Heart Valve Regurgitation: Causes, Symptoms, and Treatment
Understanding Heart Valve Regurgitation
What Is Heart Valve Regurgitation?
In a healthy heart, valves open and close precisely to ensure that blood flows in one direction. When a valve fails to close completely, a portion of blood leaks backward instead of moving forward through the heart. Depending on which valve is affected, this condition can interfere with the heart’s ability to pump efficiently.
The heart has four valves, each with a specific function:
- Mitral valve – between the left atrium and left ventricle
- Tricuspid valve – between the right atrium and right ventricle
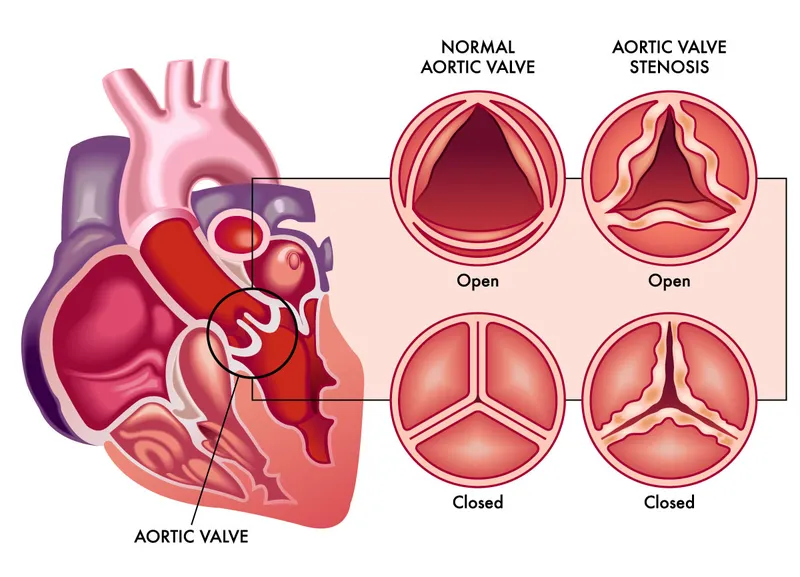
- Aortic valve – between the left ventricle and the aorta
- Pulmonary valve – between the right ventricle and the pulmonary artery
Accordingly, regurgitation can be classified as:
- Mitral regurgitation (MR)
- Tricuspid regurgitation (TR)
- Aortic regurgitation (AR)
- Pulmonary regurgitation (PR)
Severity Levels
Heart valve regurgitation is typically graded on a four-point scale based on how much blood leaks backward:
- Grade 1/4: Mild regurgitation (usually asymptomatic)
- Grade 2/4: Moderate regurgitation
- Grade 3/4: Severe regurgitation
- Grade 4/4: Very severe regurgitation, often associated with major complications such as heart failure or arrhythmia
Symptoms of Heart Valve Regurgitation
Symptoms vary depending on which valve is affected and how severe the leakage is. Many cases are mild and may go unnoticed for years, while severe regurgitation can cause disabling symptoms or even life-threatening complications.
1. Tricuspid Regurgitation (TR)
Overview:
Often secondary to right ventricular enlargement or pulmonary hypertension, tricuspid regurgitation can also result from infection (infective endocarditis), trauma, or congenital defects.
Common Symptoms:
- Enlarged liver and spleen
- Abdominal swelling (ascites)
- Swelling in legs and ankles (peripheral edema)
- Pulsating neck veins due to elevated jugular venous pressure
In advanced stages, patients may notice visible neck pulsations. If pulmonary hypertension is the underlying cause, fatigue, shortness of breath, and reduced exercise tolerance are common. Infective endocarditis can cause fever and general malaise.
2. Pulmonary Regurgitation (PR)
Overview:
A rare condition, pulmonary regurgitation typically occurs secondary to pulmonary hypertension or after surgical procedures on the pulmonary valve.
Symptoms:
Most patients are asymptomatic in early stages. As the disease progresses, shortness of breath during exertion, fatigue, or signs of right-sided heart failure may appear, such as fluid retention or swelling in the lower limbs.
