Goiter: Symptoms, Causes, and Treatment
Overview of Goiter
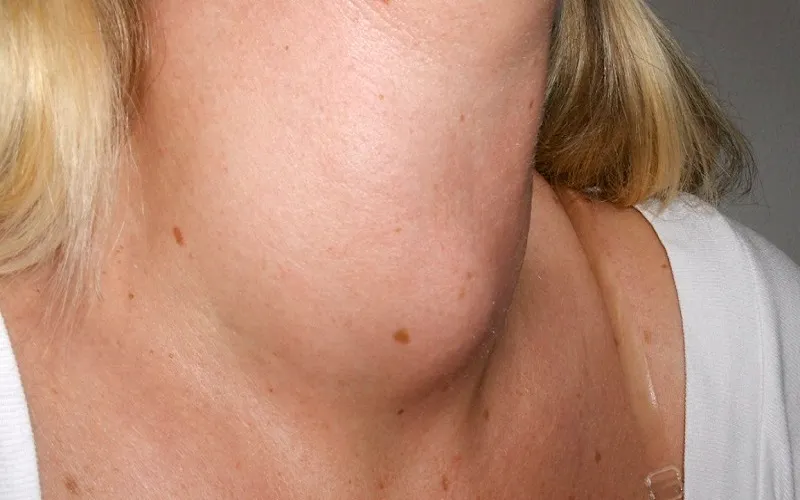
Goiter refers to an increase in the size of the thyroid gland, resulting in a noticeable swelling at the front of the neck. Depending on the cause, the swelling may or may not be painful.
There are several types of goiter:
Simple (non-toxic) goiter: Occurs when the thyroid gland does not produce enough thyroid hormones and enlarges to compensate. This type is often seen in pregnant or menopausal women, during puberty, or in individuals with iodine deficiency.
Congenital goiter: Present from birth due to developmental or genetic abnormalities of the thyroid.
Multinodular goiter: Characterized by the presence of multiple nodules (lumps) within the thyroid tissue.
Endemic (iodine-deficiency) goiter: Caused by insufficient iodine intake from the diet. In countries where iodized salt is commonly used, this form is now rare.
Sporadic (non-toxic) goiter: Often occurs without a clear cause, but may be associated with the use of certain medications.
Graves’ disease (toxic diffuse goiter): An autoimmune disorder in which the immune system produces antibodies that mimic thyroid-stimulating hormone (TSH), causing the gland to overproduce thyroid hormones and leading to hyperthyroidism.
Thyroid cancer (malignant goiter): Involves the development of malignant tumors within the thyroid gland.
A goiter is considered toxic when it is associated with hyperthyroidism, meaning the thyroid gland produces an excessive amount of hormones.
Symptoms of Goiter
Common Signs and Symptoms
You may have a goiter if you experience any of the following:
Noticeable swelling or enlargement in the neck, with one or more small nodules that gradually grow on one or both sides.
Difficulty breathing or swallowing due to compression of nearby structures.
Dry cough without other respiratory causes.
Hoarseness or changes in voice.
Dizziness when raising your arms above your head.
Tightness or discomfort in the throat.
Bulging eyes (exophthalmos) — often seen in patients with Graves’ disease.
Health Impacts of Goiter
As the thyroid gland enlarges, it can compress the trachea, esophagus, or nearby nerves, leading to:
- Difficulty swallowing or breathing.
- Persistent cough and throat pain.
- Hoarseness or voice changes.
In addition, a large goiter can cause neck discomfort, heaviness, and visible deformity, which may significantly affect the patient’s emotional well-being and self-confidence.
Possible Complications
In hyperthyroid goiter (toxic goiter): Without timely treatment, excessive thyroid hormone levels can cause serious cardiovascular issues such as arrhythmias, congestive heart failure, and thyroid storm, which can be life-threatening.
In hypothyroid goiter: If left untreated, reduced thyroid hormone levels can lead to metabolic, digestive, and cardiovascular complications, including fatigue, weight gain, and bradycardia.
When to See a Doctor
Early diagnosis and appropriate treatment can prevent disease progression and help you recover more quickly while avoiding serious complications.
Causes of Goiter
Goiter can result from various thyroid function abnormalities or structural changes within the gland. The causes are generally divided into hyperthyroid and hypothyroid conditions, along with other local or systemic factors.
Causes Related to Hyperthyroidism (Overactive Thyroid)
Thyroiditis: Inflammation of the thyroid gland, which may occur after viral infections or be congenital.
Graves’ disease (Basedow’s disease): An autoimmune disorder in which the immune system stimulates the thyroid to produce excess hormones.
Medications: Certain drugs such as amiodarone or interferon-α can trigger thyroid overactivity.
Iodine deficiency: When the body lacks iodine, the thyroid compensates by enlarging to trap more iodine, leading to goiter formation.
Causes Related to Hypothyroidism (Underactive Thyroid)
Hashimoto’s thyroiditis: A chronic autoimmune inflammation that damages thyroid tissue, reducing hormone production and leading to hypothyroidism.
Post-treatment or post-surgical hypothyroidism: After radioactive iodine therapy or thyroid surgery for hyperthyroidism.
