Non-Hodgkin Lymphoma: Symptoms, Causes, and What You Should Know
What Is Non-Hodgkin Lymphoma?
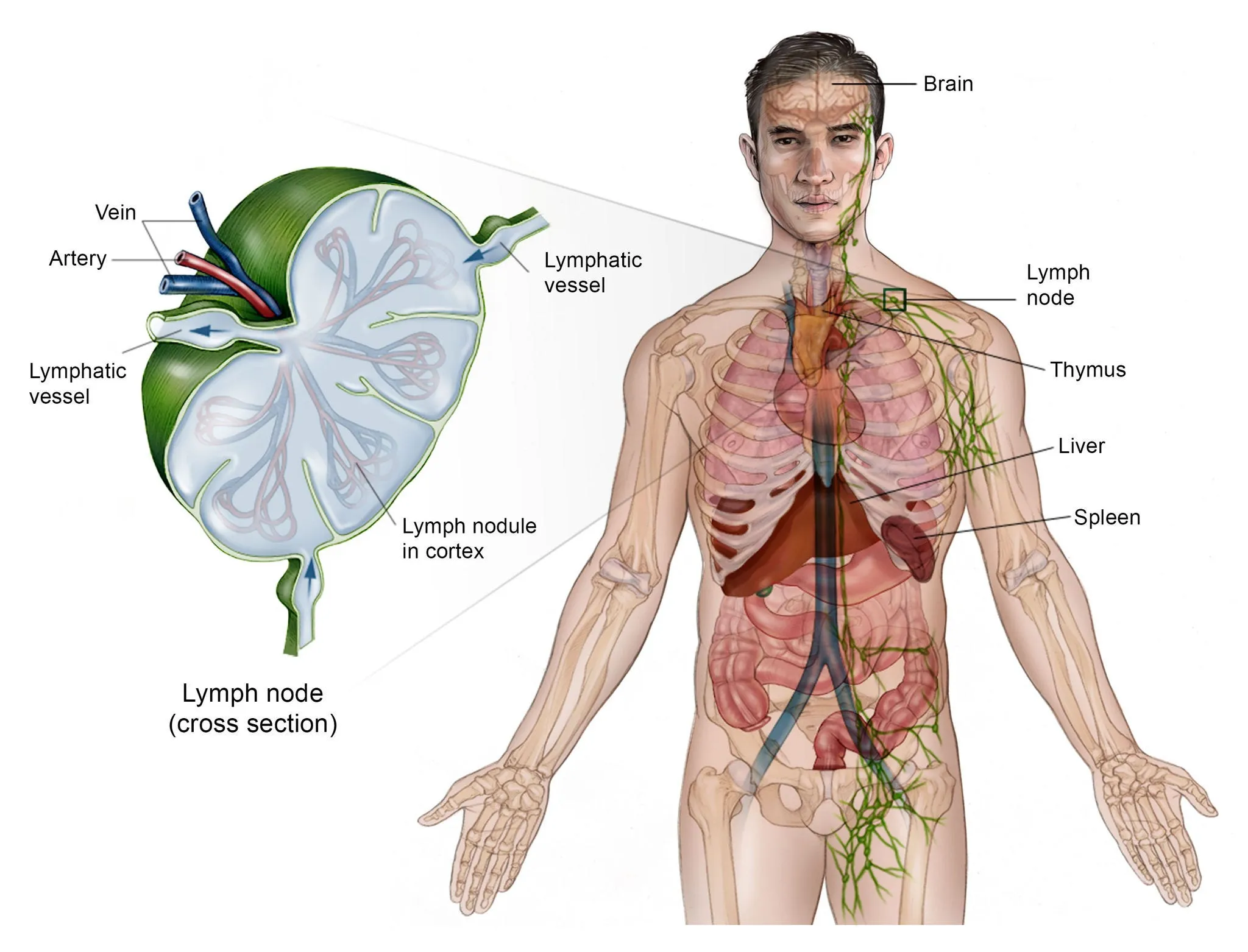
Non-Hodgkin lymphoma, sometimes called non-Hodgkin’s disease or simply NHL, refers to a group of cancers that affect the lymphatic system, which is part of the body’s immune defense.
