Atherosclerosis: What It Is, Symptoms, Causes, and Treatment
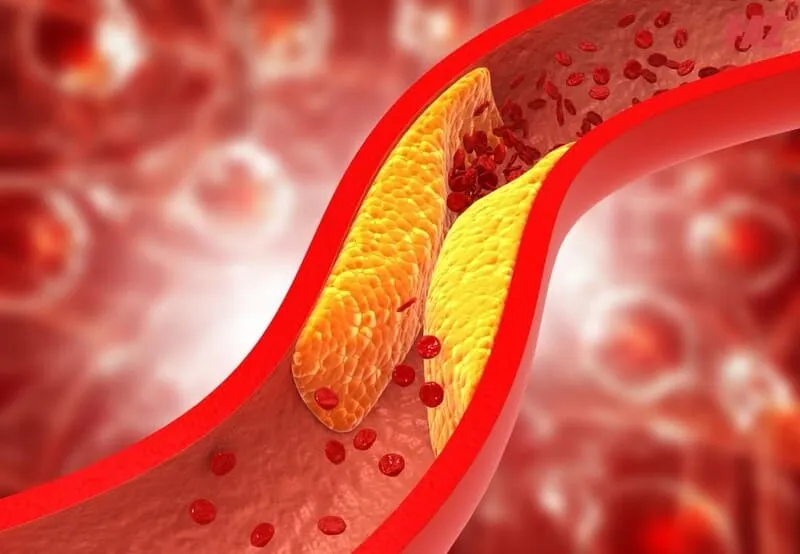
Atherosclerosis occurs when fatty deposits known as plaques build up along the inner walls of arteries, narrowing them and restricting blood flow to vital organs and tissues. Over time, this process can lead to serious cardiovascular complications, such as heart attacks, strokes, or peripheral artery disease.
These plaques are formed from a combination of fatty substances, cholesterol, smooth muscle cells, and fibrous tissue that accumulate within the arterial wall. As they grow, they trigger local inflammation and cellular responses that further damage the arteries, creating a cycle that eventually leads to blockage or vascular obstruction.
Maintaining a healthy lifestyle, engaging in regular physical activity, and following a heart-friendly diet are key strategies for preventing the onset or progression of atherosclerosis.
Overview of Atherosclerosis
What Is Atherosclerosis?
Atherosclerosis is a chronic condition characterized by the buildup of fats, cholesterol, and other cellular components inside the arterial walls. This accumulation—known as plaque—causes arteries to stiffen and narrow, reducing oxygen-rich blood flow to vital parts of the body.
In some cases, plaques may rupture or break open, triggering the formation of a blood clot (thrombus). This clot can suddenly block blood flow, resulting in life-threatening events such as stroke or myocardial infarction (heart attack).
At the cellular level, atherosclerosis begins when the endothelium (the inner lining of arteries) is damaged. Once injured, it can no longer produce enough prostacyclin, a substance that normally protects against platelet aggregation and vessel constriction.
Platelets then gather at the damaged site and release growth factors, stimulating smooth muscle cells to migrate and proliferate in the arterial wall. Meanwhile, macrophages—derived from circulating monocytes—engulf LDL cholesterol particles, turning into foam cells. These foam cells cluster to form fatty streaks, which eventually evolve into mature plaques.
When the fibrous cap of a plaque ruptures, it exposes its inner contents to the bloodstream, activating the coagulation cascade. The resulting clot can obstruct downstream blood flow, causing conditions such as:
- Acute myocardial infarction (heart attack) when the coronary arteries are blocked
- Ischemic stroke when the cerebral arteries are affected
- Peripheral gangrene when blood flow to the lower limbs is cut off
Atherosclerosis typically affects large and medium-sized arteries, including the coronary arteries, carotid arteries, cerebral arteries, aorta, and peripheral arteries of the limbs.
