Endometrial Cancer: Symptoms, Causes, and Treatment Options
What is Endometrial Cancer?
Endometrial cancer (also called endometrial carcinoma) begins in the cells of the lining inside the uterus, known as the endometrium. It is the most common type of uterine cancer.
This disease is distinct from cancers that start in the connective tissue or muscles of the uterus, which are classified as uterine sarcomas. Around 80% of all endometrial cancers are adenocarcinomas, meaning they arise from gland-forming cells within the endometrium. When detected early, endometrial cancer is often highly curable.
Doctors classify endometrial cancer into two main types and four stages:
Type 1: Low-grade endometrial carcinoma (most often grade 1 or 2 adenocarcinomas). These tumors usually invade less than 50% of the endometrial lining and generally have an excellent prognosis. The 5-year survival rate can be close to 100%.
Type 2: High-grade endometrial carcinoma, which includes more aggressive tumor patterns such as solid growth >50%, infiltrative spread, and/or tumor necrosis. The 5-year survival rate is significantly lower, averaging around 46%.
Stages of Endometrial Cancer
- Stage I: Cancer is confined to the uterus.
- Stage II: Cancer has spread to the cervix.
- Stage III: Cancer has spread to the vagina, ovaries, and/or lymph nodes.
- Stage IV: Cancer has spread to the bladder or distant organs in the body.
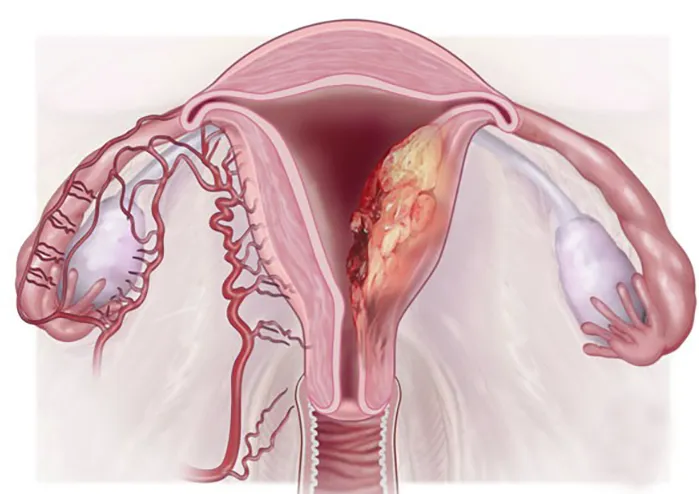
Symptoms of Endometrial Cancer
Signs and symptoms may include:
- Abnormal vaginal bleeding or discharge unrelated to the menstrual cycle. Over 90% of women diagnosed with endometrial cancer present with unusual vaginal bleeding.
- Postmenopausal bleeding.
- Painful or difficult urination.
- Pain during sexual intercourse.
- Pelvic pain or the presence of a pelvic mass.

Possible Complications
The most serious complication of endometrial cancer is death, but prognosis is generally favorable if diagnosed at an early stage. Other complications may include:
- Anemia due to chronic bleeding.
- Metastasis to other organs such as the lungs, liver, or bones.
When to See a Doctor
You should consult a healthcare professional if you experience symptoms suggestive of endometrial cancer – especially abnormal vaginal bleeding. Women with inherited genetic risks should also seek medical evaluation and counseling for early detection and preventive care.
Causes of Endometrial Cancer
Most cases of endometrial cancer are believed to begin with unopposed endometrial hyperplasia—a condition in which the lining of the uterus (endometrium) grows excessively under the influence of estrogen without the balancing effect of progesterone or progestin. Over time, this abnormal growth can progress from simple to complex hyperplasia and eventually to cancer.
Who Is at Risk of Endometrial Cancer?
Endometrial cancer is the most common gynecologic malignancy among women in the United States and remains a leading cause of morbidity and mortality. Each year, more than 60,000 new cases are diagnosed, resulting in nearly 11,000 deaths.
The disease primarily affects postmenopausal women, with an average age at diagnosis of 60 years. Most cases occur between the ages of 45 and 75.
Risk Factors for Endometrial Cancer
Several factors can increase a woman’s risk of developing endometrial cancer:
- Age: Most cases are diagnosed after menopause.
- Hormone imbalance: Elevated levels of estrogen without sufficient progesterone can stimulate abnormal endometrial growth.
- Obesity: A BMI of 25 or higher significantly raises the risk.
- Genetics: Lynch syndrome, an inherited condition, increases the likelihood of endometrial, ovarian, and other cancers.
- Early menarche (onset of menstruation at a young age).
- Late menopause.
