Arrhythmia: Symptoms, Causes, and Treatment
Understanding Arrhythmia
Arrhythmia is a cardiac condition that presents with an irregular heartbeat, which may be abnormally fast (tachycardia) or slow (bradycardia). It can cause a fluttering, racing, or irregular sensation in the chest, noticeable during daily activities or even at rest.
Most rapid arrhythmias are caused by reentry mechanisms, while others may result from increased automaticity or abnormal electrical activity within the heart.
There are various types of arrhythmias, depending on which part of the heart is affected and whether the rhythm becomes slow, fast, or irregular. Arrhythmias can originate in the atria (upper chambers) or the ventricles (lower chambers) of the heart.
Symptoms of Arrhythmia
Common signs and symptoms
Some arrhythmias may cause no noticeable symptoms. However, you should seek medical attention if you experience any of the following:
- Palpitations (feeling of skipped, fluttering, or pounding heartbeats)
- Dizziness or lightheadedness
- Shortness of breath
- Chest pain or discomfort
- Fainting (syncope) or near-fainting spells
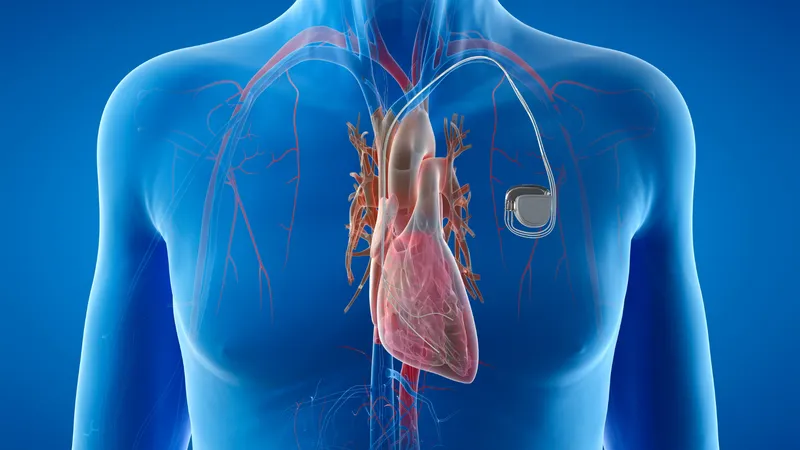
Health Impacts of Arrhythmia
If left untreated, arrhythmia can lead to severe complications, including:
Cardiac arrest: Irregular heart rhythms can cause the heart to stop suddenly.
Heart failure: Repeated arrhythmias can weaken the heart muscle, leading to an inability to pump sufficient blood to meet the body’s needs.
Cognitive and memory problems: Reduced blood flow to the brain due to arrhythmia may contribute to Alzheimer’s disease and vascular dementia.
Stroke: Blood may pool in the upper chambers of the heart, forming clots that can travel to the brain and cause a stroke.
Sudden Infant Death Syndrome (SIDS): Infants with inherited arrhythmias may have a higher risk of SIDS.
Worsening irregular heartbeat: Some arrhythmias may progress or trigger other unstable rhythms over time.
When to See a Doctor
Keep track of when your symptoms occur, how often they happen, and what you are doing at the time. Note whether the symptoms change over time.
Seek immediate medical attention if you experience severe symptoms such as shortness of breath, chest pain, or fainting.
Early diagnosis and timely treatment play a vital role in reducing complications and improving heart health.
Causes and Risk Factors of Arrhythmia
Causes of Arrhythmia
Arrhythmia can develop from various causes — including structural or functional heart abnormalities, as well as disorders in other organs that affect the heart’s rhythm.
Common causes of irregular heartbeat include:
Sinoatrial node dysfunction: The sinoatrial (SA) node is the heart’s natural pacemaker. When its function becomes impaired or abnormal, the heartbeat can become irregular.
Ectopic pacemaker activity: Abnormal electrical foci in the heart can disrupt the normal rhythm and cause irregular beats.
Abnormal conduction pathways: Irregular or extra conduction pathways in the heart may lead to disordered electrical signaling.
Damage to the conduction system: Injury or blockage within the heart’s normal conduction system (heart block) can result in arrhythmia.
Heart muscle damage: Conditions that weaken or scar the myocardium can interfere with normal electrical impulses and trigger arrhythmias.
Electrolyte imbalances: Abnormal levels of potassium, sodium, calcium, or magnesium — often due to kidney disease — can destabilize the heart’s rhythm.
Medication side effects or toxins: Certain drugs or toxic substances can provoke arrhythmias as a side effect.
Other medical conditions: Disorders such as hyperthyroidism (overactive thyroid) can accelerate the heartbeat and lead to rhythm disturbances.
Irregular heartbeats can occur temporarily, lasting only a few minutes, or persist for hours, months, or even years — sometimes without obvious warning signs.

Who Is at Risk of Developing Arrhythmia?
As we age, natural changes in heart tissue, such as scarring and the effects of chronic diseases, can increase the likelihood of arrhythmias.
Older adults are more likely to have medical conditions such as high blood pressure, heart failure, diabetes, or thyroid disease, all of which can contribute to irregular heart rhythms.
In contrast, arrhythmias caused by congenital heart defects or genetic syndromes are more common among infants and young people.
Some arrhythmias may also be inherited, meaning you’re at higher risk if your parents or close relatives have irregular heart rhythms.
Even certain antibiotics or over-the-counter allergy and cold medications can trigger arrhythmias in sensitive individuals.
Risk Factors for Arrhythmia
Several factors can increase the risk of developing arrhythmia:
Age: Older adults are at higher risk due to underlying heart and metabolic conditions.
Genetics: Family history of arrhythmia or sudden cardiac death increases susceptibility.
Lifestyle factors:
- Use of stimulants such as cocaine or amphetamines.
- Excessive alcohol intake (more than 2 drinks per day for men or 1 for women).
Medications:
Some prescription drugs used for high blood pressure or mental health disorders, as well as certain antibiotics and allergy medicines, can cause arrhythmias. Always discuss potential risks with your doctor.

