Heart Failure: Symptoms, Causes, and Treatment
Understanding Heart Failure
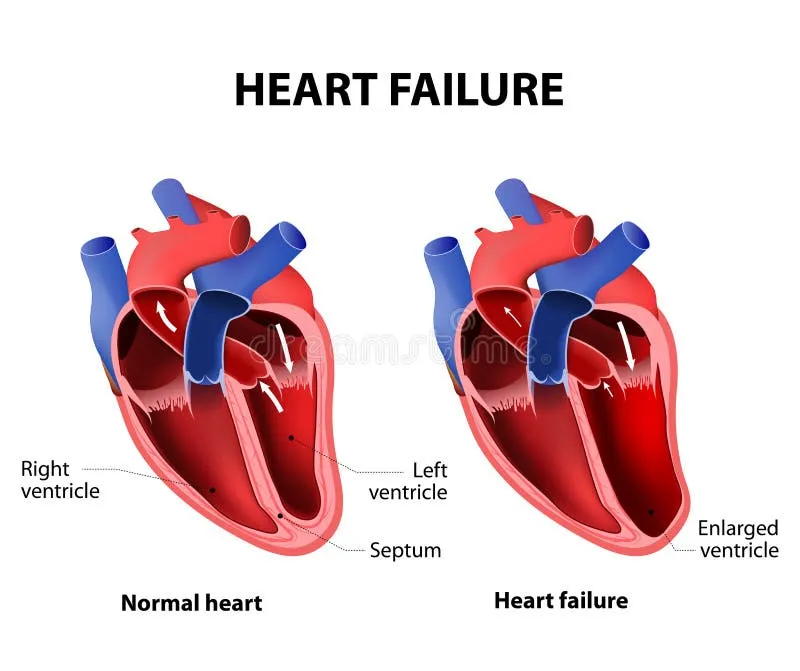
Heart failure (HF) is not a sudden event but a progressive syndrome that develops when the heart’s pumping capacity is no longer sufficient to meet the body’s metabolic demands. The heart, a muscular organ responsible for circulating blood, can weaken due to a variety of underlying conditions—such as coronary artery disease, hypertension, or prior heart attacks.
When cardiac output falls, blood may back up into the lungs, causing congestion and shortness of breath. Over time, reduced perfusion to vital organs triggers a cascade of compensatory mechanisms—like increased heart rate or fluid retention—which initially help maintain circulation but eventually worsen the disease.
In medical terms, heart failure can be classified as:
- Left-sided heart failure: Blood backs up into the lungs, causing pulmonary congestion.
- Right-sided heart failure: Blood pools in the veins, leading to swelling in the legs, ankles, and abdomen.
- Systolic vs. diastolic failure: Depending on whether the heart has trouble contracting or relaxing properly.
Understanding which type of heart failure a patient has is essential for tailoring treatment and improving outcomes.
Symptoms of Heart Failure
Heart failure manifests differently from person to person, depending on its severity and whether the left or right side of the heart is affected. Common clinical signs and symptoms include:
- Shortness of breath (dyspnea) during activity or when lying flat — caused by fluid buildup in the lungs that impairs gas exchange.
- Sudden nighttime breathlessness (paroxysmal nocturnal dyspnea): Waking up abruptly at night gasping for air, often relieved by sitting upright.
- Chest discomfort or pressure: May indicate reduced oxygen supply to the heart muscle (myocardial ischemia).
- Rapid or irregular heartbeat (palpitations): The heart tries to compensate for poor pumping efficiency.
- Swelling (edema) in the legs, ankles, or feet — due to fluid accumulation in tissues.
- Persistent cough or wheezing: May be dry or produce frothy sputum, occasionally tinged with blood if lung congestion is severe.
- Unexplained rapid weight gain: Often a sign of fluid retention rather than fat accumulation.
- Fatigue and weakness: Muscles receive less oxygen and nutrients, making even simple activities exhausting.
- Difficulty concentrating or confusion: Reduced blood flow to the brain may impair cognitive function.
- Abdominal bloating or discomfort: Fluid may accumulate in the abdominal cavity (ascites).
- Loss of appetite or nausea: The digestive system becomes congested, and reduced circulation affects metabolism.
These symptoms can develop gradually or worsen suddenly during acute exacerbations.

When to See a Doctor
Seek medical attention promptly if you experience persistent or worsening symptoms such as shortness of breath, swelling in your legs, rapid weight gain, or chest pain. Early diagnosis and treatment can significantly improve quality of life and slow disease progression.
Individuals with risk factors such as high blood pressure, diabetes, coronary artery disease, or a history of heart attack should have regular heart evaluations—even if they feel well—to detect early signs of cardiac dysfunction.