Symptoms of Atherosclerosis
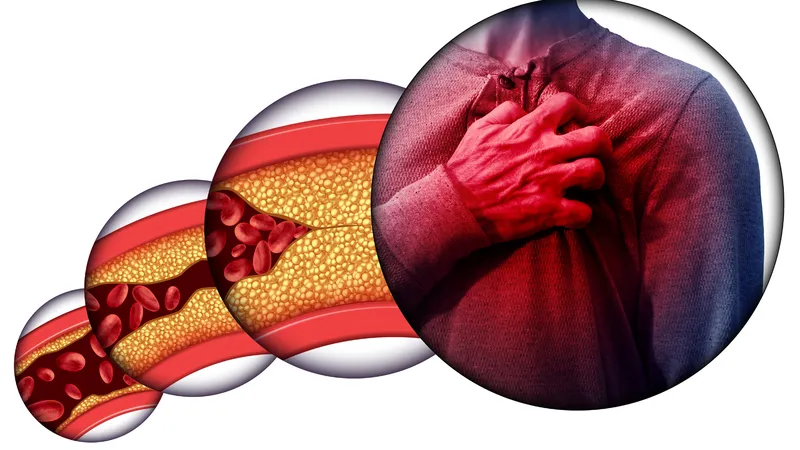
You may not experience any symptoms until an artery becomes severely narrowed or completely blocked, leading to conditions like a heart attack or stroke. Depending on which arteries are affected, symptoms can vary:
Coronary artery involvement: chest pain (angina), irregular heartbeat, shortness of breath, fatigue, nausea, vomiting, or sweating
Cerebral artery involvement: numbness or weakness in the arms or legs, confusion, cognitive decline, facial paralysis, balance problems, severe headache, or blurred vision
Peripheral artery involvement: leg pain while walking (claudication), limb numbness, or weakness in the affected area
Slow-healing wounds: due to reduced blood supply
Visible fatty streaks: may represent early-stage arterial damage
Possible Complications
If left untreated, atherosclerosis can lead to several serious conditions, including:
- Coronary artery disease (CAD)
- Carotid artery disease
- Peripheral artery disease (PAD)
- Aneurysm formation
- Chronic kidney disease
Atherosclerosis often progresses silently until it causes sudden complications such as heart attack or stroke, both of which can lead to permanent disability or death.
Complication Risks by Organ System
Brain: Narrowing of arteries supplying the brain may result in a transient ischemic attack (TIA) or a stroke. In some cases, plaques formed elsewhere (e.g., in the coronary arteries) can rupture, sending clots to the brain and causing an ischemic stroke. Chronic reduction in cerebral blood flow can also contribute to vascular dementia, impairing memory and cognition.
Heart: Coronary artery atherosclerosis can lead to aortic aneurysm, arrhythmia, angina, heart failure, or acute myocardial infarction.
Kidneys and other organs: Plaque buildup in the renal arteries can cause chronic kidney disease or renal failure, potentially requiring dialysis or kidney transplantation. Atherosclerosis affecting the mesenteric arteries can cause intestinal ischemia, leading to bowel necrosis or life-threatening infection.
Limbs: Peripheral artery disease (PAD) causes poor blood circulation in the arms or legs, leading to ulcers, infections, or gangrene. Acute limb ischemia is a medical emergency with high risks of amputation or death.
When to See a Doctor
If you experience chest pain, shortness of breath, numbness, or unexplained limb pain, seek medical attention as soon as possible. Early diagnosis and treatment can help prevent severe complications and improve long-term outcomes.
Causes of Atherosclerosis
What Causes Atherosclerosis?
Atherosclerosis develops gradually over time due to a combination of biological, lifestyle, and metabolic factors that damage the arterial walls. The most common causes include:
High cholesterol levels: Elevated LDL (“bad”) cholesterol promotes the accumulation of fatty deposits in the arterial walls, forming lipid plaques that narrow blood vessels.
High blood pressure (hypertension): Chronic hypertension triggers inflammation within blood vessels through angiotensin II–mediated pathways. This molecule stimulates endothelial cells, smooth muscle cells, and macrophages to produce pro-inflammatory cytokines, reactive oxygen species, and growth factors that accelerate arterial thickening and fibrosis.
Inflammatory conditions: Chronic inflammatory diseases such as rheumatoid arthritis, lupus, psoriasis, or inflammatory bowel disease (IBD) can damage blood vessels and contribute to plaque buildup.
Diabetes mellitus: Elevated blood glucose generates free radicals that injure endothelial cells, promote lipid oxidation, and speed up the progression of atherosclerosis.
Smoking: Nicotine and other toxic substances in tobacco smoke impair endothelial function, reduce oxygen delivery, and significantly increase plaque formation.
Chronic kidney disease: Reduced kidney function contributes to oxidative stress, systemic inflammation, and abnormal lipid metabolism, all of which promote arterial hardening.
Although these mechanisms are well understood, the exact root cause of atherosclerosis remains multifactorial and complex. Currently, there is no permanent cure, but treatment and lifestyle modification can slow disease progression, prevent complications, and protect cardiovascular health.
