What Is Neurofibromatosis? Causes, Symptoms, and Treatment
Neurofibromatosis (NF) is a rare genetic disorder of the nervous system that causes tumors to develop on nerves. These growths can occur anywhere in the brain, spinal cord, or peripheral nerves.
Depending on the type and severity of the condition, treatment may involve surgical removal of tumors, radiation therapy, or medication to manage symptoms.
Overview of Neurofibromatosis
What is Neurofibromatosis?
Neurofibromatosis is a group of inherited disorders that lead to the growth of tumors along nerves in the body. Most of these tumors are benign (noncancerous), but in some cases they can become malignant (cancerous).
There are three main types of neurofibromatosis:
Neurofibromatosis type 1 (NF1): The most common type, usually diagnosed in childhood or even at birth. NF1 is often associated with café-au-lait spots (light brown skin patches), small benign tumors on or under the skin (neurofibromas), bone deformities, learning difficulties, and an increased risk of malignant peripheral nerve sheath tumors.
Neurofibromatosis type 2 (NF2): Less common than NF1, typically diagnosed in the teenage years or early adulthood. NF2 is characterized by bilateral vestibular schwannomas (tumors on the hearing and balance nerves), which can cause hearing loss, ringing in the ears (tinnitus), and balance problems. Other brain and spinal cord tumors may also occur.
Schwannomatosis: The rarest form of neurofibromatosis, usually identified in adulthood. It causes the development of multiple schwannomas (nerve sheath tumors) throughout the body, leading to chronic pain, muscle weakness, or numbness. Unlike NF2, schwannomatosis does not involve vestibular schwannomas.
Symptoms of Neurofibromatosis
The signs and symptoms of neurofibromatosis vary depending on the type: NF1, NF2, or Schwannomatosis.
Neurofibromatosis Type 1 (NF1)
NF1 is typically diagnosed in childhood. The symptoms may include:
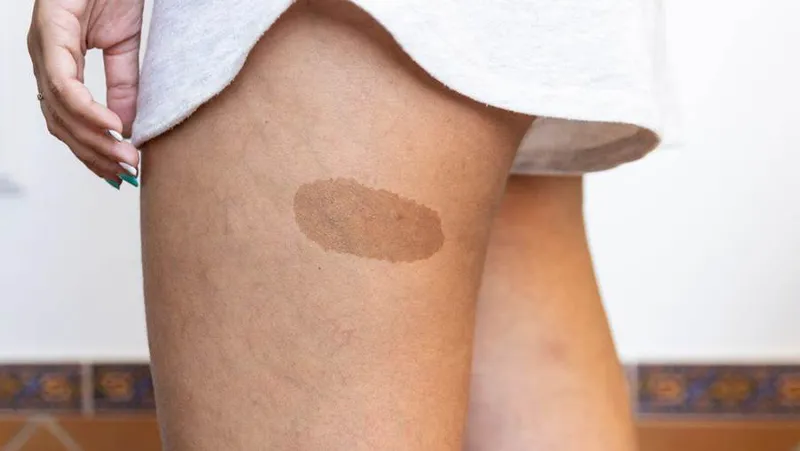
- Café-au-lait spots: Flat, light brown skin patches. Having more than six café-au-lait spots is suggestive of NF1. These usually appear at birth or in early childhood and stop developing after puberty.
- Lisch nodules: Tiny benign bumps on the iris (colored part of the eye). They do not affect vision.
- Neurofibromas: Soft, pea-sized tumors that grow on or under the skin.
- Bone deformities: Such as scoliosis (curved spine) or bowing of the legs.
- Optic pathway gliomas: Tumors that form on the optic nerve, often before age 3.
- Learning difficulties: Usually mild cognitive impairment or attention problems.
- Macrocephaly: Larger-than-average head size due to increased brain volume.
Neurofibromatosis Type 2 (NF2)
NF2 is much less common than NF1 and usually appears in adolescence or early adulthood. Symptoms may include:
- Progressive hearing loss (often due to vestibular schwannomas).
- Poor balance or frequent falls.
- Headaches.
- Numbness or weakness in the arms or legs.
- Vision problems or cataracts.
- Seizures in some cases.