Causes of Heart Failure
Heart failure rarely develops from a single cause. Instead, it often arises as the final stage of multiple underlying cardiovascular or systemic conditions that gradually weaken or damage the heart muscle.
1. Coronary Artery Disease (CAD)
The most common cause of heart failure is coronary artery disease—a condition in which fatty plaques (atherosclerosis) narrow or block the arteries supplying blood to the heart. Reduced blood flow deprives the myocardium of oxygen, leading to chest pain (angina) or myocardial infarction (heart attack). Repeated or severe damage to heart tissue diminishes its ability to contract effectively, eventually resulting in heart failure.
2. Hypertension (High Blood Pressure)
Long-term, uncontrolled high blood pressure forces the heart to work harder to pump blood against increased arterial resistance. Over time, the heart muscle thickens (left ventricular hypertrophy) and becomes stiff or fatigued, impairing its pumping efficiency. This gradual overexertion is one of the most frequent precursors to chronic heart failure.
3. Cardiomyopathy
Cardiomyopathy refers to diseases that directly affect the heart muscle, making it weak, enlarged, or abnormally rigid. It can be caused by genetic factors, viral infections (myocarditis), chronic alcohol use, drug toxicity (e.g., from chemotherapy agents), or metabolic disorders. Dilated and hypertrophic cardiomyopathies are the most common subtypes associated with heart failure.
4. Heart Valve Disorders
When heart valves become narrowed (stenotic) or fail to close properly (regurgitant), blood flow within the heart is disrupted. The heart must pump harder to compensate for this inefficiency, which can ultimately exhaust the cardiac muscle. Valvular disease due to rheumatic fever, endocarditis, or age-related degeneration remains a significant cause of heart failure worldwide.
5. Congenital Heart Disease
Structural abnormalities present at birth—such as septal defects or malformed valves—can overload the heart and accelerate the onset of heart failure, particularly in children or adults who have not undergone corrective surgery.
6. Arrhythmias
Irregular heart rhythms, including atrial fibrillation or ventricular tachycardia, can reduce the heart’s ability to pump effectively. Chronic arrhythmias increase the risk of both systolic and diastolic heart failure.
7. Other Contributing Factors
Several non-cardiac factors can also lead to or worsen heart failure:
- Chronic alcohol abuse: Alcoholic cardiomyopathy and direct myocardial toxicity.
- Diabetes mellitus: Causes both microvascular and macrovascular complications that weaken the heart.
- Severe anemia: Reduces oxygen delivery, forcing the heart to compensate by pumping harder.
- Thyroid disorders: Both hyperthyroidism and hypothyroidism can impair heart function.
- Pregnancy-related cardiomyopathy: Postpartum women may develop peripartum cardiomyopathy, a rare but serious cause of heart failure.
- Certain medications or toxins: Long-term use of anthracyclines, NSAIDs, or illicit drugs (e.g., cocaine, amphetamines) may damage the heart muscle.
Risk Factors for Heart Failure
Who Is at Risk?
Anyone can develop heart failure, but the likelihood increases with the presence of chronic cardiovascular conditions such as:
- High blood pressure
- Coronary artery disease
- Heart valve disease
- Prior heart attack
- Cardiomyopathy
Early identification and control of these conditions are essential for preventing the progression to heart failure.
Major Risk Factors That Increase the Likelihood of Heart Failure
- Chronic alcohol use or alcohol toxicity — causes direct myocardial damage.
- Obesity — increases cardiac workload and promotes hypertension and diabetes.
- Diabetes mellitus — accelerates vascular damage and heart muscle dysfunction.
- Sedentary lifestyle — weakens cardiovascular endurance and metabolic regulation.
- Pregnancy or postpartum state — in rare cases, can lead to peripartum cardiomyopathy.
- Advancing age — natural decline in cardiac reserve increases susceptibility.
- Family history of heart disease — genetic factors can predispose individuals to cardiomyopathy or arrhythmia.
Diagnosis and Treatment of Heart Failure
Heart failure diagnosis relies on a combination of clinical evaluation, laboratory findings, and imaging studies. Because its symptoms often overlap with other cardiopulmonary conditions, a thorough assessment is essential to confirm the diagnosis and identify the underlying cause.
Clinical Evaluation
The first step in diagnosing heart failure is a detailed history and physical examination. Common clinical findings include:
- Shortness of breath (dyspnea) on exertion or when lying flat.
- Fatigue and weakness due to reduced cardiac output.
- Swelling (edema) of the ankles, legs, or abdomen.
- Crackles (rales) heard over the lungs, suggesting fluid accumulation.
- Elevated jugular venous pressure and presence of an S3 gallop.