Who Is at Risk of Atherosclerosis?
Atherosclerosis can affect anyone, but certain groups are more likely to develop it:
- People with underlying metabolic disorders, such as high cholesterol, hypertension, obesity, or diabetes
- Individuals with a sedentary lifestyle or lack of regular exercise
- Smokers and those who consume excessive alcohol
- People under chronic stress, anxiety, or depression
- Adults aged 55 and older
- Individuals with a family history of atherosclerosis or early heart disease
Risk Factors That Increase the Likelihood of Atherosclerosis
Certain factors further raise the risk or accelerate the progression of atherosclerosis, including:
- Advancing age: The risk increases as arteries naturally lose elasticity over time.
- Family history: A family history of premature heart disease or atherosclerosis increases genetic susceptibility.
- Obesity and abdominal fat: Excess body weight promotes high blood pressure, insulin resistance, and lipid imbalance.
- Unhealthy diet: Diets high in saturated fats, processed foods, and alcohol—and low in fruits, vegetables, and whole grains—contribute to arterial damage.
- Lack of physical activity: Sedentary habits reduce circulation and impair cardiovascular function.
- Chronic stress: Long-term stress triggers hormonal changes that elevate blood pressure, blood sugar, and cholesterol levels.

Diagnosis and Treatment of Atherosclerosis
How Is Atherosclerosis Diagnosed?
Diagnosing atherosclerosis requires a combination of clinical evaluation, laboratory tests, and imaging studies. Physicians typically begin by reviewing your medical history, family history, and current symptoms, then perform targeted tests based on the suspected location of arterial narrowing or blockage.
Common diagnostic methods include:
Blood tests: Measure levels of total cholesterol, LDL and HDL cholesterol, triglycerides, fasting blood glucose, and C-reactive protein (CRP)—a marker of inflammation.
Cerebral atherosclerosis: Transcranial Doppler ultrasound, cerebral angiography, CT scan, or brain MRI to detect narrowed or blocked cerebral arteries.
Ocular atherosclerosis: Direct or indirect ophthalmoscopy (fundoscopy) to observe the retinal arteries for signs of reduced blood flow.
Carotid artery disease: Carotid Doppler ultrasound or CT angiography with contrast to assess plaque buildup and stenosis.
Renal artery atherosclerosis: Doppler ultrasound or contrast-enhanced renal angiography to evaluate blood flow to the kidneys.
Coronary artery disease: Electrocardiogram (ECG), stress testing, Holter monitoring, echocardiography, or coronary angiography to detect ischemic changes.
Aortic atherosclerosis: X-ray imaging with contrast, MRI, or vascular ultrasound to visualize thickening or aneurysm formation in the aorta.
Peripheral artery disease (PAD): Doppler ultrasound of the lower extremities, angiography, or ankle-brachial index (ABI) testing to compare blood pressure between the arm and ankle.
These tests help determine the extent, location, and severity of arterial damage, guiding the most effective treatment plan for each individual.
Effective Treatment Options for Atherosclerosis
Treatment depends on the severity of the disease, location of the blockage, and overall health status of the patient. The primary goal is to slow plaque progression, improve blood flow, and prevent life-threatening complications like heart attack or stroke.
1. Lifestyle Modifications
Lifestyle changes are the foundation of atherosclerosis management and can significantly improve cardiovascular health:
- Reduce dietary fat intake, especially saturated and trans fats.
- Increase consumption of fruits, vegetables, whole grains, and lean proteins.
- Engage in regular physical activity, such as 30 minutes of moderate exercise most days of the week.
- Quit smoking and limit alcohol consumption.
- Manage stress through relaxation techniques, meditation, or therapy.
2. Medications
Doctors may prescribe medications to control risk factors and prevent blood clots:
Cholesterol-lowering drugs:
- Statins (e.g., atorvastatin, rosuvastatin) to reduce LDL cholesterol and plaque buildup.
- Fibrates and bile acid sequestrants for patients with high triglycerides or statin intolerance.
Antihypertensive agents: ACE inhibitors (e.g., enalapril), angiotensin II receptor blockers (ARBs) (e.g., losartan), and beta-blockers (e.g., metoprolol) to lower blood pressure and reduce heart strain.
Antiplatelet and anticoagulant drugs:
- Aspirin or clopidogrel to prevent platelet aggregation and reduce clot formation.
- Warfarin or heparin may be used in specific cases to prevent thrombosis.
