Myocardial Infarction: Symptoms, Causes, and Treatment
Overview of Myocardial Infarction
Myocardial infarction occurs when blood flow to a portion of the heart muscle decreases or stops completely due to a thrombus blocking a coronary artery. This is a serious event that causes sudden ischemia of the heart muscle.
Acute myocardial infarction (AMI) is an emergency condition that occurs when one or more branches of the coronary arteries—the vessels supplying blood to the heart—become suddenly blocked. This interruption in blood flow leads to injury or necrosis of the heart muscle that is deprived of oxygen. Myocardial infarction can result in severe complications; without timely emergency treatment to restore circulation, it may cause permanent heart damage or even death.
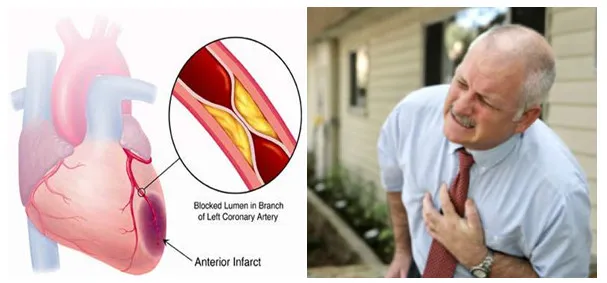
Symptoms of Myocardial Infarction
The typical first symptom of a heart attack is deep, visceral pain described as aching or crushing pressure. The pain often radiates to the back, jaw, left or right arm, shoulder, or multiple of these areas. It resembles angina but is usually more intense and prolonged, often accompanied by shortness of breath, nausea, or vomiting. Rest or nitroglycerin provides little or only temporary relief.
However, some cases present mild or atypical discomfort; about 20% of acute myocardial infarctions are silent, showing no obvious symptoms or vague ones that patients fail to recognize—especially in individuals with diabetes. Some may misinterpret the pain as indigestion, particularly when spontaneous relief occurs after burping or taking antacids.
Certain patients may experience syncope (fainting).
Women are more likely to have atypical chest discomfort, while elderly patients may report shortness of breath rather than the typical ischemic chest pain.
Physical examination may reveal pale, cool, or clammy skin, and sometimes peripheral or central cyanosis. Pulse and blood pressure can fluctuate; many patients initially present with some degree of hypertension due to pain.
Heart sounds may be muffled; a fourth heart sound (S4) is common. A soft systolic murmur at the apex may occur, reflecting papillary muscle dysfunction. During initial assessment, the presence of a loud murmur or pericardial friction rub may suggest pre-existing heart disease or an alternative diagnosis.
Possible Complications of Myocardial Infarction
Common complications include:
- Sudden cardiac death, the most severe outcome of myocardial infarction.
- Cardiac arrhythmias, occurring in more than 90% of patients.
- Weak, rapid pulse, low blood pressure, and excessive sweating.
- Thrombus formation, which can travel and block blood vessels elsewhere in the body, increasing the risk of pulmonary embolism or stroke.
- Cardiac rupture in severe cases.

When to See a Doctor
If any of the symptoms above occur, seek medical attention immediately for evaluation and management. Early diagnosis and treatment can reduce the risk of complications and improve recovery outcomes.
Causes and Risk Factors of Myocardial Infarction
Causes of Myocardial Infarction
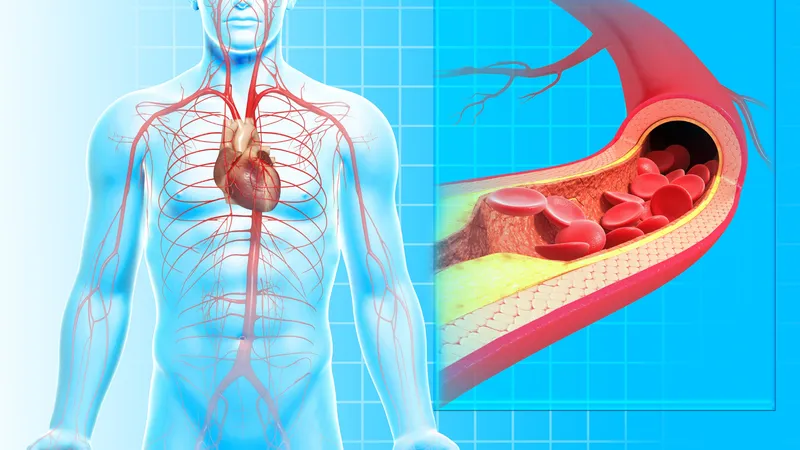
The heart is the main organ of the cardiovascular system, which also includes various types of blood vessels. Among these, the arteries play a vital role — they carry oxygen-rich blood throughout the body and to all organs.
