Thrombocytosis: Causes, Symptoms, and Possible Complications
Understanding the causes, potential risks, and preventive measures is crucial for maintaining good health and avoiding long-term damage.
What Is Thrombocytosis?
Thrombocytosis occurs when your blood contains too many platelets — the tiny cell fragments responsible for helping blood clot and stop bleeding. Under normal circumstances, platelets play a vital role in wound healing. However, when their numbers rise excessively, blood clots can form inappropriately inside blood vessels, restricting blood flow and potentially damaging vital organs.
There are two main types of thrombocytosis:
1. Primary (or Essential) Thrombocytosis – This is a rare, chronic blood disorder that originates in the bone marrow. It occurs when abnormal stem cells produce too many platelets. The exact cause remains unclear, but it is often linked to genetic mutations such as JAK2, CALR, or MPL.
2. Secondary (or Reactive) Thrombocytosis – This form is more common and develops as a response to another underlying condition such as infection, inflammation, tissue injury, trauma, surgery, iron deficiency, or certain cancers. Once the underlying trigger is resolved, platelet levels often return to normal.
Symptoms of Thrombocytosis
Most people with either primary or secondary thrombocytosis experience few or no symptoms. When symptoms do occur, they are usually related to either excessive blood clotting (thrombosis) or, paradoxically, an increased risk of bleeding.
1. Blood Clot Formation (Thrombosis)
In thrombocytosis, blood clots can form within the arteries or veins, particularly in the brain, heart, hands, or legs. These clots may block normal circulation, leading to various symptoms depending on the affected area.
Possible signs of a blood clot include:
- Confusion or difficulty speaking
- Headache or dizziness
- Seizures or fainting
- Chest pain or shortness of breath
- Abdominal pain or an enlarged spleen
- Redness, warmth, or burning sensation in the hands or feet
2. Bleeding Tendency
When platelet counts are extremely high, the platelets may become dysfunctional — paradoxically increasing the risk of bleeding rather than clotting. This happens because the body consumes a large portion of platelets in inappropriate clots, leaving fewer available to stop actual bleeding.
Common bleeding symptoms may include:
- Easy bruising
- Frequent nosebleeds
- Gum or dental bleeding
- Prolonged bleeding from minor cuts
- Blood in stool (black or red)

Possible Complications
Excessive platelets can cause blood flow obstruction in small or large vessels, leading to reduced oxygen supply to organs and tissue damage over time.
Serious complications may include:
- Stroke: Caused by a clot blocking blood flow to the brain. Symptoms may include blurred vision, sudden weakness or numbness on one side of the body, speech difficulty, loss of balance, or confusion.
- Heart attack (Myocardial infarction): When clots form in coronary arteries, patients may experience chest pain radiating to the shoulder, arm, back, or jaw, along with sweating and shortness of breath.
- Pulmonary embolism: A blood clot that travels to the lungs, leading to sharp chest pain, rapid heartbeat, or difficulty breathing.
- Budd–Chiari syndrome: A rare but serious condition caused by clotting in the veins that drain the liver, leading to abdominal pain and liver enlargement.
Less severe but still concerning complications include nosebleeds, gum bleeding, or blood-stained stools due to excessive platelet consumption.
When to Seek Medical Attention
Seek immediate medical care or call emergency services if you experience any of the following warning signs:
- Sudden chest pain radiating to the shoulder, arm, back, or jaw
- Symptoms suggestive of a stroke: facial drooping, weakness or numbness on one side, slurred speech, or blurred vision
- Uncontrolled or prolonged bleeding that does not stop

Causes of Thrombocytosis
Thrombocytosis can arise from a variety of underlying mechanisms and is generally classified into two major types — primary (essential) and secondary (reactive) — depending on whether the problem originates within the bone marrow itself or results from another medical condition.
1. Primary (Essential) Thrombocytosis
Primary thrombocytosis, also known as essential thrombocythemia, is a rare chronic blood disorder in which the bone marrow produces too many platelets without any apparent external trigger. This overproduction is usually caused by abnormalities in the stem cells responsible for blood formation.
Although the exact cause remains unknown, extensive research has identified genetic mutations as key contributors — most notably in the JAK2, CALR, or MPL genes. These mutations disrupt normal signaling pathways in bone marrow cells, causing them to divide uncontrollably and release excess platelets into circulation.
Over time, this can increase the risk of abnormal clot formation and, paradoxically, bleeding complications due to dysfunctional platelets. Primary thrombocytosis is part of a broader group of conditions known as myeloproliferative neoplasms (MPNs), which also include polycythemia vera and primary myelofibrosis.
2. Secondary (Reactive) Thrombocytosis
Secondary thrombocytosis is much more common and occurs as a temporary physiological response to another condition rather than a primary bone marrow disorder.
