Lipodystrophy: Understanding the Disorder and How It’s Treated
What Is Lipodystrophy?
Fat tissue is found throughout the body — beneath the skin and surrounding internal organs. It serves several essential functions, including:
- Storing energy in the form of calories
- Cushioning and protecting vital organs
- Regulating body temperature
- Releasing hormones such as leptin, which help control appetite and metabolism
Lipodystrophy disrupts the body’s ability to produce, store, and use fat properly. Instead of being evenly distributed, fat may concentrate in specific regions (such as the abdomen, face, neck, or upper torso) while being nearly absent in others (like the arms, legs, or buttocks).
Main Types of Lipodystrophy
Lipodystrophy can be congenital (genetic) or acquired (developed later in life). Each type affects fat distribution differently and may have distinct causes.
1. Congenital Generalized Lipodystrophy (CGL)
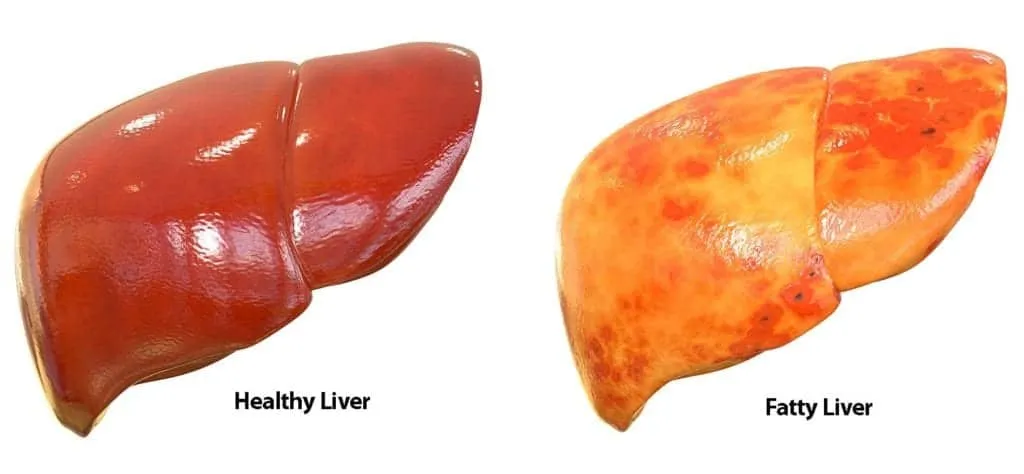
This extremely rare inherited disorder is present from birth. Affected infants often begin losing subcutaneous fat within the first few weeks of life and appear unusually muscular due to the absence of body fat. Because fat cannot be stored properly, fat accumulates in the liver and other organs, leading to metabolic problems such as insulin resistance and fatty liver disease.
2. Familial Partial Lipodystrophy (FPL)
Also genetic in origin, this condition typically appears during puberty. Individuals gradually lose fat from the arms and legs, while fat accumulates in the face, neck, and abdomen. Women are affected more frequently than men. FPL is often linked to metabolic syndrome, type 2 diabetes, and high triglyceride levels.
3. Acquired Generalized Lipodystrophy (AGL)
Also known as Lawrence syndrome, this form usually develops in adolescence. Its symptoms resemble congenital lipodystrophy, but it is not inherited. Researchers believe autoimmune mechanisms may play a role. AGL can also be associated with other immune disorders.
4. Acquired Partial Lipodystrophy (APL)
Sometimes called Barraquer–Simons syndrome, this type typically appears after childhood and causes a gradual loss of fat from the face, neck, and upper body, while sparing or even increasing fat in the lower body. In some patients, APL is linked to autoimmune conditions or viral infections.
5. Drug-Induced Lipodystrophy
This is one of the most common modern forms of lipodystrophy, often seen in people taking antiretroviral therapy for HIV. Fat loss in the arms, legs, and face may occur alongside fat buildup in the abdomen or upper back. Unfortunately, stopping the medication rarely reverses the changes completely.
6. Insulin-Related Lipodystrophy
Seen in some patients with diabetes, this form develops at insulin injection sites, leading to localized fat loss (lipoatrophy) or thickened fatty tissue (lipohypertrophy). Rotating injection sites is an important preventive measure.

Symptoms of Lipodystrophy
How to Recognize the Signs
The hallmark sign of lipodystrophy is a noticeable loss of subcutaneous fat — either throughout the entire body or in specific areas. In many cases, this fat loss is accompanied by abnormal fat accumulation in other regions. The appearance of symptoms varies depending on the type of lipodystrophy.