3. Mitral Regurgitation (MR)
Overview:
Mitral regurgitation occurs when blood leaks backward from the left ventricle into the left atrium during contraction. It may result from mitral valve prolapse, rheumatic heart disease, ischemic damage, or congenital abnormalities.
Acute MR:
Develops suddenly, often due to rupture of the papillary muscle (from myocardial infarction) or infective endocarditis. Symptoms can be dramatic:
- Sudden, severe shortness of breath (even at rest)
- Cough producing pink frothy sputum
- Chest pain, fatigue, and low blood pressure
Chronic MR:
May remain silent for years. As the heart compensates, the patient might gradually develop:
- Fatigue or weakness
- Dyspnea on exertion
- Orthopnea (shortness of breath when lying flat)
- Paroxysmal nocturnal dyspnea (sudden nighttime breathlessness)
- Palpitations (possible atrial fibrillation)
- Weight gain and peripheral edema
- Hepatomegaly or pleural effusion
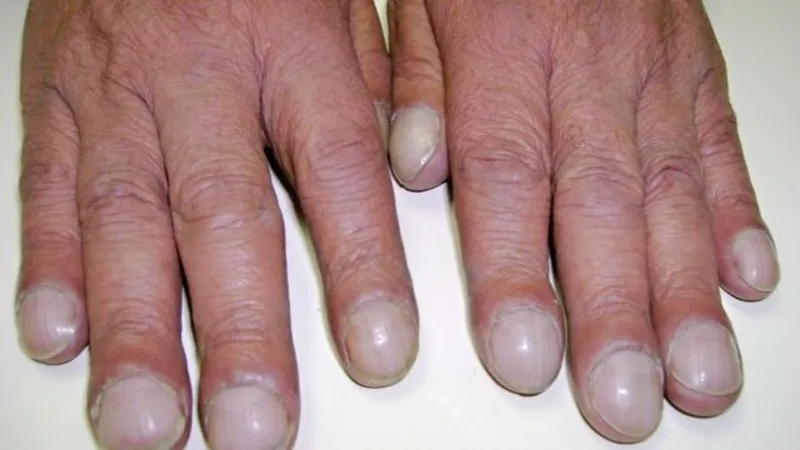
Clinical signs: A pansystolic murmur, finger clubbing, cyanosis, or even heart enlargement on imaging.
4. Aortic Regurgitation (AR)
Overview:
Aortic regurgitation allows blood to flow backward from the aorta into the left ventricle. It can result from congenital bicuspid aortic valve, rheumatic disease, connective tissue disorders (Marfan syndrome), or infections.
Symptoms:
- Shortness of breath (especially during exertion or lying down)
- Chest pain or pressure (angina-like)
- Palpitations or pounding heartbeats
- Headaches and dizziness
- Fatigue or reduced stamina
Because AR progresses slowly, symptoms may take decades to develop. Once left ventricular function declines, heart failure can occur rapidly if left untreated.
Possible Complications
Each type of valve regurgitation carries specific risks, but in general, prolonged valve leakage can disrupt blood flow and cause lasting cardiac damage:
| Valve Involved | Major Complications |
| Tricuspid | Liver congestion, ascites, venous thrombosis |
| Pulmonary | Ventricular arrhythmias, progressive right heart failure, sudden cardiac death |
| Mitral | Heart failure, atrial fibrillation, stroke, pulmonary hypertension, ventricular dilation |
| Aortic | Systolic dysfunction, congestive heart failure, ischemic cardiomyopathy, arrhythmia, sudden death |
When to See a Doctor
You should seek medical evaluation if you experience any of the following symptoms:
- Chest pain or discomfort that appears suddenly or doesn’t go away
- Pain radiating to the neck, jaw, or arms
- Dizziness, fainting, or cold sweats
- Rapid or irregular heartbeat
- Shortness of breath, especially during activity or at night
- Swelling in your legs, feet, or abdomen
- Rapid weight gain due to fluid retention
- Stroke-like symptoms such as facial drooping, weakness, or speech difficulty
Causes of Heart Valve Regurgitation
Heart valve regurgitation can arise from a variety of structural, infectious, or systemic conditions that impair valve function. The underlying cause often determines the type of valve affected and the severity of leakage. Below is an overview of the major causes categorized by valve type.