Unlike Hodgkin lymphoma, which is marked by the presence of Reed-Sternberg cells, NHL includes more than 70 different subtypes. These cancers can start anywhere in the lymphatic system — such as the lymph nodes, spleen, bone marrow, or even extranodal tissues — and may spread to other parts of the body.
Types of Non-Hodgkin Lymphoma
NHL usually develops from one of two main types of lymphocytes:
- B-cell lymphoma: The most common form, arising from B lymphocytes that produce antibodies to fight infection.
- T-cell lymphoma: A rarer subtype, originating from T lymphocytes that directly destroy infected or cancerous cells.
Common Symptoms of Non-Hodgkin Lymphoma
Signs of NHL can vary depending on where the cancer develops, but the most common warning signs include:
- Swollen but painless lymph nodes (neck, armpit, or groin)
- Abdominal pain, swelling, or bloating
- Chest pain or pressure
- Unexplained fever
- Persistent fatigue and frequent headaches
- Night sweats (often drenching)
- Unexplained weight loss
- Shortness of breath or chronic cough
- Loss of appetite, nausea, or vomiting
- Constipation or digestive issues
- In rare cases: seizures
Tip: Because these symptoms can resemble common infections, persistent or unexplained signs should be checked by a healthcare provider.
Possible Complications of Non-Hodgkin Lymphoma
If not managed promptly, NHL can lead to serious, sometimes life-threatening complications. Early recognition and treatment are crucial. Potential complications include:
- Febrile neutropenia (low white blood cells with fever)
- Tumor lysis syndrome (TLS): A metabolic emergency caused by rapid tumor breakdown, leading to high uric acid, potassium, and kidney problems
- Spinal cord or brain compression
- Airway obstruction (especially in mediastinal lymphoma)
- Intestinal obstruction or intussusception
- Urinary tract obstruction
- Superior vena cava syndrome (blocked major vein return to the heart)
- Hypercalcemia (especially in adult T-cell lymphoma)
- Pericardial effusion or compression
- Blood clot disorders (venous thrombosis)
- Autoimmune complications such as hemolytic anemia or low platelet count

When Should You See a Doctor?
You should consult a doctor if you experience:
- Persistent swollen lymph nodes
- Unexplained fever, night sweats, or weight loss
- Prolonged fatigue or shortness of breath
While swollen lymph nodes can often be caused by infections (like strep throat), it is important to rule out more serious conditions such as non-Hodgkin lymphoma. Early diagnosis leads to more effective treatment and better outcomes.
Causes and Risk Factors of Non-Hodgkin Lymphoma
What Causes Non-Hodgkin Lymphoma?
In most cases, the exact cause of non-Hodgkin lymphoma (NHL) is unknown. The disease begins when the body produces too many abnormal lymphocytes (a type of white blood cell).
These changes are often linked to genetic mutations that alter how lymphocytes grow and divide. Unlike inherited genetic disorders, these are usually acquired mutations that develop over a person’s lifetime.
NHL can be associated with a wide range of triggers, including infections, environmental exposures, immune system disorders, and chronic inflammation.
Infectious Agents Linked to NHL
Certain infections have been shown to play a role in the development of different subtypes of non-Hodgkin lymphoma:
- Epstein–Barr virus (EBV): A DNA virus linked to several forms of NHL, including endemic Burkitt lymphoma.
- Human T-cell leukemia virus type 1 (HTLV-1): Associated with adult T-cell lymphoma through chronic antigen stimulation and cytokine dysregulation.
- Hepatitis C virus (HCV): Can cause abnormal B-cell proliferation, increasing the risk of splenic marginal zone lymphoma and diffuse large B-cell lymphoma.
- Human herpesvirus 8 (HHV-8): Connected with primary effusion lymphoma (PEL), a rare, aggressive form of B-cell NHL also linked to Kaposi sarcoma.
- Helicobacter pylori (H. pylori): A bacterial infection that raises the risk of gastric mucosa-associated lymphoid tissue (MALT) lymphoma.
