Meningioma: Causes, Symptoms, and Treatment
Understanding Meningioma
What is Meningioma?
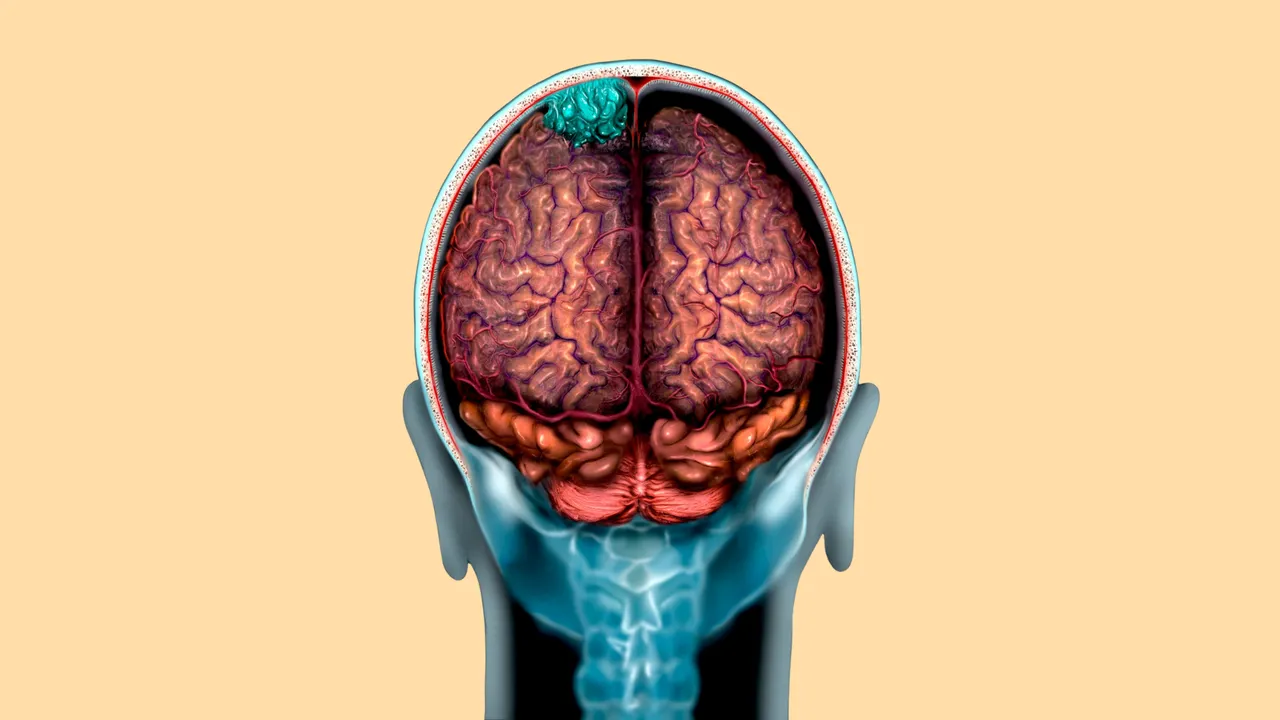
A meningioma is a tumor that arises from the meninges, the membranes surrounding the brain and spinal cord. While it is not considered a primary brain tumor, it can exert pressure on surrounding brain tissue, nerves, and blood vessels, leading to symptoms. Meningiomas are the most common type of tumor found in the head region.
Most meningiomas grow very slowly, sometimes over many years without causing noticeable symptoms. However, when the tumor becomes large enough, it can lead to significant health issues due to compression of adjacent structures.
Meningiomas occur more frequently in women and are typically diagnosed in older adults, but they can develop at any age. Because of their slow growth, not all meningiomas require immediate treatment. Many cases are managed with regular observation over time.
Classification of Meningiomas
Meningiomas are classified into three grades based on histopathological analysis:
- Grade I (Benign/Low Grade): Slow-growing cells with low risk of recurrence. This type accounts for about 80% of cases.
- Grade II (Atypical/Intermediate): Faster-growing, with a higher chance of recurrence after surgery. Subtypes include chordoid meningioma and clear cell meningioma.
- Grade III (Malignant/High Grade): Aggressive and rapidly spreading tumors. This grade includes papillary meningioma and rhabdoid meningioma.