In these cases, platelet production increases because the body is reacting to inflammation, infection, tissue injury, or blood loss.
Common causes of reactive thrombocytosis include:
Iron-deficiency anemia or hemolytic anemia – The bone marrow compensates by producing more platelets.
Chronic inflammatory or infectious diseases – Conditions like rheumatoid arthritis, tuberculosis, or chronic infections can stimulate the release of inflammatory cytokines that boost platelet production.
Tissue damage or trauma – After injury, burns, or major surgery (especially abdominal procedures), platelet counts can rise as part of the healing response.
Splenectomy (spleen removal) – The spleen normally stores and removes old platelets from circulation. When it is surgically removed or injured, platelet counts often rise significantly.
Certain cancers – Lung, gastrointestinal, breast, ovarian, and lymphoid cancers may cause secondary thrombocytosis through the release of growth factors such as interleukin-6 (IL-6).
Kidney disease (renal failure) – Impaired kidney function can alter hormone levels, indirectly stimulating platelet production.
Medications – Some drugs, including corticosteroids and chemotherapy agents, may trigger elevated platelet counts.
Acute blood loss or recovery from alcohol overuse – The body temporarily boosts platelet formation during recovery from significant blood loss or alcohol-related bone marrow suppression.
Vitamin deficiencies – Low levels of vitamins B12 (cobalamin) or B9 (folate) can also contribute to a mild, transient rise in platelet count.
Risk Factors for Thrombocytosis
Certain factors may increase the likelihood of developing thrombocytosis or exacerbate its complications. Having one or more of these risk factors does not guarantee the disease, but it does raise the level of concern for abnormal clot formation.
Key risk factors include:
Age: Thrombocytosis is most common among adults aged 50 to 70 years, as the risk of clotting disorders increases with age.
Gender and hormonal factors: Women using oral contraceptives or hormone therapy may have a slightly higher tendency toward clot formation.
Smoking: Tobacco use damages blood vessel walls, promoting clot formation and increasing the risk of thrombosis.
History of blood clots: Individuals who have previously experienced deep vein thrombosis (DVT), pulmonary embolism, or stroke are more vulnerable to platelet-related complications.
Chronic conditions: Diseases like diabetes mellitus and hypertension accelerate blood vessel damage and raise thrombotic risk when platelet counts are high.
Inflammatory disorders: Chronic inflammation from autoimmune diseases can stimulate excess platelet production.
Understanding and managing these risk factors — through lifestyle modification, regular medical check-ups, and control of chronic diseases — plays a critical role in preventing the progression of thrombocytosis and reducing its complications.

Diagnosis and Treatment of Thrombocytosis
How Thrombocytosis Is Diagnosed
Diagnosing thrombocytosis requires a thorough evaluation to determine whether the elevated platelet count is primary (essential) or secondary (reactive) in nature. The process typically involves a detailed medical history, physical examination, and a series of laboratory and imaging tests.