Medications and Environmental Exposures
Some drugs and chemicals may also increase NHL risk:
- Medications such as phenytoin, digoxin, and TNF antagonists
- Organic solvents, pesticides, herbicides (phenoxy types), wood preservatives, dyes, and dust exposure
- Hair dyes and chemotherapy drugs
- Radiation exposure
Immune System Disorders
Disruptions in the immune system can play a significant role in lymphoma development:
- Inherited immune deficiencies: Conditions such as Wiskott–Aldrich syndrome and severe combined immunodeficiency (SCID).
- Acquired immunodeficiency: Immunosuppressive therapy after organ transplantation or in patients with autoimmune diseases.
- HIV/AIDS: Greatly increases the risk of primary central nervous system lymphoma.
- Autoimmune disorders: Conditions like Sjögren’s syndrome, rheumatoid arthritis, Hashimoto’s thyroiditis, and celiac disease are linked to higher NHL risk.
Who Is at Risk of Non-Hodgkin Lymphoma?
Anyone can develop NHL, but certain groups have a higher likelihood:
- People with weakened immune systems (such as transplant recipients on anti-rejection medications)
- Individuals with chronic infections like HIV, EBV, or H. pylori
- Older adults, particularly those over age 60
- Men, who statistically face a slightly higher risk than women
Additional Risk Factors for NHL
Several lifestyle and medical factors may increase susceptibility:
- Autoimmune diseases: Such as inflammatory bowel disease, rheumatoid arthritis, psoriasis, and other rheumatic conditions
- HIV/AIDS: Although NHL does not mean a person necessarily has HIV, those living with the virus face a much higher risk
- Helicobacter pylori infection: Known for causing stomach ulcers, repeated infections can raise NHL risk
- Viral exposure: Including EBV and HTLV-1
- Organ transplantation: Heart, lung, or kidney transplant recipients are more vulnerable due to long-term immunosuppression
- Radiation therapy from past treatments
- Pesticide exposure: Agricultural workers exposed to high levels of pesticides may face a slightly elevated risk
- Obesity
- Diets high in red meat and animal fat
Diagnosis and Treatment of Non-Hodgkin Lymphoma
How Is Non-Hodgkin Lymphoma Diagnosed?
Diagnosis of non-Hodgkin lymphoma (NHL) involves reviewing medical history, family history, physical examination, and a variety of tests to confirm the disease.
Common diagnostic methods include:
- Physical examination: Doctors check for enlarged lymph nodes, as well as signs of liver or spleen enlargement.
- Complete blood count (CBC): Helps detect anemia, thrombocytopenia, leukopenia, or abnormal increases in white blood cells or platelets. These abnormalities may be linked to bone marrow involvement, splenic enlargement, or gastrointestinal bleeding.
- Blood chemistry tests: Useful for ruling out tumor lysis syndrome (common in aggressive lymphomas such as Burkitt lymphoma). Elevated lactate dehydrogenase (LDH) levels may indicate heavy tumor burden or liver infiltration.
- Imaging studies: CT scans of the neck, chest, abdomen, and pelvis or PET scans are typically performed. MRI of the brain and spinal cord may be required in specific cases.
- Lymph node or tissue biopsy: Recommended if a lymph node is significantly enlarged, persists for more than 4–6 weeks, or continues to grow in size. This remains the gold standard for diagnosis.
- Bone marrow aspiration and biopsy: Helps detect whether lymphoma cells are present in the bone marrow.
- Lumbar puncture: Reserved for high-risk patients with suspected central nervous system involvement.
- Immunophenotyping and molecular testing: Analyzing blood, bone marrow, and lymph node samples helps classify the type of lymphoma more precisely.
Staging of Non-Hodgkin Lymphoma
Staging helps determine the extent of the disease and guides treatment decisions. The Lugano classification, based on the Ann Arbor staging system, is widely used:
- Stage I: Involvement of a single lymph node region or a single lymphoid organ (such as the thymus, spleen, or bone marrow).
- Stage II: Two or more lymph node regions on the same side of the diaphragm, or limited involvement of an adjacent organ.
