Placental Cancer (Choriocarcinoma): Causes, Symptoms, Diagnosis, and Treatment
Understanding Choriocarcinoma
What is Choriocarcinoma?
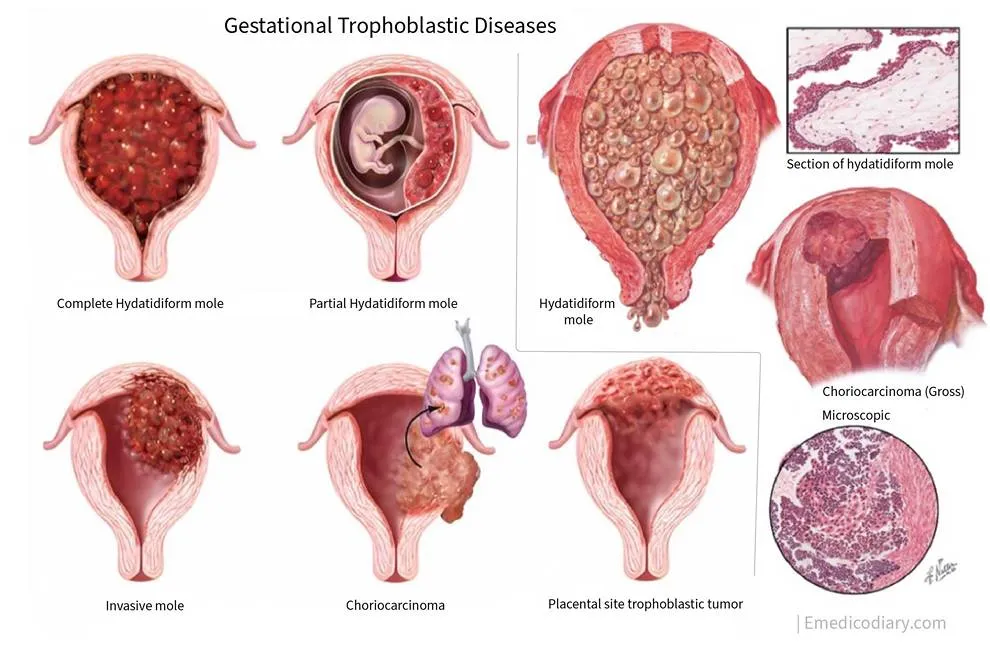
Choriocarcinoma is a rare, fast-growing cancer that originates from placental cells. It belongs to a group of disorders known as gestational trophoblastic diseases (GTD). This cancer typically starts in the placenta—the organ that nourishes a developing fetus during pregnancy—but it is not confined to the uterus. It has the potential to spread (metastasize) to other organs in the body.
There are two main types of choriocarcinoma:
- Gestational choriocarcinoma: This develops as a direct complication of pregnancy.
- Non-gestational choriocarcinoma: This is unrelated to pregnancy and can occur in both women and men, usually as part of a mixed germ cell tumor.
Choriocarcinoma has been described in medical literature as far back as 400 B.C. by Hippocrates.
Symptoms of Choriocarcinoma
Common Signs and Symptoms
Choriocarcinoma can cause a variety of symptoms, particularly in women who have recently been pregnant. Common signs include:
- Abnormal vaginal bleeding: This is the most frequent symptom. Bleeding may be intermittent, heavy, or accompanied by unusual vaginal discharge.
- Pelvic pain: Patients may feel discomfort or pain in the lower abdomen.
Symptoms of Metastasis
If the cancer spreads to other organs, additional symptoms may appear depending on the site of metastasis:
- Vagina: Heavy bleeding, abnormal discharge, or small nodules inside the vaginal wall.
- Lungs: Cough, shortness of breath, or chest pain.
- Brain: Seizures, headaches, dizziness, or other neurological problems.
- Liver or kidneys: Pain or pressure in the abdomen.
Because of the aggressive nature of the disease, early recognition of these symptoms and prompt medical evaluation are crucial.