- Rapid or irregular heartbeat (tachycardia or arrhythmia).
However, these signs may be subtle or absent in the early stages, and similar symptoms can appear in conditions such as chronic obstructive pulmonary disease (COPD), recurrent pneumonia, or severe obesity.
Clinicians should maintain a high index of suspicion in patients with a history of:
- Myocardial infarction or ischemic heart disease
- Hypertension
- Valvular heart disease
- Diabetes mellitus
- Advanced age
Diagnostic Tests and Imaging
1. Chest X-ray
A chest radiograph may show characteristic findings such as:
- Cardiomegaly (enlarged heart silhouette)
- Pleural effusion or interstitial edema
- Kerley B lines indicating pulmonary congestion
- It can also help exclude other causes of dyspnea such as COPD, pneumonia, or lung cancer.
2. Electrocardiogram (ECG)
While ECG alone cannot confirm heart failure, it often reveals abnormalities suggestive of cardiac dysfunction:
- Evidence of prior myocardial infarction
- Left ventricular hypertrophy
- Bundle branch block
- Atrial fibrillation or other arrhythmias
A normal ECG makes the diagnosis of significant heart failure less likely.
3. Echocardiography (Cardiac Ultrasound)
This is the gold standard imaging test for assessing heart structure and function. Echocardiography provides detailed information about:
- Ejection fraction (EF)
- Chamber size and wall motion abnormalities
- Valve function
- Pulmonary artery pressures
It also helps distinguish between systolic (reduced EF) and diastolic (preserved EF) heart failure.
4. Blood Tests
- BNP (B-type natriuretic peptide) or NT-proBNP levels are elevated in most cases of heart failure and help differentiate cardiac from non-cardiac causes of shortness of breath.
- Routine tests include kidney and liver function, electrolytes, thyroid hormones, and complete blood count.
5. Advanced Imaging and Procedures
In selected cases, additional tests such as:
- Cardiac MRI (to evaluate fibrosis or myocarditis)
- Coronary angiography (to assess coronary artery disease)
- Chest ultrasound or CT scan for further evaluation
Treatment of Heart Failure
Treatment aims to alleviate symptoms, improve cardiac performance, prevent hospitalization, and prolong survival. Management strategies are based on the severity of the disease, classified by the NYHA functional class and ejection fraction.
Treatment Goals
Short-term goals:
- Relieve symptoms such as breathlessness and fatigue
- Prevent complications like renal dysfunction or electrolyte imbalance
- Stabilize hemodynamics and reduce neurohormonal activation
Long-term goals:
- Improve cardiac function and quality of life
- Prevent disease progression and hospital readmissions
- Reduce mortality and morbidity
Non-Pharmacologic Management
Lifestyle and behavioral changes form the foundation of all heart failure treatment plans:
- Dietary modification:
- Limit sodium intake (ideally <2g/day in severe heart failure).
- Restrict fluid intake if fluid overload is present.
- Daily weight monitoring: Detect fluid retention early.
- Smoking cessation and alcohol restriction: Abstinence is essential in alcohol-induced cardiomyopathy.
- Regular light-to-moderate exercise: Improves functional capacity and endurance.
- Vaccinations: Annual influenza and 5-year pneumococcal vaccines are recommended.
- Control of comorbidities:
- Manage hypertension, diabetes, and thyroid disorders.
- Address depression, which commonly coexists with chronic heart disease.
- Adequate rest: During acute exacerbations, patients should avoid overexertion.
Pharmacologic Therapy
Medication choice depends on the patient’s clinical profile and ejection fraction. The main drug classes recommended by international heart failure guidelines include:
1. ACE inhibitors (ACEIs) or Angiotensin II receptor blockers (ARBs): Reduce afterload and prevent remodeling of the heart muscle.
2. ARNI (Angiotensin receptor–neprilysin inhibitor): A combination of sacubitril and valsartan shown to reduce mortality and hospitalization rates.
3. Beta-blockers: Improve survival, reduce arrhythmia risk, and allow the heart to pump more efficiently.
4. Diuretics: Relieve symptoms of fluid overload such as edema and dyspnea.
5. Aldosterone antagonists (e.g., spironolactone, eplerenone): Provide additional mortality benefit in systolic heart failure.
6. SGLT2 inhibitors (e.g., dapagliflozin, empagliflozin): Now recommended for both HFrEF and HFpEF, even in non-diabetic patients.
7. Ivabradine: Used in patients with high resting heart rate despite beta-blocker therapy.
8. Digoxin: Helps control symptoms and heart rate in patients with atrial fibrillation and systolic dysfunction.
9. Hydralazine and isosorbide dinitrate: Especially beneficial for African-American patients or those intolerant to ACEIs/ARBs.