The coronary arteries specifically deliver oxygenated blood to the heart muscle itself. When these arteries become blocked or narrowed due to the buildup of plaque (a mixture of fat, cholesterol, and other substances), blood flow to the heart can be significantly reduced or completely stopped. This interruption of blood supply is what causes a heart attack (myocardial infarction).
Who Is at Risk of Myocardial Infarction?
Certain individuals are more likely to develop myocardial infarction due to underlying health conditions or lifestyle factors, including:
High blood pressure (hypertension): Can damage arteries and accelerate plaque buildup.
High blood sugar (diabetes): May injure blood vessels and eventually lead to coronary artery disease.
Smoking: Increases the risk of myocardial infarction and contributes to other cardiovascular conditions.
Age: The risk of heart attack increases with age — men are more likely to have one after age 45, and women after age 55.
Family history: You are at higher risk if a close family member developed heart disease early — particularly if a male relative was affected before age 55 or a female relative before age 65.
Stress: Although evidence remains limited, acute or chronic stress may trigger a heart attack. Managing stress and anxiety can help reduce long-term cardiovascular risk.
Lack of physical activity: Regular exercise helps maintain a healthy weight and supports normal blood pressure, cholesterol, and glucose levels.
Drug use: Certain drugs, such as cocaine or amphetamines, can constrict blood vessels and increase the risk of a heart attack.
Preeclampsia: A history of high blood pressure during pregnancy increases the risk of heart disease later in life.

Additional Risk Factors
Other common factors that may increase the likelihood of developing myocardial infarction include:
- Older age
- Family history of heart disease
- Smoking
- Sedentary lifestyle (low physical activity)
Diagnosis and Treatment of Myocardial Infarction
Diagnostic Tests and Procedures
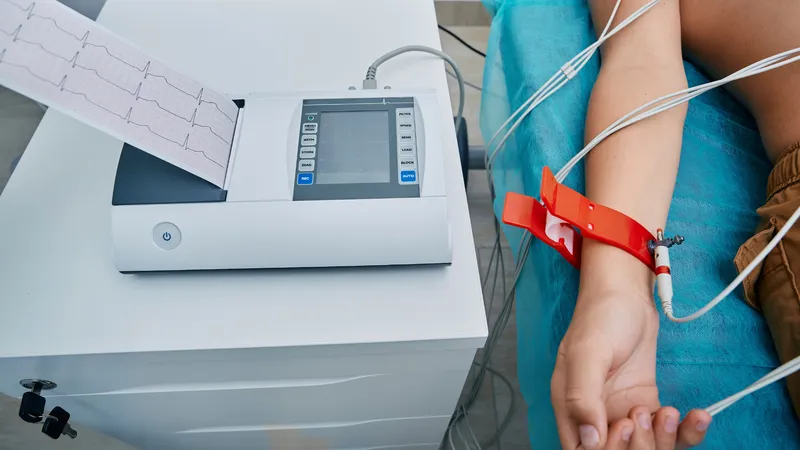
Electrocardiogram (ECG or EKG)
An electrocardiogram is the most important diagnostic test and should be performed within 10 minutes of initial evaluation.
It helps detect electrical changes in the heart that occur when blood flow is blocked, allowing physicians to identify the location and severity of myocardial injury.
