What Is Colorectal Cancer? Can It Be Prevented?
Understanding Colorectal Cancer
What Is Colorectal Cancer?
Colorectal cancer begins in the colon (large intestine), a long tube that carries digested food to the rectum.
The wall of the colon and rectum is made up of mucous membranes, tissue, and muscle layers. Colorectal cancer starts in the innermost lining, the mucosa, which contains cells that produce mucus and other fluids. When these cells undergo mutations or abnormal changes, they can form colorectal polyps.
Over time, colorectal polyps may develop into cancer (it typically takes about 10 years for most polyps to become cancerous). If not detected or treated, the cancer can grow through the tissue and muscle layers, eventually spreading to the outer layer of the colon or rectum. Colorectal cancer may also metastasize to other parts of the body through lymph nodes or blood vessels.
Symptoms of Colorectal Cancer
Common Signs and Symptoms
You can have colorectal cancer without experiencing any symptoms. Even if you do notice symptoms, they do not always mean you have cancer, as some of them may be caused by less serious conditions.
- Blood in or on your stool: You may see blood in the toilet after a bowel movement, on the toilet paper, or notice that your stool is dark or bright red. Keep in mind that blood in stool does not necessarily mean colorectal cancer — other causes include hemorrhoids, anal fissures, or even eating beets.
- Changes in bowel habits: Persistent constipation and/or diarrhea, or the feeling that you still need to pass stool even after a bowel movement.
- Abdominal pain: Ongoing, unexplained stomach pain that does not go away or becomes severe. While abdominal pain can have many causes, it is best to seek medical advice if it is frequent or unusual.
- Bloating: Feeling unusually full or bloated, especially if this lasts more than a week, worsens over time, or is accompanied by vomiting or blood in the stool.
- Unexplained weight loss: Significant weight loss without trying.
- Nausea or vomiting: Frequent vomiting without an obvious cause, or vomiting multiple times within 24 hours.
- Fatigue and shortness of breath: These can be signs of anemia, which may be caused by colorectal cancer.
Possible Complications of Colorectal Cancer
Colorectal cancer can lead to a wide range of complications. Tumor-related complications include bleeding, obstruction, perforation, and fistula formation into surrounding organs. Metastatic disease may present with different symptoms depending on where the cancer spreads.
Surgical complications may include bleeding, wound or organ infections, anastomotic leaks, injury to nearby structures such as the ureters or duodenum, and long-term issues like incisional hernias.
When to See a Doctor
You should see a doctor if you notice any of the above signs or symptoms that persist or worsen over time. Early evaluation can lead to timely diagnosis and treatment, improving your chances of successful outcomes.
Causes of Colorectal Cancer
Why Colorectal Cancer Develops
Like all cancers, colorectal cancer occurs when cells in the body grow abnormally and divide uncontrollably. Normally, cells in your body grow, divide, and die in an orderly way — this process keeps your body healthy and functioning.
In colorectal cancer, the cells lining your colon and rectum continue to grow and divide even when they should die. These cancerous cells often arise from polyps in the colon or rectum.
Colon and rectal polyps are quite common, especially as you get older. Most polyps are benign (noncancerous). However, some types of polyps can eventually turn into cancer, usually over many years. The likelihood of a polyp becoming cancerous depends on its type:
- Adenomatous polyps (adenomas): These polyps sometimes turn into cancer. Because of this, adenomas are considered precancerous. There are three types: tubular, villous, and tubulovillous. Tubular adenomas are the most common. Villous adenomas are the least common but have the highest risk of becoming cancerous.
- Hyperplastic and inflammatory polyps: These are more common and are usually not precancerous. However, people with large hyperplastic polyps (greater than 1 cm) may need more frequent colonoscopy screening.
- Sessile serrated polyps (SSPs) and traditional serrated adenomas (TSAs): These are typically treated like adenomas because they carry a higher risk of progressing to cancer.
Researchers are still not completely sure why some people develop precancerous polyps that later turn into colorectal cancer. Scientists believe that several risk factors — including genetic predisposition and lifestyle choices — may increase the likelihood of developing these polyps and, eventually, colorectal cancer.