- Diabetes.
- Tamoxifen use: Women treated with Tamoxifen for breast cancer are at increased risk.
Diagnosis of Endometrial Cancer
To diagnose endometrial cancer, doctors will review your medical history, conduct a physical examination, and order laboratory and imaging tests.
Common diagnostic methods include:
Pelvic examination: The doctor examines the uterus, ovaries, and other reproductive organs. A speculum may be used to view the vagina and cervix, while manual palpation helps detect abnormalities.
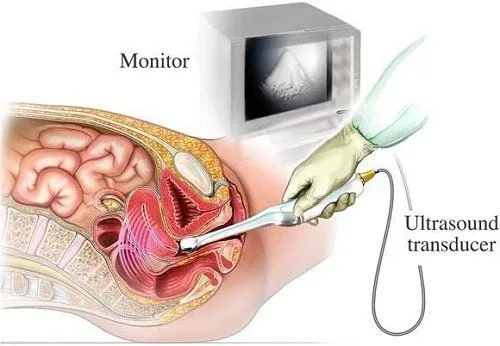
Imaging tests: The most common is transvaginal ultrasound, where a probe inserted into the vagina uses sound waves to create images of the uterus. This helps assess the thickness and structure of the endometrium and detect possible tumors.
Hysteroscopy: A thin, lighted tube is inserted through the vagina and cervix into the uterus to visualize the endometrium directly.
Endometrial biopsy: A tissue sample is taken from the uterine lining and examined under a microscope to detect cancerous or abnormal cells.
Dilation and curettage (D&C): If a biopsy is inconclusive, D&C may be performed. During this minor procedure, the cervix is dilated and uterine tissue is scraped for analysis.
Treatment of Endometrial Cancer
The main treatment for endometrial cancer is surgery, often involving hysterectomy (removal of the uterus), sometimes combined with removal of the fallopian tubes and ovaries. This procedure prevents future pregnancy and induces early menopause if the ovaries are removed.
Additional treatments depend on the stage and type of cancer, overall health, and patient preferences. Options include:
Surgery: Total hysterectomy, often with removal of fallopian tubes and ovaries. Lymph nodes may also be sampled to check for cancer spread and determine staging.
Radiation therapy: Uses high-energy beams (X-rays, protons) to kill cancer cells. It can be given before surgery to shrink the tumor or after surgery to reduce recurrence risk.
Chemotherapy: Involves powerful drugs that kill cancer cells. It may be used after surgery to prevent recurrence or before surgery to shrink the tumor. Chemotherapy is often combined with radiation in advanced cases.
Hormone therapy: Involves medications that lower or block hormones, slowing cancer growth. It may be recommended for advanced or recurrent endometrial cancer.
Targeted therapy: Uses drugs designed to attack specific molecular changes in cancer cells, often combined with chemotherapy for advanced disease.
Immunotherapy: Helps the body’s immune system recognize and destroy cancer cells. It may be considered for advanced or treatment-resistant endometrial cancer.
Palliative care: Specialized supportive care that focuses on symptom management and quality of life. When combined with active treatment, palliative care can help patients feel better and live longer.
Lifestyle and Prevention of Endometrial Cancer
Because endometrial cancer is strongly associated with obesity, maintaining a healthy weight through balanced nutrition and regular physical activity is one of the most effective ways women can reduce their risk.
Healthy Lifestyle Habits
Adopting positive daily habits can help slow disease progression and improve overall health:
Follow your treatment plan: Strictly adhere to your doctor’s prescribed therapies and stay engaged in your care.
Routine checkups: Schedule regular medical follow-ups after treatment to monitor recovery and detect recurrence early.
Stay active: Engage in regular exercise to maintain a healthy body weight and body mass index (BMI), which helps lower obesity-related risk.
Avoid harmful substances: Quit smoking and limit or avoid alcohol and other stimulants.
Nutrition Guidelines
A balanced diet is key to overall well-being and cancer risk reduction. Recommendations include:
Eat a variety of fresh fruits, vegetables, whole grains, and legumes.
Limit fast food, fried or greasy meals, saturated fats, animal organ meats, and high-calorie foods or beverages loaded with sugar.

Prevention of Endometrial Cancer
While there is no guaranteed way to prevent endometrial cancer, research suggests several strategies may reduce risk:
Manage risk factors: Maintain a healthy weight, control diabetes, and avoid prolonged unopposed estrogen exposure.
Consider hormonal contraception: The use of birth control pills or other forms of hormonal contraceptives may help reduce risk.
Lifestyle modification: Healthy eating and regular physical activity remain the cornerstone of prevention.