Tricuspid Regurgitation (TR)
Tricuspid regurgitation can be secondary (functional) or primary (organic) in origin.
Secondary (Functional) TR
This is the most common form, usually resulting from dilation of the right ventricle or pulmonary hypertension that stretches the tricuspid annulus.
Common secondary causes include:
- Left-sided heart failure
- Mitral valve stenosis or regurgitation
- Chronic lung diseases such as pulmonary embolism or pulmonary hypertension
- Pulmonary valve stenosis
- Hyperthyroidism (thyrotoxic heart disease)
Primary (Organic) TR
Primary tricuspid regurgitation involves direct damage to the tricuspid valve leaflets or supporting structures.
It is rare in adults but may occur in congenital or acquired settings.
Possible causes:
- Congenital anomalies (e.g., Ebstein’s anomaly)
- Trauma or injury to the chest
- Infective endocarditis affecting the tricuspid valve
- Rheumatic heart disease
- Carcinoid syndrome, which can produce fibrotic deposits on the valve
- Myxomatous degeneration or connective tissue disorders such as Marfan syndrome
- Drug-induced damage, such as from certain appetite suppressants or ergot-derived medications
- Post-cardiac procedures, including pacemaker or catheter-related injury
Pulmonary Regurgitation (PR)
Pulmonary regurgitation is relatively rare and often discovered incidentally during echocardiography.
Common causes:
- Previous surgical or interventional repair (such as after tetralogy of Fallot correction or balloon valvuloplasty)
- Pulmonary hypertension, which increases the pressure load on the valve
- Carcinoid syndrome
- Infective endocarditis
- Rheumatic heart disease
- Congenital absence or malformation of the pulmonary valve
In many post-surgical cases, mild pulmonary regurgitation is expected and well-tolerated; however, long-term follow-up is essential to monitor for right ventricular dilation and functional decline.
Mitral Regurgitation (MR)
Mitral regurgitation has both organic and functional causes, involving damage to the mitral valve leaflets, chordae tendineae, papillary muscles, or surrounding myocardium.
Major causes include:
- Mitral valve prolapse (degenerative or myxomatous changes)
- Congenital valve malformations
- Rheumatic heart disease
- Infective endocarditis
- Papillary muscle rupture due to myocardial infarction
- Ischemic dysfunction of papillary muscles
- Dilated or hypertrophic cardiomyopathy
- Atrial fibrillation and chronic left atrial dilation
- Heart failure with secondary annular dilation
Aortic Regurgitation (AR)
Aortic regurgitation may stem from diseases affecting either the valve leaflets or the aortic root.
Valve-related causes:
- Congenital bicuspid aortic valve
- Infective endocarditis
- Rheumatic fever
- Trauma or iatrogenic damage following cardiac procedures
Aortic root or ascending aorta-related causes:
- Aortic root dilation (age-related or due to connective tissue disorders)
- Aortic dissection, which can separate the valve commissures
- Inflammatory or autoimmune diseases, such as:
- Ankylosing spondylitis
- Psoriatic arthritis
- Reactive arthritis
- Ulcerative colitis (as part of systemic inflammation)
In all these cases, structural changes in the aortic root prevent proper closure of the aortic valve cusps, resulting in regurgitation.

Risk Factors for Heart Valve Regurgitation
While anyone can develop valve regurgitation, certain groups are at higher risk depending on the type of valve affected.
Population and Demographic Risks
Aortic regurgitation is more common in men, and its prevalence increases with age, especially after 50.
Pulmonary regurgitation is more frequent among adolescents and is often benign. In individuals who have undergone tetralogy of Fallot repair, regurgitation may appear 1–20 years after surgery, warranting regular cardiac imaging.