Having one or more risk factors does not mean you will definitely get colorectal cancer. It only means your risk is higher compared to someone without these risk factors.
Risk Factors for Colorectal Cancer
Who Is at Risk?
People at increased risk for colorectal cancer include:
- Age: The risk rises with age. Most cases occur in people over 50.
- Sex: Men are slightly more likely to develop colorectal cancer than women.
- Family history: Having a family history of colorectal cancer or certain inherited syndromes — such as Lynch syndrome or familial adenomatous polyposis (FAP) — increases your risk.
- Personal history: People who have previously had colorectal cancer or certain types of polyps are at higher risk of developing the disease again.
Additional Risk Factors
Certain lifestyle and health factors can further increase your risk:
- Smoking: Use of tobacco products, including chewing tobacco and e-cigarettes, increases colorectal cancer risk.
- Excessive alcohol use: Men should limit alcohol to two drinks per day and women to one drink per day. Even light alcohol consumption may increase your risk.
- Obesity: Diets high in fat and calories can lead to excess weight, which raises your cancer risk.
- High intake of red or processed meat: Processed meats include bacon, sausage, and deli meats. Limit red and processed meat consumption to no more than twice per week.
- Sedentary lifestyle: Any form of regular physical activity can help lower your risk of colorectal cancer.

Diagnosis and Treatment of Colorectal Cancer
Diagnostic Tests and Screening
If you have symptoms suggestive of colorectal cancer, your doctor may recommend tests to detect and screen for the disease. These tests can also find colorectal cancer at an early stage.
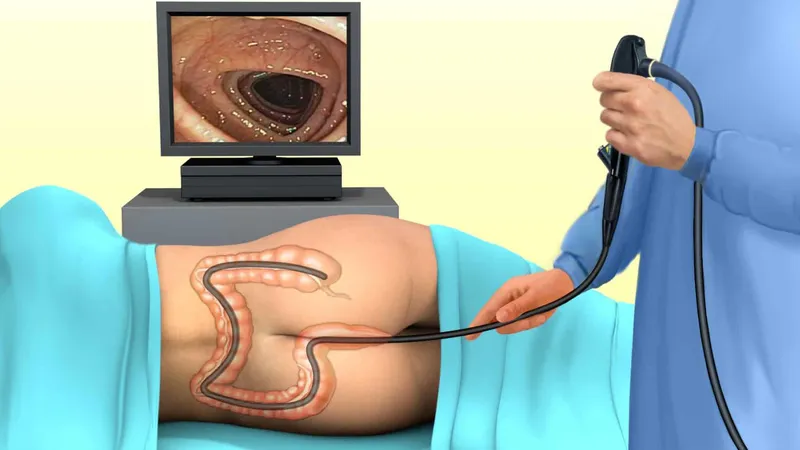
Colonoscopy
Colonoscopy is considered the gold standard diagnostic test for colorectal cancer. It is highly accurate and allows doctors to precisely locate tumors. During the procedure, a doctor uses a flexible tube with a light and camera to view the entire colon and rectum. Polyps can be removed, or tissue samples (biopsies) can be taken for further testing.
Fecal Occult Blood Test (FOBT)
This test looks for hidden (occult) blood in the stool. Many conditions can cause blood in the stool, so a positive result does not necessarily mean cancer is present.
Barium Enema X-ray
Barium is a contrast dye used to detect abnormalities in the gastrointestinal tract during an X-ray. A healthcare provider introduces the barium into the colon as an enema to outline the colon and rectum.
CT Colonography (Virtual Colonoscopy)
This test produces detailed images of the colon and rectum using CT scanning. Although it is less invasive than colonoscopy, a follow-up colonoscopy is required if a tumor or polyp is detected.
Additional Imaging
Ultrasound, CT scans, or MRI may be used to determine whether the cancer has spread to other organs.