Schwannomatosis
Schwannomatosis is the rarest type of neurofibromatosis and usually develops in adults after age 20, most often between ages 25–30. Unlike NF2, schwannomatosis does not cause vestibular schwannomas, so patients do not typically experience hearing loss.
Symptoms may include:
- Chronic pain anywhere in the body, which may become disabling.
- Numbness or weakness in different body parts.
- Muscle wasting (atrophy).
When to See a Doctor
If you or your child develop unexplained skin changes, tumors, or neurological symptoms suggestive of neurofibromatosis, consult a neurologist or genetic specialist for timely evaluation and treatment.
Causes of Neurofibromatosis
Neurofibromatosis is caused by genetic mutations, which may be inherited from a parent or occur spontaneously at conception. The specific gene involved depends on the type of neurofibromatosis:
Neurofibromatosis type 1 (NF1): Caused by a mutation in the NF1 gene on chromosome 17. This gene normally produces a protein that helps regulate cell growth. A mutation leads to loss of neurofibromin, resulting in uncontrolled cell growth.
Neurofibromatosis type 2 (NF2): Caused by a mutation in the NF2 gene on chromosome 22. The gene produces merlin (schwannomin), a tumor-suppressor protein. Loss of merlin function allows abnormal cell growth.
Schwannomatosis: Linked to mutations in the SMARCB1 and LZTR1 genes, both of which are associated with tumor regulation.
Risk Factors for Neurofibromatosis
Although neurofibromatosis can affect anyone, some factors increase the likelihood of developing the disorder:
- Family history: Having a parent with NF1, NF2, or schwannomatosis significantly raises the risk.
- Childhood onset: NF1 often develops in childhood, while NF2 and schwannomatosis typically appear in adolescence or adulthood.
- Environmental exposure (rare): Contact with harmful chemicals or radiation during pregnancy may contribute in some cases.
Both men and women are equally affected.
Diagnosis of Neurofibromatosis
Doctors usually begin with a physical exam and a review of personal and family medical history. Diagnostic tests may include:
Skin examination: To identify café-au-lait spots (suggestive of NF1).
Eye exam: An ophthalmologist can detect Lisch nodules, cataracts, or vision loss.
Hearing and balance tests: Audiometry may help diagnose hearing impairment and balance problems in NF2.
Imaging tests: X-ray, CT scan, or MRI to detect bone abnormalities or tumors in the brain and spinal cord. MRI is particularly useful for identifying optic gliomas in NF1 and monitoring NF2 or schwannomatosis.
Genetic testing: Available for NF1 and NF2 and may also be performed during pregnancy to confirm diagnosis.

Treatment of Neurofibromatosis
Treatment depends on the type and severity of the condition. While there is no cure, therapies help manage symptoms and prevent complications.
Medications
- Selumetinib (FDA-approved): Used in children (age 2+) with NF1 to slow or shrink tumors by inhibiting abnormal cell signaling.
- Pain management drugs: Especially important in schwannomatosis, may include Gabapentin, Pregabalin, Amitriptyline, Duloxetine, Topiramate, or Carbamazepine.
- Chemotherapy: Reserved for cases involving malignant tumors.
Surgery
- Recommended for large or symptomatic tumors, or when there is a risk of malignant transformation and metastasis.
- Surgical removal helps relieve symptoms such as pain, vision impairment, or nerve compression.
Lifestyle and Prevention of Neurofibromatosis
Healthy Lifestyle Habits
While there is no cure for neurofibromatosis, adopting healthy habits can help slow disease progression and improve overall well-being:
- Follow your doctor’s treatment plan: Adherence to prescribed therapies helps manage symptoms and prevent complications.
- Monitor symptoms regularly: Contact your doctor if new symptoms appear or existing ones worsen.
- Avoid harmful exposures: Pregnant women should avoid smoking, radiation, and toxic chemicals to reduce potential risks.
Nutrition
There is no specific diet proven to treat neurofibromatosis. However, maintaining a balanced, nutrient-rich diet is essential for overall health and immune support.

Prevention of Neurofibromatosis
Currently, there is no known way to prevent neurofibromatosis.
For individuals planning a family, genetic counseling is recommended. This can help assess the risk of passing on inherited conditions and provide guidance on family planning options.