Tricuspid regurgitation shows no significant difference across sex or race, according to U.S. epidemiological studies.
General Risk Factors
- Advancing age – age-related degeneration of valve tissue
- Family history of valvular or congenital heart disease
- Unhealthy lifestyle habits, such as smoking, poor diet, or sedentary behavior
- Chronic hypertension – increases the workload and pressure on the valves
- Autoimmune diseases such as lupus or rheumatic fever
- Use of certain medications (e.g., ergot alkaloids, appetite suppressants)
- Medical devices in the heart – pacemaker leads, catheters, or prosthetic valves
- Gender, with men more likely to develop aortic or mitral valve disease

Diagnosis and Treatment of Heart Valve Regurgitation
The diagnosis of heart valve regurgitation requires a combination of clinical assessment, imaging studies, and functional testing to evaluate both the structure of the heart and its hemodynamic performance. Early and accurate diagnosis plays a vital role in preventing long-term complications such as heart failure or arrhythmia.
Diagnostic Methods
When heart valve regurgitation is suspected, your healthcare provider will begin with a detailed medical history and physical examination, listening carefully for characteristic heart murmurs or signs of heart enlargement. To confirm the diagnosis and assess its severity, several diagnostic tests may be ordered:
1. Echocardiography (ECHO)
Primary diagnostic tool for detecting and grading valve regurgitation.
Evaluates valve morphology, chamber size, blood flow direction, and regurgitant volume using Doppler imaging.
Determines whether the regurgitation is due to structural damage (e.g., leaflet prolapse) or functional causes (e.g., chamber dilation).
2. Chest X-ray
Helps detect cardiomegaly (enlarged heart), pulmonary congestion, or pleural effusion.
May suggest chronic pressure overload or heart failure secondary to valve disease.
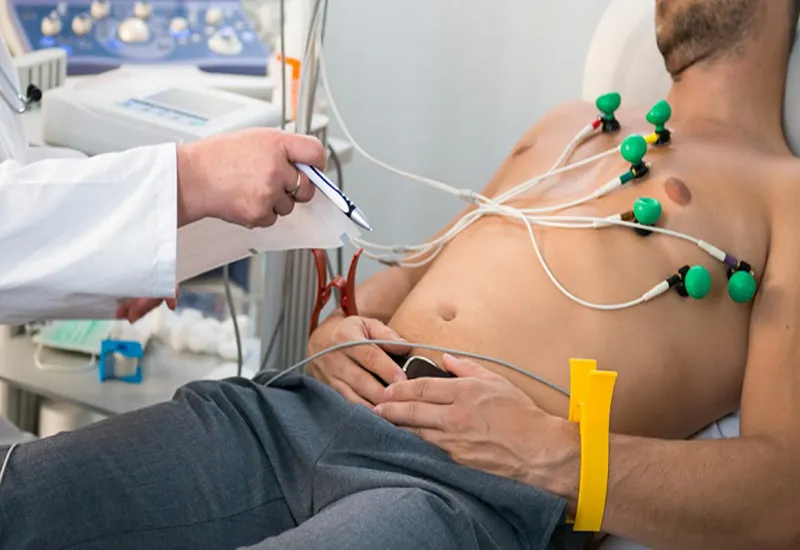
3. Electrocardiogram (ECG)
Evaluates electrical activity of the heart.
Detects atrial fibrillation, ventricular hypertrophy, or ischemic changes that may coexist with valve dysfunction.
4. Blood Tests
Used to identify infection (in suspected endocarditis), inflammation, hepatic dysfunction (in right-sided failure), and cardiac biomarkers such as BNP or NT-proBNP to assess heart failure severity.
5. Cardiac MRI
Provides detailed structural imaging when echocardiography results are inconclusive.
Particularly valuable in mitral regurgitation and aortic regurgitation to quantify regurgitant fraction and ventricular volumes.
