Stage 2 Uterine Cancer: Symptoms, Causes, Diagnosis and Treatment
What Is Stage 2 Uterine Cancer?
There are two main types of uterine cancer:
- Endometrial cancer – the most common form, starting in the inner lining of the uterus (endometrium).
- Uterine sarcoma – a rare type that begins in the muscle layer of the uterus or surrounding tissues.
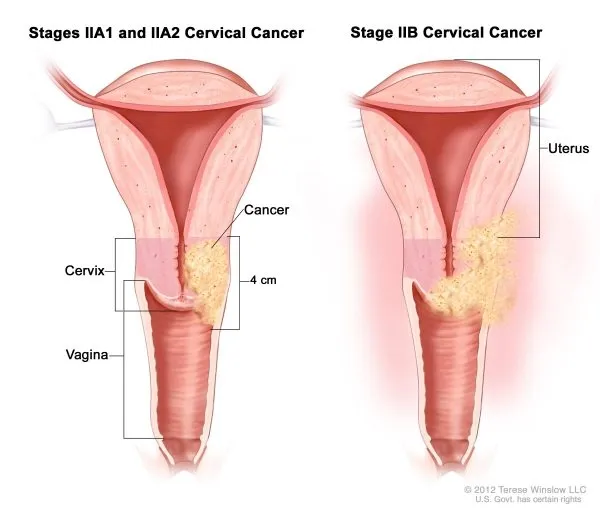
Understanding Stage 2 Uterine Cancer
Doctors usually stage uterine cancer using two similar systems:
- The International Federation of Gynecology and Obstetrics (FIGO) system
- The TNM classification from the American Joint Committee on Cancer (AJCC)
Both systems evaluate three key factors:
- Tumor (T): The size of the main tumor and how deeply it has invaded surrounding tissues.
- Lymph nodes (N): Whether cancer has spread to nearby lymph nodes. Lymph nodes are small bean-shaped glands throughout the body and are part of the immune system.
- Metastasis (M): Whether cancer has spread to distant lymph nodes or other organs.
Uterine cancer has four stages (I–IV). Lower stages mean the cancer is still localized. By stage IV, cancer cells have spread to distant parts of the body.
Stage 2 uterine cancer means the cancer has spread from the uterus into the cervical tissue but has not yet extended outside the uterus.
Symptoms of Stage 2 Uterine Cancer
The most common symptom of stage 2 uterine cancer is abnormal vaginal bleeding, such as spotting or bleeding not related to your menstrual cycle. You may also notice watery or blood-streaked vaginal discharge. In postmenopausal women, any vaginal bleeding should be considered a warning sign.
When to See a Doctor
See your doctor if you experience any abnormal vaginal bleeding or spotting unrelated to your period. If you have a hereditary risk for endometrial cancer, you should have yearly checkups and may need an annual endometrial biopsy starting at age 35.
Causes of Stage 2 Uterine Cancer
Researchers do not yet know the exact cause of uterine cancer. Something triggers changes in the DNA of cells within the uterus. These genetic mutations cause cells to grow and multiply uncontrollably, forming a mass known as a tumor.
Several risk factors can increase the likelihood of developing uterine cancer. If you are at high risk, talk to your doctor about regular checkups and preventive screening.
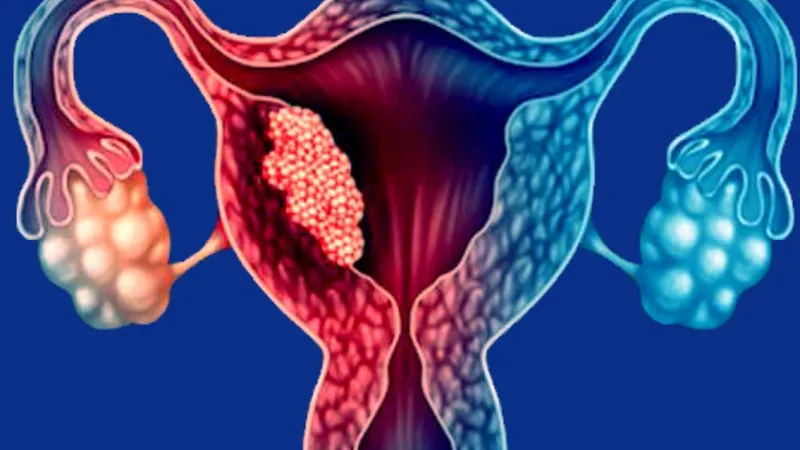
Risk Factors for Stage 2 Uterine Cancer
Who Is at Risk?
In the United States, endometrial cancer is the most common cancer of the female reproductive system. It occurs mainly after menopause. About 3% of women will be diagnosed with uterine cancer at some point in their lives, with roughly 65,000 new cases diagnosed each year.