Underlying health conditions:
- Cardiovascular diseases such as cardiomyopathy, congenital heart defects, myocardial infarction, or myocarditis.
- Kidney disease.
- Chronic lung diseases like COPD.
- Obesity.
- Sleep apnea, which limits oxygen intake and stresses the heart.
- Thyroid disorders.
- Viral infections such as influenza or COVID-19.
Surgery: Arrhythmia risk increases in the days or weeks following surgery involving the heart, lungs, or throat.
Diagnosis and Treatment of Arrhythmia
Diagnostic Methods and Tests for Arrhythmia
Sometimes, especially if you don’t experience any noticeable symptoms of an irregular heartbeat, your doctor may detect arrhythmia during a routine checkup.
To diagnose the condition, your doctor will ask about your symptoms, lifestyle habits, and risk factors for arrhythmia. The physical examination may include:
- Checking for swelling in your legs or feet, which could indicate an enlarged heart or heart failure.
- Measuring your pulse.
- Listening to your heart rate and rhythm.
- Detecting any abnormal heart sounds.
- Looking for signs of other medical conditions, such as thyroid disorders, that may cause arrhythmia.
Diagnostic tests may include:
- Electrocardiogram (ECG or EKG): The most common test used to diagnose arrhythmias.
- Blood tests: Used to measure the levels of certain substances in your blood, such as potassium, other electrolytes, and thyroid hormones.

Effective Treatments for Arrhythmia
Treating the Underlying Cause
Treatment focuses on addressing the underlying cause of arrhythmia. If necessary, direct anti-arrhythmic therapy may be used, including anti-arrhythmic medications, defibrillation, implantable cardioverter-defibrillators (ICDs), pacemakers (or cardiac resynchronization therapy), catheter ablation, surgery, or a combination of these options.
Patients with irregular heartbeats that have caused or may cause hemodynamic instability should avoid driving until their response to treatment is evaluated.
Surgical Treatment for Arrhythmia
Surgery to treat tachyarrhythmias (rapid heart rhythms) has become less common as minimally invasive ablation techniques have advanced. However, surgery is still indicated when the arrhythmia cannot be managed with ablation, or when another cardiac procedure is required — for example, in patients with atrial fibrillation who need valve repair or replacement, or in those with ventricular tachycardia requiring coronary revascularization or left ventricular aneurysm resection.
Medications for Managing Rapid Heart Rhythms
Common medications used to control fast or irregular heartbeats include:
Adenosine: May cause temporary chest discomfort, flushing, shortness of breath, or atrial fibrillation; typically administered by emergency medical services or in an emergency room setting.
Beta-blockers: May cause fatigue, digestive problems, sleep disturbances, sexual dysfunction, and can worsen certain conduction disorders.
Calcium channel blockers: Can lead to digestive issues, swelling in the feet, or low blood pressure.
Digoxin: Used mainly for atrial fibrillation; may cause nausea, vomiting, or diarrhea.
Potassium channel blockers: Can cause low blood pressure, thyroid problems, lung conditions, or other irregular heart rhythms.
Sodium channel blockers: May increase the risk of sudden cardiac arrest in patients with structural heart disease.
Lifestyle & Prevention of Arrhythmia
Healthy Habits to Help Manage Arrhythmia
Lifestyle Recommendations:
Follow your doctor’s instructions carefully regarding medication and treatment plans.
Maintain a positive and active lifestyle while minimizing stress.
Contact your doctor immediately if you notice any unusual symptoms or changes in your condition during treatment.
Schedule regular medical checkups to monitor your heart health, assess disease progression, and allow your doctor to adjust treatment if necessary.
Stay optimistic. Mental health plays a vital role in recovery. Talk to trusted friends or family members, spend time with pets, read, or engage in activities that bring you comfort and relaxation.
Avoid contact sports that could dislodge your pacemaker or implanted defibrillator.
Refrain from high-intensity activities such as swimming or diving if advised by your doctor.
Modify loud or startling sounds like alarm tones or ringtones to prevent sudden stress responses.
Dietary Guidelines
Limit or avoid caffeine found in coffee, tea, sodas, and chocolate, as it may trigger or worsen arrhythmia in some individuals.
Effective Ways to Prevent Arrhythmia
If you are at higher risk of developing an arrhythmia, your doctor may recommend specific preventive strategies, such as:
Avoid known triggers that may cause irregular heart rhythms.
Manage underlying health conditions — such as high blood pressure, diabetes, or thyroid disorders — that can contribute to arrhythmia.
Adopt heart-healthy lifestyle changes, including:
- Eating a balanced diet rich in fruits, vegetables, and whole grains.
- Engaging in regular physical activity suitable for your condition.
- Maintaining a healthy weight.
- Quitting smoking.
- Managing stress through relaxation techniques or counseling.
Consult your doctor before heart surgery or procedures to ensure proper management of electrolyte levels and medications during and after the operation to prevent rhythm disturbances.