Benign thyroid cysts or nodules: Localized growths within the gland can cause visible swelling.
Thyroid cancer: Malignant changes within the gland resulting in abnormal enlargement.
Risk Factors for Goiter
Certain individuals have a higher likelihood of developing goiter, including:
People with chronic medical conditions (e.g., chronic kidney disease, inflammatory bowel disease) that impair iodine absorption or excretion.
Individuals taking lithium, amiodarone, or other drugs that affect thyroid function.
Those exposed to radiation, especially during cancer therapy (radiation or chemotherapy).
People living in iodine-deficient regions.
Factors That Increase the Risk of Developing Goiter
Age: More common in individuals over 40 years old.
Sex: Women are more likely than men to develop goiter or thyroid disorders.
Pregnancy: Elevated human chorionic gonadotropin (hCG) levels can overstimulate the thyroid, causing temporary enlargement.
Menopause: Hormonal changes can increase susceptibility to thyroid dysfunction.
Autoimmune diseases: A personal or family history of autoimmune disorders increases risk.
Family history: Having relatives with thyroid disease or thyroid cancer raises the likelihood of goiter.
Lifestyle and environment: Poor diet, stress, and environmental toxins can also contribute to thyroid enlargement.
Diagnosis and Treatment of Goiter
Diagnostic Methods
Several tests can help determine the type and cause of goiter:
Thyroid ultrasound: Helps assess the size, shape, and presence of nodules or cysts in the thyroid gland.
Blood tests: Measure thyroid hormone levels (TSH, T3, T4) and detect thyroid antibodies (anti-TPO, anti-thyroglobulin, or TSHR antibodies) in autoimmune thyroid diseases.
Fine-needle aspiration biopsy: Performed if nodules are detected to evaluate for malignancy.
CT or MRI scans: Used when the goiter is very large or extends into the chest to assess compression on surrounding structures.
Effective Treatment Options
Treatment for goiter depends on its underlying cause, size, symptoms, and impact on thyroid hormone levels.
Observation: Small, asymptomatic goiters with normal thyroid function may not require immediate treatment. Regular monitoring and dietary adjustments (especially iodine intake) are recommended.
Medication:
- For hypothyroidism: Thyroid hormone replacement therapy (levothyroxine or liothyronine) helps normalize hormone levels and may reduce goiter size in some cases.
- For thyroid inflammation: Nonsteroidal anti-inflammatory drugs (NSAIDs) such as aspirin or corticosteroids may be prescribed.
- For hyperthyroidism: Antithyroid medications or radioactive iodine (I-131) can reduce excess hormone production and shrink the gland.
Radioactive iodine therapy (RAI): Oral administration of I-131 selectively destroys overactive thyroid tissue, helping to shrink goiters caused by hyperthyroidism.
Surgery (Thyroidectomy): Indicated when the goiter is excessively large, causes breathing or swallowing difficulties, does not respond to medical therapy, or is suspected to be cancerous. Depending on the case, partial or total removal of the thyroid may be necessary. After total thyroidectomy, lifelong thyroid hormone replacement is usually required.
Home care and dietary management: Dietary iodine intake should be adjusted according to the type of thyroid disorder—either increasing or decreasing as advised by a healthcare professional.
Lifestyle and Prevention of Goiter
Healthy Habits to Help Manage Goiter
Adopting the right lifestyle habits plays an important role in preventing the progression of goiter and improving overall thyroid health.
Daily habits:
Follow your doctor’s instructions carefully. Take medications exactly as prescribed and never stop treatment without consulting your healthcare provider.
Maintain a positive mindset. Mental well-being has a significant impact on recovery and hormone balance.
Manage stress effectively. Practice relaxation techniques such as yoga, meditation, or gentle exercise.
Monitor your symptoms. Contact your doctor immediately if you experience unusual swelling, fatigue, or voice changes.
Schedule regular check-ups. Routine medical visits help track thyroid size and hormone levels, ensuring timely treatment adjustments.
Nutrition Tips for Thyroid Health
Diet plays a key role in both preventing and managing goiter.
Ensure adequate iodine intake through daily meals — the recommended amount for adults is about 150–200 µg per day.
Avoid excessive consumption of goitrogenic foods (which can interfere with thyroid hormone production), such as cabbage, broccoli, kale, soybeans, millet, and processed or high-fat foods — especially if you already have iodine deficiency.
Opt for a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats to support optimal metabolism.
Effective Prevention Strategies
You can reduce your risk of developing goiter or other thyroid disorders by following these recommendations:
Treat chronic illnesses promptly, especially conditions that affect iodine absorption or metabolism.
Get regular health screenings to detect early signs of thyroid dysfunction.
Seek medical attention if you notice symptoms of:
- Hypothyroidism: fatigue, drowsiness, cold intolerance, muscle weakness, dry skin, constipation, or memory problems.
- Hyperthyroidism: weight loss, sweating, frequent urination, rapid heartbeat, high blood pressure, anxiety, insomnia, or menstrual irregularities.
Pay special attention to children showing signs of hyperthyroidism, such as rapid growth or behavioral changes.