Major Risk Factors
Many risk factors for uterine cancer are linked to the balance between estrogen and progesterone. These include obesity, polycystic ovary syndrome (PCOS), or taking estrogen without progesterone. A hereditary condition called Lynch syndrome is another non-hormonal risk factor.
Key factors include:
Age, Lifestyle and Family History
- Age: Risk increases as you get older. Most uterine cancers occur after age 50.
- High-fat diet: Diets rich in animal fat may raise the risk of certain cancers, including uterine cancer. High-fat foods also tend to be calorie-dense, contributing to obesity.
- Family history: Some people have inherited conditions that raise their cancer risk. Those with Lynch syndrome (also called hereditary nonpolyposis colorectal cancer, HNPCC) have a higher risk of endometrial and other cancers.
Other Medical Conditions
- Diabetes: Often associated with obesity, diabetes may independently increase uterine cancer risk.
- Obesity: Fat tissue can convert other hormones into estrogen, raising estrogen levels. The more body fat, the stronger this effect.
- Ovarian conditions: Certain ovarian tumors may increase estrogen levels while lowering progesterone levels, altering hormone balance and increasing risk.
Gynecologic History
- Early menarche: Starting periods before age 12 increases lifetime estrogen exposure.
- Late menopause: Menopause after age 50 also prolongs estrogen exposure.
- Long reproductive span: The total number of years with menstrual cycles may matter more than age.
- Never having been pregnant: Nulliparous women have a higher risk.
Previous Treatments
- Prior pelvic radiation therapy: Used to treat other cancers, it can alter DNA in uterine cells, increasing the chance of a second cancer.
- Estrogen replacement therapy (ERT): Some women receive estrogen to relieve menopausal symptoms, which can increase risk if not balanced with progesterone.
- Tamoxifen use: This breast cancer drug acts like estrogen in the uterus and may raise uterine cancer risk.

Diagnosis and Treatment of Stage 2 Uterine Cancer
Diagnostic Tests and Examinations for Stage 2 Uterine Cancer
Your doctor may recommend several tests to check whether you have uterine cancer. The types of tests will depend on your symptoms and may include:
- Transvaginal ultrasound
- Endometrial biopsy
- Blood tests
If you are diagnosed with uterine cancer, you will usually undergo additional tests to determine how far the cancer has spread, such as:
- CT scan (computed tomography)
- MRI (magnetic resonance imaging)
- PET scan (positron emission tomography)
- Colonoscopy
- Chest X-ray
- Genetic testing to check for a rare inherited condition called Lynch syndrome
These tests help doctors determine the stage of the uterine cancer.
Treatment for Stage 2 Uterine Cancer
In most cases, stage 2 uterine cancer is treated with radical hysterectomy, which involves removal of the uterus, the tissues next to it, and the upper part of the vagina. The surgeon may also remove your fallopian tubes and ovaries.
You may also receive radiation therapy as part of your treatment plan.
Lifestyle Habits and Prevention of Stage 2 Uterine Cancer
Lifestyle Habits to Help Slow the Progression of Stage 2 Uterine Cancer
Daily habits:
Here are some general lifestyle suggestions for people with stage 2 uterine cancer:
Physical activity and exercise:
- Engage in gentle exercises such as walking, yoga, or swimming to maintain health and a positive mindset.
- Consult your doctor before starting any new exercise program.
Maintain a positive outlook:
- Seek support from family, friends, support groups, or mental health counseling.
- Practice stress-reduction techniques such as meditation, yoga, or relaxing activities.
Regular health check-ups:
- Attend regular medical check-ups and follow your doctor’s treatment plan.
- Discuss any new or unusual symptoms with your doctor.
Limit exposure to harmful substances:
- Avoid smoking, alcohol, and environmental pollutants.
Self-care:
- Learn to take care of yourself and listen to your body.
- Ensure adequate sleep and rest.
Nutrition
A healthy diet plays an important role in supporting treatment and improving quality of life for people with stage 2 uterine cancer. Here are some suggestions:
- High-fiber foods: Eat plenty of fresh vegetables and fruits to supply fiber for good digestion and to support treatment.
- Protein-rich foods: Include protein from sources such as poultry, fish, beans, nuts, dairy, and eggs to maintain muscle and overall health.
- Balanced carbohydrates: Choose whole grains and unsweetened cereals to maintain stable energy levels.
- Limit sugar and saturated fat: Reduce foods high in sugar and saturated fat to lower the risk of weight gain and improve heart health.
- Stay hydrated: Drink enough water daily to maintain health and help your body eliminate toxins.
- Avoid processed and fast foods: Limit processed foods and fast foods that are high in preservatives and unhealthy fats.
Prevention of Stage 2 Uterine Cancer
You cannot completely prevent uterine cancer. However, you can take steps to reduce your risk by:
- Managing diabetes well.
- Maintaining a healthy weight.
- Consulting your doctor if you use hormone therapy.