Symptoms of Meningioma
Because meningiomas usually grow slowly, symptoms may not become noticeable until the tumor is large enough to compress surrounding brain or spinal cord structures. The type and severity of symptoms depend largely on the tumor’s location.
Common Symptoms
- Persistent headaches, often worse in the morning
- Dizziness, nausea, and vomiting
- Visual changes, including double vision, blurred vision, or loss of vision
- Hearing loss
- Seizures
- Changes in behavior or personality
- Memory problems
- Muscle weakness or paralysis in specific body parts
- Increased reflexes
Location-Specific Symptoms
- Olfactory groove meningioma: Partial or complete loss of the sense of smell
- Parasagittal meningioma: Weakness or paralysis of the legs and lower body
- Sphenoid wing meningioma: Cavernous sinus syndrome and bulging of the eye (proptosis)
Spinal Meningioma Symptoms
- Localized pain at the tumor site
- Muscle weakness, loss of tone, and reduced or absent reflexes
- Neurological deficits such as paralysis or impaired mobility

Complications of Meningioma
Both the tumor and its treatment (commonly surgery or radiotherapy) can lead to long-term complications, including:
- Difficulty concentrating
- Memory loss
- Personality changes
- Seizures
- Weakness or paralysis of limbs
- Sensory changes
- Language or speech problems
When to See a Doctor
Most meningioma symptoms develop gradually, but some situations require immediate medical attention. Go to the emergency department if you experience:
- A sudden onset seizure
- Sudden changes in vision or memory
Schedule an appointment with a neurologist if you have persistent symptoms that concern you, such as headaches that progressively worsen over time.
Meningiomas are often discovered incidentally on imaging studies like CT or MRI scans performed for other health reasons, as they may remain asymptomatic for years.

Causes of Meningioma
The exact cause of meningioma is still unknown. However, researchers have identified several risk factors and genetic components that may contribute to its development:
- Gene mutations: Meningiomas are associated with genetic changes. Around 40–80% of meningiomas show abnormalities on chromosome 22, which is involved in tumor suppression. Most of these mutations occur sporadically, but some may be inherited.
- Radiation exposure: Exposure to radiation—especially during childhood—increases the risk of developing meningioma.
- Neurofibromatosis Type 2 (NF2): This rare inherited condition significantly raises the risk of meningioma.
Who Is at Risk of Developing Meningioma?
Certain groups of people are more likely to develop meningioma, including:
- Adults: Meningiomas most commonly affect adults, especially those over 66 years of age. The highest incidence occurs between ages 70–80.
- Gender: Women are about three times more likely than men to develop meningioma. However, malignant meningiomas tend to occur more often in men.
- Race/Ethnicity: In the U.S., Black individuals have a higher incidence of meningioma compared to other ethnic groups.

Risk Factors for Meningioma
Factors that may further increase your risk include:
- Radiation exposure: Especially to the head (such as from radiation therapy), which increases the likelihood of developing meningioma.
- Female hormones: The higher incidence in women may be linked to female hormones. Research suggests that oral contraceptive use or hormone replacement therapy (HRT) may raise the risk.
- Neurofibromatosis Type 2 (NF2): This inherited nervous system disorder increases the risk of meningioma and other brain tumors.
- Obesity: A higher body mass index (BMI) has been linked to an increased risk of meningioma, though the exact mechanism remains unclear.
Diagnosis and Tests
To diagnose a meningioma, your doctor will perform a full physical and neurological examination to assess any abnormal signs that may be related to the tumor. Common diagnostic tools include:
- Brain MRI (Magnetic Resonance Imaging): Contrast-enhanced MRI is the most accurate method for detecting meningiomas. It provides detailed images of the brain’s internal structures using magnetic fields and radio waves.