- Stage III: Lymph node regions on both sides of the diaphragm, possibly including the spleen.
- Stage IV: Widespread disease with extranodal involvement (such as the liver, lungs, or bone marrow), with or without lymph node involvement.
Treatment Options for Non-Hodgkin Lymphoma
The choice of treatment depends on the type, stage, and aggressiveness of the lymphoma, as well as the patient’s overall health.
1. Active Surveillance
For indolent or slow-growing forms of NHL without symptoms, doctors may recommend watchful waiting instead of immediate treatment. Patients are closely monitored until symptoms appear or the disease progresses.
2. Chemotherapy
Chemotherapy drugs target cancer cells throughout the body. Most are delivered intravenously. Side effects can include fatigue, nausea, hair loss, and reduced blood counts.
3. Targeted Therapy
These treatments attack cancer cells more precisely than chemotherapy. For example, monoclonal antibody therapy uses lab-made antibodies to identify and destroy cancerous lymphocytes.
4. Immunotherapy
Also called biologic therapy, this approach strengthens the body’s own immune defenses. CAR T-cell therapy is an advanced option that engineers a patient’s own T-cells to fight lymphoma cells.
5. Radiation Therapy
Radiation uses high-energy X-rays to kill cancer cells. It is often used for localized NHL (Stage I or II) and may also be combined with chemotherapy in more advanced cases.
6. Stem Cell Transplant
High-dose chemotherapy may be followed by a stem cell transplant to restore healthy blood cells. Both autologous (using the patient’s own stem cells) and allogeneic (from a donor) transplants may be considered.
Role of Surgery in NHL
Surgery is rarely used as a treatment for non-Hodgkin lymphoma. Its main role is for biopsy to confirm diagnosis. However, exceptions include:
- Splenectomy (removal of the spleen): Sometimes necessary in splenic marginal zone lymphoma.
- Debulking surgery: Removal of a large abdominal mass before starting chemotherapy in rare cases.
Lifestyle and Prevention Tips for Non-Hodgkin Lymphoma
While there is no guaranteed way to prevent non-Hodgkin lymphoma (NHL), adopting a healthy lifestyle and following medical advice can help support treatment outcomes, boost immunity, and potentially reduce the risk of disease progression.
Recommended Lifestyle Habits
- Follow medical guidance: Always adhere to your doctor’s treatment plan and attend regular follow-up appointments.
- Maintain good hygiene: Wash hands frequently before preparing food, before meals, and after using the restroom to reduce infection risk.
- Keep your living environment clean and well-ventilated to minimize exposure to harmful pathogens.
- Stay active: Engage in regular exercise such as walking, yoga, or light aerobic activities to strengthen overall health.
- Manage stress: Avoid overwork, ensure adequate rest, and practice relaxation techniques such as meditation or deep breathing.
- Think positively: Maintain a cheerful and optimistic mindset to support emotional well-being during treatment.
- Avoid harmful substances: Do not smoke, drink alcohol excessively, or use recreational drugs.
Nutrition for Patients with Non-Hodgkin Lymphoma
- Eat well-cooked food: Avoid raw or undercooked foods to prevent infections. Fermented or pickled foods should also be limited.
- Balanced diet: Ensure meals include essential macronutrients—carbohydrates, protein, and healthy fats—along with vitamins and minerals from fruits and vegetables.
- Choose fresh, natural foods: Avoid processed, canned, or fast foods that are high in unhealthy fats and preservatives.
- Limit salt and sugar: Reduce intake of overly salty or sweet foods.
- Stay hydrated: Drink at least 2 liters of water daily unless otherwise advised by your physician.

How to Lower the Risk of Non-Hodgkin Lymphoma
Although there is no specific preventive method, adopting the following habits may help reduce risk and strengthen the immune system:
- Maintain a nutrient-rich, balanced diet with plenty of fresh fruits and vegetables.
- Establish a healthy work-rest schedule, avoiding late nights and overwork.
- Control stress levels and keep a positive outlook.
- Avoid tobacco, alcohol, and stimulants that can harm the immune system.
- Exercise regularly at a level suitable for your health condition.