Congenital Generalized Lipodystrophy (CGL)
People with this form of lipodystrophy experience widespread fat loss and often appear unusually muscular, as fat is replaced by hypertrophied muscles. Over time, excess fat accumulates inside muscles and organs such as the liver and heart.
Typical symptoms and complications include:
- Elevated insulin and triglyceride levels
- Severe insulin resistance
- Fatty liver disease (hepatic steatosis)
- Early-onset diabetes
- Increased risk of heart disease and liver failure
Life expectancy may be shortened due to these metabolic complications if not properly managed.

Familial Partial Lipodystrophy (FPL)
In this inherited condition, fat loss primarily affects the limbs — especially the lower arms and legs — and typically becomes noticeable around puberty. In contrast, fat tends to build up in the face, neck, and abdomen, leading to a characteristic appearance.
People with FPL may experience:
- Pancreatitis caused by severe hypertriglyceridemia
- Type 2 diabetes due to insulin resistance
- Fatty liver and elevated blood lipids
Women are generally more affected than men, and symptoms often become more pronounced with age.
Acquired Generalized Lipodystrophy (AGL)
Also known as Lawrence syndrome, this rare condition develops during childhood or adolescence. It starts with gradual fat loss from the upper body, eventually spreading throughout the body. Unlike congenital forms, AGL is not inherited and may be associated with autoimmune disorders.
A distinguishing feature is fat accumulation in the hips and legs, sometimes giving the lower body a more prominent shape. Patients with AGL are also at higher risk of kidney disease compared to other forms of lipodystrophy.
Drug- or Treatment-Induced Lipodystrophy
Lipodystrophy related to highly active antiretroviral therapy (HAART) for HIV typically causes fat loss in the arms, legs, and face, along with fat gain in the abdomen, upper back (buffalo hump), and breasts.
Even when the medication is adjusted, these physical changes are often only partially reversible.
How Lipodystrophy Affects Overall Health
Fat tissue is made up of specialized fat cells (adipocytes) that play key roles in energy storage and hormone regulation. When fat cannot be stored properly, it tends to accumulate in organs such as the liver, pancreas, muscles, and bones. This “ectopic fat” buildup contributes to a range of metabolic complications, including:
- Fatty liver disease (hepatic steatosis)
- Insulin resistance and hyperinsulinemia
- Type 2 diabetes mellitus
- Severe hypertriglyceridemia
- Pancreatitis
- Metabolic syndrome
- Coronary artery disease (CAD)
Not everyone with lipodystrophy develops all of these complications. The severity and pattern of symptoms vary significantly from person to person.
When to See a Doctor
You should seek medical attention if you:
- Notice unexplained fat loss or fat accumulation in certain areas
- Experience symptoms of insulin resistance, such as fatigue or darkened skin patches
- Have a family history of metabolic disorders
- Are undergoing antiretroviral or insulin therapy and notice body fat changes
Early diagnosis is essential for effective management. A healthcare provider can perform blood tests, imaging studies, and genetic evaluations to determine the cause and guide appropriate treatment.
Causes of Lipodystrophy
Why Does Lipodystrophy Occur?
The causes of lipodystrophy vary depending on the type. Some forms are inherited through genetic mutations, while others develop later in life due to autoimmune disorders, infections, or medication side effects. Understanding the underlying cause is essential for accurate diagnosis and effective management.
1. Congenital Generalized Lipodystrophy (CGL)
Also known as Berardinelli–Seip syndrome, this condition follows an autosomal recessive inheritance pattern. It results from mutations in genes that regulate fat metabolism and adipocyte development — including AGPAT2, BSCL2 (seipin), CAV1 (caveolin-1), and PTRF (cavin-1).
These genetic defects disrupt the body’s ability to form and maintain fat tissue, leading to near-total loss of subcutaneous fat and the severe metabolic disturbances seen in affected individuals.
2. Familial Partial Lipodystrophy (FPL)
FPL is usually inherited in an autosomal dominant manner. The condition is caused by mutations in genes such as LMNA, PPARG, or AKT2, which are crucial for fat distribution and insulin sensitivity.
Patients typically lose fat in the limbs — especially the lower extremities — while gaining fat around the face, neck, and abdomen. Metabolic complications such as insulin resistance and dyslipidemia are common.
3. Acquired Generalized Lipodystrophy (AGL)
This extremely rare form of lipodystrophy develops after birth and involves progressive loss of body fat. The exact cause remains unclear, but research suggests a strong link to autoimmune diseases, where the body’s immune system mistakenly attacks its own fat cells.