Complications of Choriocarcinoma
Choriocarcinoma grows rapidly and can lead to serious complications if untreated:
Rapid metastasis: Due to its fast growth and invasive potential, the cancer can quickly spread to the lungs, brain, liver, kidneys, and vagina—causing severe symptoms such as difficulty breathing, chest pain, seizures, headaches, and organ dysfunction.
Death: Without timely diagnosis and treatment, choriocarcinoma can be fatal.
Chemotherapy-related side effects: Although chemotherapy is highly effective, it can cause adverse effects such as:
- Nausea and vomiting
- Hair loss
- Diarrhea
- Fever and infection
- Anemia requiring blood transfusion
- Long-term risk of secondary cancers

When to See a Doctor
You should seek medical advice from an obstetrician–gynecologist if you experience abnormal vaginal bleeding or pelvic pain, particularly if you have a history of molar pregnancy or develop symptoms within one year after childbirth.
Causes of Choriocarcinoma (Placental Cancer)
Choriocarcinoma arises when the cells that form the placenta—called trophoblastic cells—undergo malignant transformation. While the exact mechanism of this process is not fully understood, several biological factors have been linked to the development of this rare cancer:
Hydatidiform mole (molar pregnancy): Around 50% of choriocarcinoma cases develop after a molar pregnancy. This occurs when fluid-filled sacs or abnormal tissue grow inside the uterus instead of a normal placenta. Both complete and partial molar pregnancies can trigger abnormal trophoblastic cell proliferation, potentially leading to cancer.
Other types of pregnancy: Choriocarcinoma can also develop after a normal pregnancy, miscarriage, ectopic pregnancy, or even after childbirth. Any type of pregnancy may activate abnormal growth of placental cells.
Non-gestational choriocarcinoma: In rare cases, this cancer can develop without a preceding pregnancy. It usually arises in the ovaries, testes, or uterus as part of a germ cell tumor. These cells may produce human chorionic gonadotropin (hCG) and appear similar to trophoblastic cells under the microscope.
Genetic and biological factors: Some genetic alterations have been associated with choriocarcinoma, including overexpression of p53 and MDM2 genes. Other factors such as NECC1, EGF receptor, E-cadherin, and HLA-G may contribute to changes in the tumor microenvironment and local immune evasion.
Abnormal pregnancies: Any pregnancy that does not develop normally—including miscarriages, ectopic pregnancies, or gestational tumors—can predispose to abnormal trophoblastic cell growth.
Risk of Choriocarcinoma
Who is at risk?
Anyone who has been pregnant may develop choriocarcinoma, including individuals who have had:
- A normal full-term pregnancy
- A miscarriage, ectopic pregnancy, or abortion
Choriocarcinoma can also develop in men or in women unrelated to pregnancy as part of germ cell tumors, though this is extremely rare.
Risk factors that increase the likelihood of choriocarcinoma
- Hydatidiform mole (molar pregnancy): This is the strongest risk factor. Individuals with a history of complete molar pregnancy have the highest risk. About 50% of all choriocarcinoma cases develop from a molar pregnancy.
- Maternal age: Women are at higher risk if they become pregnant at an early age (under 20) or later in life (over 40).
- Abnormal pregnancies: A history of ectopic pregnancy, miscarriage, or abortion also raises the risk.
Diagnosis and Treatment of Choriocarcinoma (Placental Cancer)
Diagnostic Methods and Tests
Choriocarcinoma is diagnosed through a combination of laboratory tests and imaging studies to confirm the presence of the tumor and assess how far the cancer has spread. Common diagnostic methods include:
Clinical Examination
- Pelvic exam: The doctor checks the uterus and ovaries for masses or abnormalities.
- Physical examination: To detect any signs of tumors or abnormal findings in the rest of the body.
Blood Tests
- hCG (human chorionic gonadotropin) test: People with choriocarcinoma have very high hCG levels, even when not pregnant. This is a key test for diagnosis and for monitoring disease progression.
- Liver and kidney function tests: To evaluate how the disease is affecting these organs.
- Complete blood count (CBC): To assess overall blood health and detect complications from cancer or its treatment.
