollen lymph nodes near the ears
- Mild headache or body aches
How Red Eye Affects Your Health
Red eye is a common clinical presentation, and in most cases, it is benign and self-limiting. However, a small number of patients may have sight-threatening conditions that require urgent ophthalmologic evaluation — such as corneal ulcers, acute glaucoma, or uveitis.
Possible Complications
If left untreated or mismanaged, red eye can lead to:
- Reduced vision or blurred eyesight
- Corneal inflammation (keratitis)
- Corneal scarring
- Permanent vision loss or blindness
When to See a Doctor
Seek immediate medical attention if you experience any of the following:
- Sudden change or loss of vision
- Severe headache, intense eye pain, or fever
- Unusual sensitivity to light
- Nausea or vomiting accompanying eye pain
- Redness following chemical exposure or a foreign object in the eye
- Seeing halos around lights
- Noticeable swelling around or inside the eye
- Inability to open the affected eye
Causes of Red Eye
Red eye can result from bacterial, viral, or allergic reactions, as well as environmental factors or physical irritation.
1. Bacterial Causes
Bacterial conjunctivitis often leads to purulent (pus-like) discharge and crusting.
Common bacteria include:
- Staphylococcus aureus — frequently associated with eyelid inflammation (blepharitis)
- Haemophilus influenzae — common in children and may occur with ear infections
- Streptococcus pneumoniae and Moraxella catarrhalis
- Neisseria gonorrhoeae — a severe form linked to sexually transmitted infections; this can rapidly cause corneal ulceration and perforation
2. Viral Causes
Viruses account for over 80% of red eye cases.
The most common culprit is adenovirus, which causes epidemic keratoconjunctivitis (EKC).
Less frequent causes include:
- Enterovirus
- Coxsackievirus
- Herpes simplex virus (HSV) — may cause corneal infection and recurrent flare-ups
3. Allergic Causes
Allergic conjunctivitis is triggered by exposure to allergens such as dust, pollen, animal dander, certain medications, or chemical agents.
Symptoms often include itchy, watery, and swollen eyes, sometimes recurring seasonally or persisting year-round.
Who Is at Risk?
You may be more prone to red eye if you have:
- Chronic dry eyes
- Eye allergies
- Contact lens use (especially poor hygiene or overuse)
- Recurrent viral or bacterial conjunctivitis
Other Risk Factors Include:
- Airborne allergens (dust, mold, pet dander)
- Air pollution or smoke exposure
- Dry air (air-conditioned offices, airplane cabins)
- Chemical exposure (e.g., chlorine in swimming pools)
- Excessive sunlight or UV exposure without sunglasses
- Contact with contaminated water or unhygienic environments

Diagnosis and Treatment of Red Eye
How Red Eye Is Diagnosed
Because red eye has many possible causes, a thorough examination is necessary to identify the source of inflammation.
An eye doctor (ophthalmologist or optometrist) typically performs several evaluations, including:
1. Medical and General Examination
- Checking the head, neck, nose, and throat for signs of allergies or respiratory infections.
- Reviewing recent exposure to irritants, contact lenses, or infected individuals.
2. Eye Examination
- Visual acuity test to assess how well you see.
- Pupil size and light reflex evaluation.
- Fluorescein dye test to highlight corneal abrasions or ulcers.
- Slit-lamp examination for detailed inspection of the eye’s surface and anterior chamber.
- Eyelid eversion (flipping the eyelid) to check for hidden foreign objects.
- Tonometry (eye pressure test) when glaucoma is suspected.
In most mild cases of conjunctivitis, no laboratory tests are required.
However, cultures or viral testing may be performed when:
- Herpes infection is suspected
- The condition is severe or persistent
- There is corneal ulceration or scarring
- Autoimmune disease is suspected