During your consultation, your doctor will:
- Ask about your medical history, including any past illnesses, surgeries, or blood transfusions.
- Review all medications or supplements you are currently taking.
- Check for symptoms of bleeding (such as nosebleeds or easy bruising) or blood clots (such as leg pain, shortness of breath, or neurological issues).
To confirm the diagnosis and uncover the underlying cause, your doctor may order one or more of the following tests:
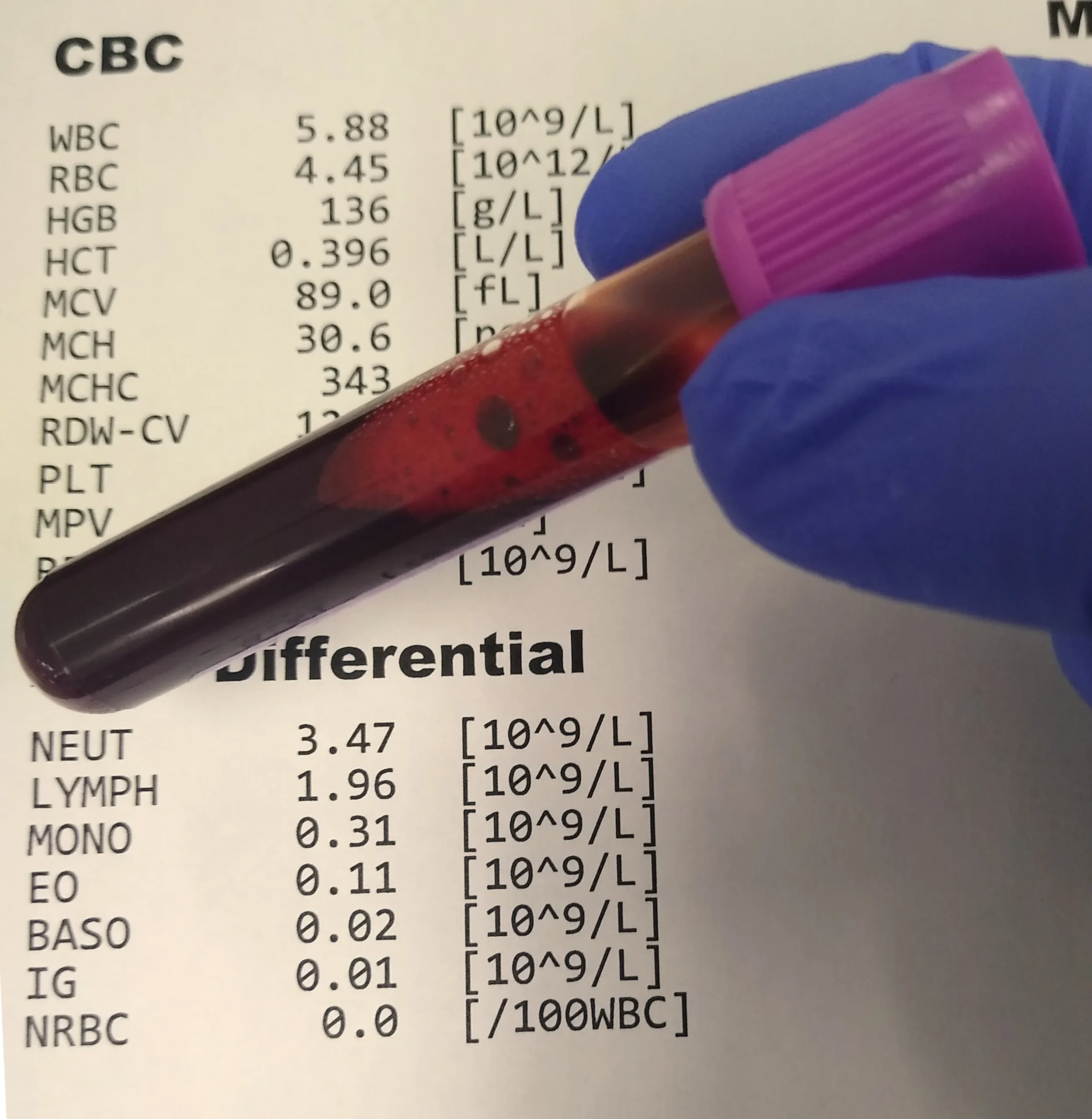
1. Complete Blood Count (CBC): This routine blood test measures the number of platelets and other blood cells. A count exceeding 450,000 platelets per microliter often suggests thrombocytosis.
2. Coagulation Tests: These tests evaluate how well your blood clots, helping to assess whether platelet function is normal or impaired.
3. Peripheral Blood Smear: A small drop of blood is examined under a microscope. In primary thrombocytosis, platelets may appear abnormal in size or shape. In secondary thrombocytosis, platelets usually look normal.
4. Bone Marrow Examination (Aspirate or Biopsy): A sample from the bone marrow may be taken to check for abnormal growth of megakaryocytes — the cells that produce platelets. This helps distinguish essential thrombocythemia from reactive causes or other bone marrow disorders.
5. Genetic and Molecular Testing: Testing for mutations in genes such as JAK2, CALR, and MPL helps confirm a diagnosis of primary thrombocytosis and rule out other myeloproliferative diseases.
6. Cancer Screening and ImagingL Since certain cancers can trigger reactive thrombocytosis, your doctor may order additional tests such as abdominal ultrasound, chest X-ray, CT scan, or MRI to look for tumors or organ abnormalities.
7. Liver and Kidney Function Tests: Assessing how well these organs are working can help identify secondary causes related to chronic diseases or inflammation.
If no secondary cause is found after comprehensive evaluation, a diagnosis of essential (primary) thrombocytosis is typically made.
Treatment of Thrombocytosis
Treatment depends on the type of thrombocytosis, the underlying cause, and whether any complications (such as clotting or bleeding) have occurred.
1. Management of Primary (Essential) Thrombocytosis
If your platelet count is high but you have no symptoms and no significant risk factors, immediate treatment may not be necessary. Instead, your doctor will likely recommend careful monitoring with regular blood tests and check-ups.
However, treatment is usually considered for patients who:
- Are over 60 years old
- Smoke or have other cardiovascular risk factors
- Have diabetes, heart disease, or hypertension
- Have a history of blood clots or bleeding episodes
Treatment options may include:
- Low-dose aspirin: Helps prevent blood clots by making platelets less sticky.
- Cytoreductive therapy (platelet-lowering medications): Drugs such as hydroxyurea, anagrelide, or interferon-alpha may be prescribed to reduce platelet production in the bone marrow.