Imaging Studies
- Pelvic ultrasound: Provides an initial look at uterine size, structure, and the presence of masses or ovarian abnormalities.
- CT scan (Computed Tomography): Used to determine if the cancer has spread to other organs such as the lungs, brain, or liver.
- MRI (Magnetic Resonance Imaging): Offers detailed images of tumors and surrounding tissues.
- Chest X-ray: Helps check for lung metastases.
Post-molar pregnancy surveillance
Individuals who have had a molar pregnancy require close monitoring to detect early signs of choriocarcinoma.
Treatment Options
Treatment depends on the stage of the cancer, the extent of spread, and the patient’s overall health.
Chemotherapy
- Single-agent chemotherapy: For early-stage (Stage I–III) and low-risk disease (WHO score <7), drugs such as methotrexate or actinomycin D may be used to destroy cancer cells.
- Combination chemotherapy: For high-risk (WHO score >7) or advanced-stage disease (Stage II–IV), multi-drug regimens are employed (e.g., EMA/CO – etoposide, methotrexate, actinomycin D, cyclophosphamide, vincristine) to provide a stronger attack on cancer cells.
Surgery
Hysterectomy: In cases where chemotherapy is ineffective or the cancer has spread extensively, removal of the uterus may be necessary to completely eliminate the tumor.
Surgery may also be considered to remove residual masses or metastases after chemotherapy.
Radiation Therapy
Radiotherapy may be used in combination with other treatments, especially in cases where the cancer has spread beyond the uterus or is resistant to chemotherapy (such as brain metastases).
Follow-Up After Treatment
After treatment, patients require regular monitoring to ensure the cancer does not return:
- Monthly hCG testing for at least one year to confirm remission.
- Routine health check-ups to detect early recurrence.
- If pregnancy occurs after treatment, a first-trimester pelvic ultrasound is recommended to verify the uterine environment and placental health, minimizing the risk of recurrence.
Lifestyle and Prevention for Choriocarcinoma (Placental Cancer)
Healthy Lifestyle Habits to Help Manage Choriocarcinoma
Regular medical follow-up: After treatment, patients should have their hCG hormone levels monitored regularly and attend periodic medical check-ups to detect early signs of recurrence.
Maintain a positive mindset: Cancer can be emotionally stressful. Practicing relaxation techniques such as yoga, meditation, or talking with family and friends can help reduce stress and improve mental well-being.
Light exercise: Moderate physical activity, such as walking or gentle yoga, helps strengthen the immune system, improve recovery, and reduce the side effects of chemotherapy.
Strictly follow your doctor’s instructions: Take prescribed medications and complete all treatment courses as directed. Stopping or altering treatment without medical advice can reduce its effectiveness.

Nutritional Recommendations
High-protein foods: Increase intake of fish, eggs, tofu, chicken, beans, and legumes to help the body heal and rebuild tissues.
Fiber-rich foods: Vegetables, fruits, and whole grains provide fiber to support digestion, reduce constipation, and help the body eliminate toxins.
Vitamins and minerals: Foods rich in vitamin C, vitamin E, and antioxidants help combat free-radical damage and strengthen the immune system.
Limit sugar and processed foods: These can increase inflammation and hinder recovery.
Stay hydrated: Drink enough water daily to maintain hydration and support detoxification, especially during chemotherapy.
Prevention of Choriocarcinoma
Although there is no absolute way to prevent choriocarcinoma, certain measures may reduce the risk:
Careful monitoring after molar pregnancy: Women who have had a molar pregnancy should undergo close follow-up with regular hCG testing after treatment to detect early signs of choriocarcinoma.
Reproductive health care: Regular gynecological check-ups are important, especially when abnormal pregnancy-related symptoms occur.
Reduce age-related risk: Women who become pregnant very young (under 20) or later in life (over 40) are at higher risk. If possible, planning pregnancy during the age range of 20–35 may reduce the risk.
Post-pregnancy complication follow-up: Women who have had miscarriages, ectopic pregnancies, or abortions should receive careful medical follow-up to prevent complications and lower the risk of cancer development.