Cardiac Biomarkers
Cardiac biomarkers (serum markers of myocardial cell injury) include heart enzymes — such as creatine kinase-MB (CK-MB) — and structural proteins such as troponin I, troponin T, and myoglobin. These substances are released into the bloodstream when heart muscle cells die.
Different biomarkers appear at various times after the onset of injury and decline at different rates. Their sensitivity and specificity vary, but cardiac troponins (cTn) are currently the most specific and sensitive indicators of myocardial injury.
Recently, high-sensitivity cardiac troponin (hs-cTn) assays have become widely available, offering even greater accuracy for early detection.
Coronary Angiography
Coronary angiography is both a diagnostic and therapeutic procedure, often combined with percutaneous coronary intervention (PCI) — such as angioplasty or stent placement.
When feasible, emergency angiography and primary PCI should be performed as soon as possible after the onset of acute myocardial infarction.
Early PCI (within 3–4 hours of symptom onset) significantly improves outcomes and can restore blood flow to the affected area, preventing further damage.
Effective Treatment Approaches for Myocardial Infarction
Pre-Hospital Care
Immediate management focuses on:
- Oxygen therapy
- Aspirin administration
- Nitrate therapy for pain relief
- Rapid transport to an appropriate medical center
Medication Therapy
Treatment aims to restore blood flow, prevent clot formation, and protect the heart. Commonly used medications include:
- Antiplatelet drugs: Aspirin, clopidogrel, or both (prasugrel or ticagrelor as alternatives to clopidogrel)
- Anticoagulants: Unfractionated or low-molecular-weight heparin, or bivalirudin
- Glycoprotein IIb/IIIa inhibitors: Used when PCI is performed to prevent platelet aggregation
- Nitrates: Typically nitroglycerin to relieve chest pain and improve blood flow
- Antihypertensive drugs: To control blood pressure and reduce cardiac workload
- ACE inhibitors: Help improve survival and reduce strain on the heart
- Statins: Lower cholesterol and prevent further plaque formation
Reperfusion Therapy
Reperfusion therapy aims to restore blood flow to the heart muscle and may include:
- Thrombolytic (fibrinolytic) therapy — using drugs to dissolve blood clots
- Coronary angioplasty and stent placement (PCI)
- Coronary artery bypass grafting (CABG) in severe or complex cases
Post-Discharge Care and Long-Term Management
After recovery, patients require:
- Cardiac rehabilitation programs to restore physical function
- Lifestyle modifications such as quitting smoking, adopting a heart-healthy diet, and exercising regularly
- Ongoing medical therapy for chronic coronary artery disease to prevent recurrence
Lifestyle and Prevention of Myocardial Infarction
Healthy Lifestyle Habits to Manage and Prevent Myocardial Infarction
Adopting a heart-healthy lifestyle plays a crucial role in slowing the progression of myocardial infarction and reducing the risk of future cardiac events.
Lifestyle Recommendations:
- Follow your doctor’s instructions carefully regarding medication, treatment, and follow-up appointments.
- Maintain a positive and active lifestyle — manage stress and avoid prolonged emotional tension.
- Seek medical advice immediately if you experience any unusual symptoms or changes in your condition during treatment.
- Schedule regular health checkups to monitor your recovery and allow your doctor to adjust treatment as needed.
- Stay optimistic. A positive mindset greatly influences recovery. Talk to trusted people, share with family members, care for pets, read, or engage in relaxing activities that bring you comfort.
Healthy Diet for Heart Protection
A balanced diet supports heart health and helps prevent recurrence of myocardial infarction. Recommended foods include:
- Whole grains
- Fresh vegetables
- Fruits
- Lean protein sources (such as fish, skinless poultry, or legumes)
Avoid foods high in saturated fat, salt, or refined sugar to maintain optimal heart function.
Effective Prevention Tips for Myocardial Infarction
To effectively prevent myocardial infarction, consider the following steps:
- Control blood pressure to reduce strain on the heart and arteries.
- Regulate blood sugar and cholesterol levels through medication, diet, and regular monitoring.
- Exercise regularly, aiming for at least 30 minutes of moderate activity most days of the week.