6. Cardiac Catheterization
Measures chamber pressures and evaluates pulmonary hypertension or coronary artery disease prior to surgery.
May be indicated when noninvasive imaging is insufficient or conflicting.
Treatment Options for Heart Valve Regurgitation
The management of valve regurgitation depends on:
- The type and severity of the valve involved
- The presence of symptoms or ventricular dysfunction
- The underlying cause (structural vs. secondary)
A multidisciplinary approach — involving cardiologists, surgeons, and imaging specialists — is essential.
Tricuspid Regurgitation (TR)
Treatment goals include:
- Managing the underlying cause, such as left-sided heart failure or pulmonary hypertension.
- Using diuretics to relieve symptoms of volume overload (e.g., edema, ascites).
- Surgical or transcatheter valve repair/replacement is indicated in severe TR or when combined with other valve surgery.
Women with significant TR should receive pre-pregnancy counseling, as pregnancy increases blood volume and cardiac workload.
Pulmonary Regurgitation (PR)
Commonly occurs after surgical repair of tetralogy of Fallot.
Regular annual echocardiography is crucial to monitor right ventricular size and function.
Surgical valve replacement or percutaneous pulmonary valve implantation may be necessary if symptoms develop or the right ventricle dilates significantly.
Medical management is reserved for secondary causes, such as pulmonary hypertension.
Mitral Regurgitation (MR)
Treatment depends on whether the condition is acute or chronic:
Acute MR (e.g., due to papillary muscle rupture or endocarditis) requires emergency surgery.
Chronic MR may initially be managed medically using:
- Afterload-reducing agents (ACE inhibitors, ARBs)
- Diuretics for congestion
- Beta-blockers for rate control in atrial fibrillation
Surgical intervention (mitral valve repair preferred over replacement) is recommended when:
- Symptoms appear (NYHA class II or higher)
- Left ventricular ejection fraction (LVEF) < 60%
- Left ventricular end-systolic diameter (LVESD) ≥ 40 mm
Aortic Regurgitation (AR)
Management varies depending on disease stage:
Acute severe AR — a surgical emergency requiring prompt aortic valve replacement (AVR).
Chronic AR — categorized into Stages A (at risk), B (progressive), and C (symptomatic or ventricular dysfunction).
- Medical therapy (vasodilators like nifedipine or ACE inhibitors) may be used to reduce afterload.
- Surgery is indicated for symptomatic patients or asymptomatic individuals with LV dysfunction.
Lifestyle Modifications and Prevention
Healthy Lifestyle Habits
Although structural valve disorders may not always be preventable, adopting a heart-healthy lifestyle can slow progression and improve quality of life.
- Adhere to medical treatment and attend regular follow-up appointments.
- Monitor symptoms (shortness of breath, fatigue, swelling) and report changes promptly.
- Ask your doctor about safe exercise levels — activities should match the severity of valve disease.
- Manage blood pressure diligently to reduce stress on the valves.
- Avoid excessive alcohol and quit smoking.
Heart-Healthy Diet
- Focus on a balanced diet rich in fruits, vegetables, whole grains, and lean proteins.
- Limit saturated fats, trans fats, salt, and refined sugars.
- Include omega-3 fatty acids (e.g., from fish, flaxseed) for vascular health.
- Stay hydrated and maintain a healthy body weight.
Effective Prevention Strategies
Complete prevention is not always possible — particularly in congenital or degenerative cases — but the following measures can significantly reduce risk and complications:
- Treat throat infections early to prevent rheumatic fever.
- Maintain optimal blood pressure and cholesterol levels.
- Exercise regularly, as advised by a healthcare provider.
- Limit alcohol and avoid stimulant or appetite-suppressant drugs.
- Monitor for autoimmune or connective tissue disorders (e.g., lupus, Marfan syndrome).
- Adhere strictly to prescribed medications and never self-adjust dosages.
- For those with prior valve surgery or prosthetic valves, antibiotic prophylaxis may be recommended before certain dental or invasive procedures to prevent infective endocarditis.