Surgical and Device-Based Therapies
For patients who remain symptomatic despite optimal medical treatment, advanced interventions may be required:
- Cardiac resynchronization therapy (CRT): Restores coordinated ventricular contraction.
- Implantable cardioverter-defibrillator (ICD): Prevents sudden cardiac death from arrhythmia.
- Left ventricular assist device (LVAD): Provides mechanical circulatory support in end-stage cases.
- Heart transplantation: Considered the definitive treatment for patients with refractory, end-stage heart failure.
Heart failure management is lifelong and dynamic. Success depends on a multidisciplinary approach that combines medication, lifestyle optimization, patient education, and regular medical follow-up.
Lifestyle and Prevention of Heart Failure
Managing heart failure effectively requires more than medication—it also depends heavily on adopting a heart-healthy lifestyle. Small daily habits can make a significant difference in slowing disease progression, improving quality of life, and even preventing heart failure from developing in the first place.
Healthy Lifestyle Habits to Slow Heart Failure Progression
1. Follow Your Doctor’s Instructions
Strictly adhere to your prescribed treatment plan, including taking medications as directed and attending all follow-up appointments. Regular medical supervision helps track your heart function and adjust treatment as your condition changes.
2. Maintain a Positive and Active Lifestyle
Emotional health has a strong influence on physical health.
- Manage stress through relaxation techniques such as yoga, deep breathing, or meditation.
- Stay socially connected—talk to friends, family, or support groups about your feelings.
- Engage in activities you enjoy—reading, gardening, caring for pets, or listening to music can enhance mental well-being.
A positive mindset encourages adherence to treatment and improves recovery outcomes.
3. Gentle and Regular Exercise
Light-to-moderate physical activity helps strengthen your heart and improve circulation. Activities like walking, cycling, or swimming for 20–30 minutes most days of the week are beneficial.
Avoid overexertion, and consult your doctor before starting or changing an exercise routine—especially during periods of symptom flare-up.
4. Eliminate Unhealthy Habits
Quit smoking completely: Smoking accelerates atherosclerosis, increases blood pressure, and deprives tissues of oxygen.
Limit or avoid alcohol: Alcohol weakens the heart muscle, especially in people with alcoholic cardiomyopathy.
Maintain a healthy weight: Obesity increases cardiac workload and contributes to hypertension and diabetes.
Get adequate sleep: Poor sleep can worsen blood pressure and heart rhythm control.
5. Regular Medical Checkups
Schedule periodic health evaluations to monitor your condition and detect any early signs of deterioration. Early medical intervention can prevent complications and hospitalizations.
6. Rehabilitation and Physical Therapy
In patients recovering from cardiac events or stroke, cardiac rehabilitation and physical therapy play a vital role in restoring mobility, improving exercise tolerance, and enhancing long-term outcomes.
Nutrition for Heart Health
Diet plays a central role in managing and preventing heart failure.
- Reduce sodium intake:
Aim for less than 2 grams of sodium per day in moderate to severe heart failure to prevent fluid retention. Avoid processed and canned foods high in salt. - Eat a balanced diet rich in fiber and vitamins:
Include fresh vegetables, fruits, whole grains, and lean proteins (such as fish, chicken, tofu, or legumes). - Limit saturated fats and trans fats:
Replace them with healthy fats from olive oil, avocado, or nuts. - Control portion sizes:
Overeating increases blood volume and cardiac workload. - Stay hydrated appropriately:
In severe heart failure, your doctor may recommend fluid restriction to prevent fluid overload.
A heart-healthy diet supports optimal blood pressure, cholesterol, and weight—all key factors in preventing further cardiac strain.
Effective Prevention of Heart Failure
Primary Prevention (Preventing the Onset of Heart Failure)
The best strategy is to manage or eliminate risk factors before heart damage occurs:
- Control high blood pressure through medication, diet, and exercise.
- Manage diabetes with lifestyle modification and glucose-lowering therapy.
- Treat high cholesterol and maintain healthy lipid levels.
- Adopt a balanced, low-sodium diet and maintain a normal body weight.
- Avoid tobacco and excessive alcohol consumption.
Secondary Prevention (Preventing Worsening of Established Heart Failure)
For those already diagnosed with heart failure:
- Strict adherence to medical treatment to prevent exacerbations.
- Monitor symptoms daily: Sudden weight gain or increased swelling may indicate fluid buildup.
- Adjust medications promptly under medical supervision when symptoms worsen.
- Stay physically active within tolerance limits.
- Address comorbidities: Proper management of anemia, thyroid disorders, or kidney disease improves outcomes.
Early recognition and continuous care are the keys to stabilizing heart failure and improving survival.