3. Surgical and Interventional Procedures
In advanced cases or when medical therapy alone is insufficient, interventional or surgical treatments may be required to restore blood flow:
- Coronary artery bypass grafting (CABG): Redirects blood flow around blocked coronary arteries.
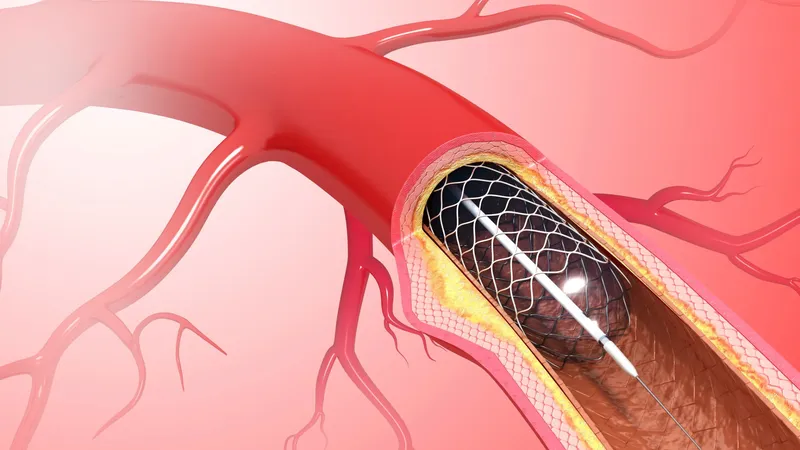
- Angioplasty and stent placement: Opens narrowed arteries and keeps them patent using a stent.
- Thrombolytic therapy: Dissolves blood clots that obstruct arteries (used in emergency settings).
- Endarterectomy: Removes plaque buildup from the inner walls of major arteries, such as the carotid artery.
- Aneurysm or vessel resection: Surgical removal or repair of severely damaged or aneurysmal blood vessels.
- Amputation: In severe PAD cases with gangrene, limb amputation may be necessary to prevent systemic infection.
Summary
Atherosclerosis is a progressive but manageable disease. Early detection, combined with a heart-healthy lifestyle and appropriate medical treatment, can dramatically reduce the risk of complications. Regular follow-ups and adherence to prescribed therapy are essential to protect long-term cardiovascular health.
Lifestyle and Prevention of Atherosclerosis
Developing healthy daily habits can significantly slow the progression of atherosclerosis and improve overall cardiovascular health.
Recommended Lifestyle Habits
Follow your doctor’s treatment plan. Adhere strictly to prescribed medications and monitoring schedules.
Manage related conditions such as high cholesterol, hypertension, obesity, and diabetes effectively.
Exercise regularly. Aim for at least 75 minutes of vigorous activity per week or 150 minutes of moderate-intensity exercise to strengthen the heart and promote blood circulation.
Quit smoking. Stopping tobacco use helps improve vascular function and slows plaque buildup.
Maintain a healthy weight. Achieving and keeping a balanced body mass index (BMI) reduces cardiovascular strain.
Adopt a positive lifestyle. Limit stress through relaxation, mindfulness, or engaging hobbies.
Monitor your health regularly. Check blood pressure, cholesterol, and blood sugar levels periodically.
Stay in touch with your doctor if you notice any unusual symptoms during treatment.
Maintain a positive attitude. Mental well-being plays an important role in managing chronic cardiovascular diseases.
Dietary Recommendations
A heart-healthy diet is a cornerstone of preventing and managing atherosclerosis.
Eat more fruits, vegetables, whole grains, legumes, low-fat dairy products, poultry, and fish (preferably without skin).
Use healthy fats such as olive oil, avocados, and nuts instead of saturated and trans fats.
Limit sugar intake. Avoid sugary beverages and sweets. According to the American Heart Association (AHA), women should consume no more than 100 calories from added sugar per day, and men no more than 150 calories.
Reduce sodium intake. Aim for less than 2,300 mg of sodium per day; ideally, less than 1,500 mg is best for heart health.
Avoid unhealthy fats and processed foods, including fried, baked, and fast foods high in trans fats or preservatives.

Effective Prevention Strategies
To effectively prevent atherosclerosis, consider the following recommendations:
Maintain a healthy lifestyle. Manage stress, sleep at least 7–8 hours per night, and engage in regular physical activity.
Avoid harmful habits such as smoking, secondhand smoke exposure, and excessive alcohol consumption.
Follow a balanced diet low in saturated fat, cholesterol, and sodium.
Treat and regularly monitor chronic diseases such as heart disease, diabetes, and kidney disorders.