Conditions associated with AGL include:
- Systemic lupus erythematosus (SLE)
- Autoimmune hepatitis
- Autoimmune thyroiditis
- Celiac disease
- Vasculitis
- Pernicious anemia
AGL often appears in women and may coexist with other connective tissue or inflammatory diseases.
4. Acquired Partial Lipodystrophy (APL)
Also known as Barraquer–Simons syndrome, the cause of APL remains uncertain. However, some studies suggest an immune-mediated mechanism involving complement-induced adipocyte lysis. In many patients, the presence of C3 nephritic factor (C3NeF) — an antibody linked to kidney disease — has been observed.
This abnormal immune response gradually destroys fat cells in specific regions, typically starting in the face and upper body and sparing the lower limbs.
5. Insulin-Related Lipodystrophy
This form develops in people receiving insulin injections for diabetes. The repeated use of the same injection site can cause either:
- Lipoatrophy – localized fat loss, appearing as a sunken scar-like area
- Lipohypertrophy – thickened, rubbery fat deposits under the skin
Both complications can interfere with insulin absorption and lead to unpredictable blood glucose fluctuations and episodes of hypoglycemia. Rotating injection sites is the best preventive strategy.
Risk Factors for Lipodystrophy
Who Is Most at Risk?
Certain genetic and environmental factors increase the likelihood of developing lipodystrophy.
- Family history: Having a first-degree relative (parent, sibling, or child) with lipodystrophy significantly raises the risk, particularly for congenital generalized and familial partial types.
- Autoimmune diseases: Individuals with autoimmune conditions such as lupus, autoimmune hepatitis, or thyroiditis are more likely to develop acquired forms.
- Infections: Viral or bacterial infections such as chickenpox, measles, infectious mononucleosis, diphtheria, osteomyelitis, pneumonia, and HIV have been linked to the onset of lipodystrophy.
- Medications: Long-term use of certain antiretroviral drugs or insulin therapy can trigger treatment-induced lipodystrophy.
- Gender and ethnicity: Acquired generalized lipodystrophy tends to occur more often in women, while acquired partial lipodystrophy is reported more frequently in people of Indian or South Asian descent, again with a higher prevalence among women.
Key Takeaway
Lipodystrophy can result from genetic mutations, immune dysfunction, or external factors such as infections and medications. Identifying the root cause not only helps guide treatment but also determines the long-term outlook for the patient.
Diagnosis and Treatment of Lipodystrophy
How Lipodystrophy Is Diagnosed
Diagnosing lipodystrophy typically begins with a detailed medical history review, physical examination, and careful evaluation of symptoms. Because the condition can resemble other disorders that cause abnormal fat distribution, such as Cushing’s syndrome or anorexia nervosa, these must first be ruled out.
If lipodystrophy is suspected, your doctor may perform several metabolic assessments to better understand your body’s fat distribution and hormone balance, including:
- Blood glucose testing: To check for insulin resistance or diabetes
- Liver function tests: To detect fatty liver or inflammation
- Lipid profile: To measure cholesterol and triglyceride levels
- Hormone tests: To assess leptin, insulin, and reproductive hormone levels
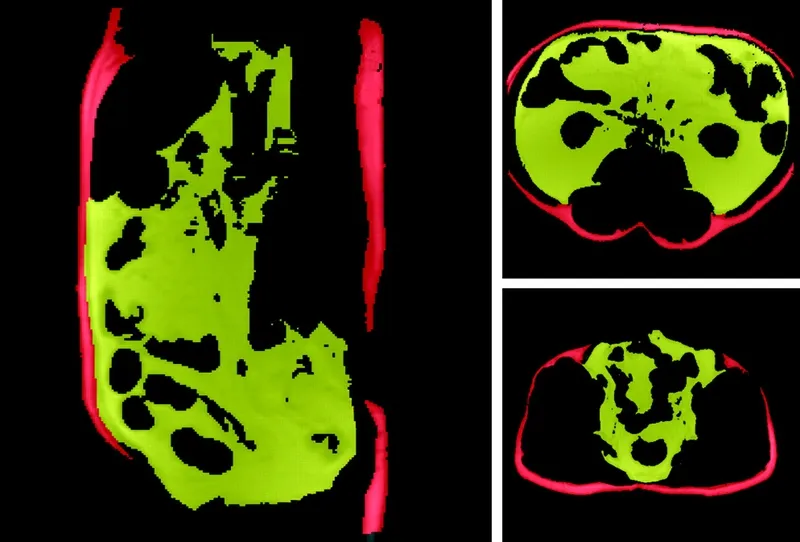
- MRI or body composition imaging: To visualize fat loss or accumulation patterns
- Genetic testing (if indicated): Although not always necessary, it may help confirm inherited forms of lipodystrophy
Because lipodystrophy affects multiple body systems, diagnosis often involves a multidisciplinary team — including an endocrinologist, cardiologist, nutritionist, and sometimes a genetic specialist.