Treatment Options for Colorectal Cancer
The treatment plan depends on several factors, including:
- The size, location, and stage of the tumor
- The risk of recurrence
- The patient’s overall health
Treatment approaches may include surgery, chemotherapy, radiation therapy, targeted therapy, immunotherapy, and palliative care to manage symptoms and improve quality of life.
Surgery
Surgery is the primary treatment for colorectal cancer when the cancer is confined to the colon or rectum. The goal is to remove the cancerous tissue — including the tumor and affected lymph nodes — and to prevent further spread.
In most cases, the surgeon reconnects the remaining sections of the colon. In some cases, a temporary or permanent colostomy (stoma) may be required to divert stool into an external pouch.
Surgery can completely remove early-stage cancers. For later-stage cancers, surgery may not stop the spread but can relieve symptoms such as bowel obstruction.
Types of Colorectal Cancer Surgery
- Local excision: Removes early-stage cancer or polyps and a small margin of surrounding healthy tissue.
- Colectomy: Removes part or all of the colon. If only a portion is removed, the surgeon reconnects the healthy segments. Total colectomy is less common and is usually performed when multiple polyps are present.
- Relief of obstruction: If a tumor blocks part of the colon, a stent may be inserted to open the bowel. If stenting fails or the blockage is severe, a colectomy with colostomy may be performed.
Surgery can be performed as an open procedure (single large incision) or as a laparoscopic (minimally invasive) procedure with several small incisions.
Medical Treatments
- Chemotherapy: Uses cancer-killing drugs that circulate throughout the body. It may be given before surgery to shrink tumors, after surgery to reduce recurrence risk, or to manage symptoms in advanced stages. Side effects occur because chemotherapy affects both cancerous and healthy cells.
- Targeted Therapy: Uses drugs that specifically attack certain proteins involved in cancer growth. These therapies generally have fewer side effects compared to chemotherapy.
- Immunotherapy: Helps the immune system recognize and attack cancer cells. It may benefit patients with advanced colorectal cancer. Potential side effects include autoimmune reactions where the body attacks its own healthy cells.
- Radiation Therapy: Uses high-energy beams to kill cancer cells or prevent them from dividing. It is often used before surgery to shrink rectal tumors or combined with chemotherapy (chemoradiation).
Palliative and End-of-Life Care
If colorectal cancer spreads to distant organs (stage 4), it is typically no longer curable. Treatment focuses on improving comfort and quality of life:
- Surgery to relieve obstructions
- Radiation or chemotherapy to shrink tumors
- Pain management
- Managing side effects of medications
- Home care and hospice support
Lifestyle & Prevention of Colorectal Cancer
Healthy Habits to Slow Disease Progression
Lifestyle
- Regular Checkups: Visit your doctor as scheduled to monitor your health status and adjust your treatment plan if needed.
- Exercise Regularly: Moderate, consistent physical activity can help lower your risk of colorectal cancer. Exercise also helps reduce the risk of obesity, which is linked to colorectal and other cancers.
- Avoid Prolonged Sitting: Stand up and move around every hour to improve circulation.
Nutrition
- Eat a high-fiber diet rich in fruits and vegetables.
- Limit red meat and processed meats.
- Choose healthy fats such as those from avocados, olive oil, fish oil, and nuts instead of saturated fats.

Prevention of Colorectal Cancer
You may not be able to completely prevent colorectal cancer, but you can lower your risk by managing modifiable risk factors:
- Avoid Tobacco: If you smoke, talk to your doctor about cessation programs that can help you quit.
- Drink Alcohol in Moderation: Stay within recommended safe limits.
- Maintain a Healthy Weight: Obesity increases colorectal cancer risk.
- Adopt a Balanced Diet: Emphasize fruits and vegetables while limiting red meat, processed foods, high-fat, and high-calorie foods.
- Know Your Family History: If a parent, sibling, or child has had colorectal cancer or advanced polyps — or if any family member was diagnosed before age 45 — discuss early screening with your doctor.
- Screening: If you have chronic inflammatory bowel disease or a family history of colorectal cancer, your doctor may recommend starting screening before age 45.