Effective Treatment Options for Red Eye
Treatment depends on the underlying cause and severity of the condition.
The goal is to relieve symptoms, control infection, and prevent complications.
1. Viral Conjunctivitis
- Usually self-limiting and resolves within 1–2 weeks.
- Apply cold compresses several times a day to reduce swelling and irritation.
- Rinse eyes gently with saline solution (0.9% sodium chloride).
- Use artificial tears for lubrication and comfort.
- Antihistamine eye drops may be recommended if itching is significant.
- In cases caused by herpes simplex virus, antiviral medication such as acyclovir 400 mg (five times daily) is prescribed.
Important Warning: Avoid using steroid eye drops in viral conjunctivitis unless directed by an ophthalmologist. Steroids can worsen viral infections and delay healing.
Hygiene Reminder: Viral conjunctivitis is highly contagious. Wash your hands frequently, avoid touching your eyes, and do not share towels, makeup, or bedding.
2. Bacterial Conjunctivitis
- Requires antibiotic eye drops or ointments for 5–7 days.
- Keep the eye area clean with sterile saline.
- For infections caused by Haemophilus influenzae, oral amoxicillin/clavulanate may be prescribed.
- For gonococcal infections, immediate medical care is required:
- Ceftriaxone 1 g intramuscularly
- Azithromycin 1 g orally
- Frequent saline irrigation and antibiotic ointment (fluoroquinolone)
- Hospitalization if corneal involvement is suspected.
3. Allergic Conjunctivitis
- Identify and avoid known allergens (dust, pollen, pet dander, chemicals).
- Use artificial tears to flush out irritants.
- Mild cases: Lubricating eye drops or cold compresses.
- Moderate cases: Antihistamine or mast-cell stabilizer drops.
- Severe cases: Short-term topical corticosteroids under doctor supervision.
- For widespread allergy symptoms, oral antihistamines may be added.
General Self-Care and Lifestyle Measures
Building good eye hygiene and overall health habits can significantly speed up recovery and prevent recurrence.
Hygiene Habits
- Wash your hands regularly with soap and water.
- Use your own towel, pillow, and wash basin.
- Wash face towels daily with hot water and dry under sunlight.
- Avoid touching or rubbing your eyes.
- Do not wear contact lenses until symptoms fully resolve.
Diet and Nutrition for Eye Health
A balanced diet rich in vitamins and antioxidants supports faster healing and stronger immunity.
- Vitamin A, C, and E: Found in carrots, sweet potatoes, spinach, kale, and pumpkins.
- Beta-carotene: In orange and red fruits (tomatoes, cherries, watermelon, beets).
- Zinc and Omega-3 fatty acids: Found in fish, eggs, nuts, and seeds — protect against dryness and inflammation.
- Adequate protein intake (chicken, eggs, fish, milk) helps the body produce antibodies and repair tissues.
- Stay well-hydrated throughout the day to reduce dryness and flush out toxins.

Preventing Red Eye
Simple preventive measures can protect you and your family from recurring eye irritation or infections.
Tips for Prevention
- Wash your hands often or use alcohol-based sanitizers.
- Rinse your eyes daily with sterile saline solution (0.9%) three times a day.
- Do not share eye drops, makeup, or personal items with others.
- Avoid close contact with anyone who has red eye.
- Stay away from crowded or poorly ventilated areas during outbreaks.
- Avoid swimming in chlorinated or contaminated water.
- Always wear UV-protective sunglasses when outdoors.
- Maintain clean, allergen-free indoor air by using air filters and humidifiers.
Key Takeaways
- Most cases of red eye are mild and self-limiting, but a few can lead to serious vision damage if ignored.
- Identify and treat the root cause — whether viral, bacterial, or allergic — instead of self-medicating.
- Maintain excellent eye hygiene and nutrient-rich diet to protect ocular health long-term.
- Always consult an eye specialist if symptoms persist beyond a few days or worsen over time.
Important Medical Warning: Persistent redness, pain, or discharge should never be ignored.
Misusing eye drops — especially steroids or unprescribed antibiotics — can cause irreversible vision loss.
Early evaluation by an ophthalmologist ensures safe, effective, and lasting recovery.