Treatment Options for Lipodystrophy
Managing Symptoms and Improving Quality of Life
There is currently no cure for lipodystrophy. Treatment focuses on managing complications, stabilizing metabolism, and improving quality of life. Therapy is usually tailored to each patient’s specific type of lipodystrophy and associated health issues.
A comprehensive approach may include:
1. Management of Metabolic Disorders
- Diabetes control: Oral medications such as pioglitazone may improve insulin sensitivity and are often preferred over metformin in lipodystrophy-related diabetes. Severe cases may require insulin therapy.
- Lipid regulation: Statins (e.g., rosuvastatin, atorvastatin) are typically first-line agents for managing cholesterol abnormalities.
Patients with severe hypertriglyceridemia may benefit from fibrate derivatives or omega-3 fatty acid supplements (fish oil). - Polycystic Ovary Syndrome (PCOS): Hormonal regulation may be necessary in women with lipodystrophy-related reproductive disturbances.
2. Leptin Replacement Therapy (Metreleptin)
Metreleptin is a recombinant form of the hormone leptin that was approved by the U.S. FDA in 2014 for the treatment of generalized lipodystrophy. It helps compensate for leptin deficiency, restoring certain metabolic functions.
Clinical benefits include:
- Improved appetite regulation and satiety
- Reduction in hepatic fat accumulation
- Improved metabolic control and insulin sensitivity
- Normalization of pubertal development in adolescent females
Potential adverse effects:
While metreleptin is effective, it can cause serious side effects in some individuals, such as:
- Headache
- Hypoglycemia
- Abdominal pain
- Unintentional weight loss
- Development of anti-metreleptin antibodies, which may reduce effectiveness and increase infection risk
- Rare association with lymphoma (requires monitoring)
Due to these risks, metreleptin should only be used under close medical supervision, ideally by a specialist experienced in metabolic disorders.
3. Surgical and Cosmetic Procedures
For individuals who experience visible or disfiguring fat changes — particularly in sensitive areas such as the face, neck, chest, or pubic region — cosmetic surgery may be an option to restore self-confidence and body symmetry.
Common procedures include:
- Liposuction – to remove excess fat from areas like the chin, neck, or abdomen
- Fat grafting or reconstructive surgery – to restore volume in areas affected by fat loss
These procedures do not treat the underlying metabolic disorder but can significantly improve psychological well-being and social comfort.
4. Lifestyle and Supportive Care
Lifestyle management plays a vital role in improving overall health outcomes:
- Diet: A balanced, low-fat, nutrient-rich diet helps control blood glucose and lipid levels.
- Exercise: Regular physical activity enhances insulin sensitivity and cardiovascular health.
- Mental health support: Counseling and support groups can help patients cope with body image challenges and chronic disease stress.
Outlook
Although lipodystrophy is a lifelong condition, early diagnosis, proper treatment, and ongoing monitoring can help patients live longer and healthier lives. Advances in genetic research and hormone therapy continue to improve outcomes for those affected.
Lifestyle and Prevention of Lipodystrophy
Healthy Lifestyle Habits to Help Slow Disease Progression
Lifestyle recommendations:
- Engage in regular physical activity to reduce insulin resistance.
- Avoid smoking.
- Refrain from drinking alcohol.
- Get sufficient sleep and avoid staying up late.
- Stay well-hydrated and limit the consumption of alcoholic beverages.
Dietary recommendations:
- Maintain a nutritionally balanced diet.
- Prioritize healthy foods such as vegetables, fruits, and nuts.
- Reduce the intake of animal fats.

Effective Prevention Strategies for Lipodystrophy
Inherited (congenital) lipodystrophy cannot be prevented, as it results from genetic mutations. To assess your child’s potential risk, discuss your pregnancy plans with an obstetrician or genetic counselor.
For acquired lipodystrophy, which often develops due to infections or autoimmune disorders, vaccination against diseases such as chickenpox and measles may help lower the risk. However, autoimmune-related lipodystrophy cannot be prevented.