- Plateletpheresis: In emergency situations—such as stroke or severe clotting due to extremely high platelet counts—platelets can be rapidly removed from the blood using a specialized filtering procedure.
Lifestyle adjustments such as stopping smoking, staying hydrated, and regular exercise may also help lower clotting risk.
2. Management of Secondary (Reactive) Thrombocytosis
For reactive thrombocytosis, treating the underlying cause is the primary goal. In these cases, platelet counts typically return to normal once the triggering condition improves.
For example:
- If caused by infection or inflammation, antibiotics or anti-inflammatory medications are used.
- If due to iron-deficiency anemia, iron supplementation may be recommended.
- If related to surgery, trauma, or splenectomy, platelet counts are monitored closely but usually normalize over time.
- In cancer-related cases, managing the malignancy itself will often correct the elevated platelet count.
Unlike primary thrombocytosis, antiplatelet or cytoreductive drugs are rarely needed for secondary cases.
Follow-Up and Long-Term Management
Regular follow-up is essential for anyone diagnosed with thrombocytosis. Your doctor will monitor:
- Platelet count trends
- Signs of bleeding or thrombosis
- Response to treatment and any medication side effects
Early detection and proper management greatly reduce the risk of complications such as stroke, heart attack, or deep vein thrombosis.
Lifestyle and Prevention Tips for Thrombocytosis
While thrombocytosis itself may not always cause symptoms, maintaining a healthy lifestyle can play a key role in preventing complications such as blood clots or bleeding. Good daily habits not only support your overall cardiovascular health but also help keep your blood circulation and platelet function stable.
Healthy Lifestyle Habits
If you’ve been diagnosed with thrombocytosis, it’s important to adopt certain lifestyle practices to support treatment and minimize health risks:
- Follow your doctor’s instructions closely: Take medications as prescribed, attend all follow-up appointments, and have your blood counts checked regularly.
- Exercise regularly: Engage in moderate physical activity such as walking, cycling, yoga, or swimming. These activities improve blood flow and reduce clotting risk. Avoid high-impact or contact sports that may cause injury or bleeding.
- Quit smoking: Nicotine damages blood vessels and greatly increases your risk of clot formation. Quitting is one of the most powerful steps you can take for your vascular health.
- Maintain a healthy body weight: Excess body fat contributes to inflammation, hypertension, and insulin resistance—all of which may worsen clotting tendencies.
- Stay hydrated: Drinking enough water helps maintain proper blood viscosity and reduces the risk of blood thickening.
Nutrition and Diet
A balanced diet supports healthy platelet production and circulation. In most cases, there are no strict dietary restrictions, but certain nutritional principles can be beneficial—especially if you have other risk factors such as diabetes, high blood pressure, or high cholesterol.
General dietary recommendations include:
- Eat a diet rich in vegetables, fruits, and whole grains. These foods are high in fiber and antioxidants, which help maintain healthy blood vessels.
- Choose lean proteins such as fish, tofu, beans, or skinless poultry. Fatty fish like salmon and mackerel contain omega-3 fatty acids that naturally reduce clotting risk.
- Limit saturated fats and refined sugars, particularly if you have diabetes or elevated cholesterol levels.
- Avoid excessive alcohol consumption, as heavy drinking can affect bone marrow and platelet production.
- Ensure adequate intake of iron, vitamin B12, and folate. Deficiencies in these nutrients can alter blood cell production and mimic or worsen platelet abnormalities.
If you have specific health conditions—such as diabetes, hypertension, or high cholesterol—your doctor or dietitian can design a tailored meal plan to reduce cardiovascular risk and maintain healthy blood parameters.
Prevention of Thrombocytosis and Its Complications
Currently, there are no proven methods to prevent primary (essential) thrombocytosis, since it is primarily linked to genetic mutations and bone marrow dysfunction.
However, you can significantly reduce the risk of complications and secondary (reactive) thrombocytosis through proactive health management and lifestyle choices.
Effective preventive measures include:
Control blood pressure, cholesterol, and blood sugar levels: Keeping these within normal ranges helps prevent damage to blood vessels and lowers the risk of thrombosis.
Exercise consistently: Regular moderate activity supports circulation and heart health. Aim for at least 150 minutes of exercise per week.
Adopt a heart-healthy diet: Focus on whole grains, fresh fruits, vegetables, legumes, and healthy fats (olive oil, nuts, avocados).
Avoid tobacco: Smoking cessation drastically lowers your risk of clot formation and cardiovascular complications.
Inform your doctor about any planned surgery or procedures: Your physician may adjust medications or monitor platelet counts more closely to prevent excessive clotting or bleeding during recovery.
Review medications regularly: Some drugs can raise platelet levels or affect clotting. Always consult your healthcare provider before starting new medications or supplements.