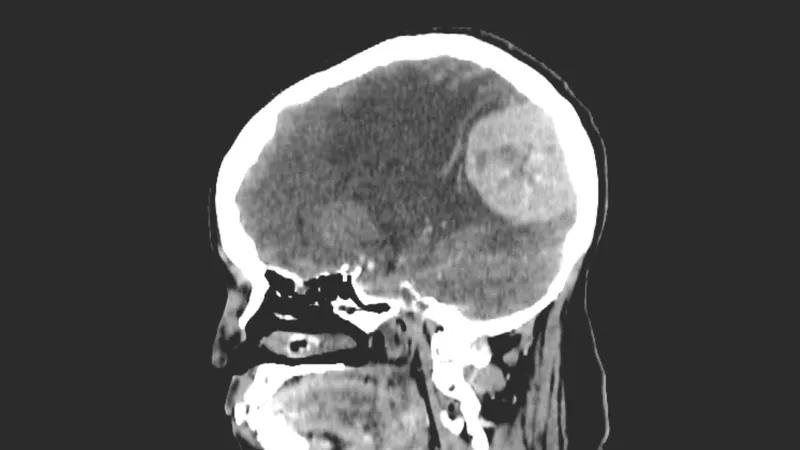
- CT Scan (Computed Tomography): If MRI is not possible, your doctor may recommend a contrast-enhanced head CT to produce detailed cross-sectional images of the brain using X-rays and computer technology.
- Biopsy: In some cases, a biopsy may be performed to obtain a tissue sample from the tumor. This sample is analyzed to determine whether the tumor is benign or malignant and to rule out other types of growths.
Treatment Options
Watchful Waiting (Active Surveillance)
Recommended for small, asymptomatic tumors or those not located near critical nerves or blood vessels. Patients may undergo regular MRI or CT scans to monitor tumor growth over time.
Surgery
Surgery is the primary treatment for symptomatic or large meningiomas. The goal is to completely remove the tumor and reduce the risk of recurrence. However, complete removal may be limited if the tumor is located near delicate brain structures or major blood vessels.
Radiation Therapy
Used for tumors that cannot be surgically removed or for residual tumor tissue after surgery. Types of radiation therapy include:
- Stereotactic Radiosurgery (SRS): A non-invasive technique using focused beams of radiation precisely targeted at the tumor.
- External Beam Radiation Therapy (EBRT): The most common form, delivering radiation from outside the body.
- Brachytherapy: Placement of radioactive seeds directly near the tumor.
Palliative (Supportive) Care
Focuses on improving quality of life by managing symptoms and psychological impact. This may include medications, dietary changes, relaxation techniques, and emotional support.
Chemotherapy
Rarely used for meningiomas but may be considered in cases of recurrent or progressive tumors that do not respond to surgery or radiation. Bevacizumab, a targeted therapy, has shown promising results in some malignant meningiomas.
Lifestyle Tips to Manage Meningioma
People with meningioma can support their treatment and recovery by adopting healthy daily habits:
- Regular Monitoring: If the tumor is small and does not require immediate intervention, your doctor may recommend periodic MRI or CT scans to track its growth.
- Adequate Rest: Balance rest with gentle physical activities such as walking or yoga to maintain overall health and reduce stress.
- Stress Management: Use relaxation methods such as meditation, deep breathing, or enjoyable hobbies to help reduce anxiety.
- Healthy Living: Avoid alcohol, smoking, and stimulants. These habits can harm overall health and slow recovery.
- Keep Appointments: Always follow your scheduled checkups so your doctor can monitor tumor progression and adjust treatment if needed.

Nutrition for Better Recovery
Good nutrition plays an important role in supporting health and recovery:
- Eat Plenty of Fruits and Vegetables: Provide vitamins, minerals, and antioxidants to help the body combat abnormal cell growth.
- Include Healthy Fats: Prioritize unsaturated fats from fatty fish (salmon, mackerel), olive oil, and chia seeds to reduce inflammation and support brain function.
- Choose High-Quality Protein: Include lean protein sources like fish, poultry, beans, lentils, and low-fat dairy to help maintain and repair tissues.
- Stay Hydrated: Drink enough water to help your body flush out toxins and maintain essential functions.
- Limit Processed Foods and Refined Sugar: Avoid foods high in sugar, unhealthy fats, and salt as they may contribute to inflammation and hinder recovery.
Prevention Tips for Meningioma
There is no guaranteed way to prevent meningioma, but you can lower your risk through these measures:
- Limit Radiation Exposure: Minimize exposure to radiation, especially head X-rays, unless absolutely necessary for diagnosis or treatment.
- Maintain a Healthy Lifestyle: Eat a balanced diet, avoid smoking, and limit alcohol or other harmful substances to protect overall health and reduce cancer risks.
- Manage Weight: Obesity may increase the risk of meningioma. Maintain a healthy BMI through a balanced diet and regular exercise.
- Monitor Genetic Risks: Individuals with inherited conditions such as Neurofibromatosis Type 2 should be closely monitored by healthcare professionals to detect meningiomas early.

