Can Immune Thrombocytopenia Be Cured?
Immune thrombocytopenia (ITP) is a rare blood disorder in which the immune system mistakenly targets and destroys the body’s own platelets—cells essential for normal blood clotting. As a result, affected individuals may bruise easily, bleed excessively from minor injuries, or even develop spontaneous bleeding without a clear cause.
In some cases, ITP may resolve spontaneously, particularly in children. However, for many adults, it tends to become a chronic condition requiring long-term management rather than a one-time treatment. Therapies focus on controlling bleeding, maintaining a safe platelet count, and preventing life-threatening complications rather than providing a permanent cure.
Understanding Immune Thrombocytopenia (ITP)
What Is ITP?
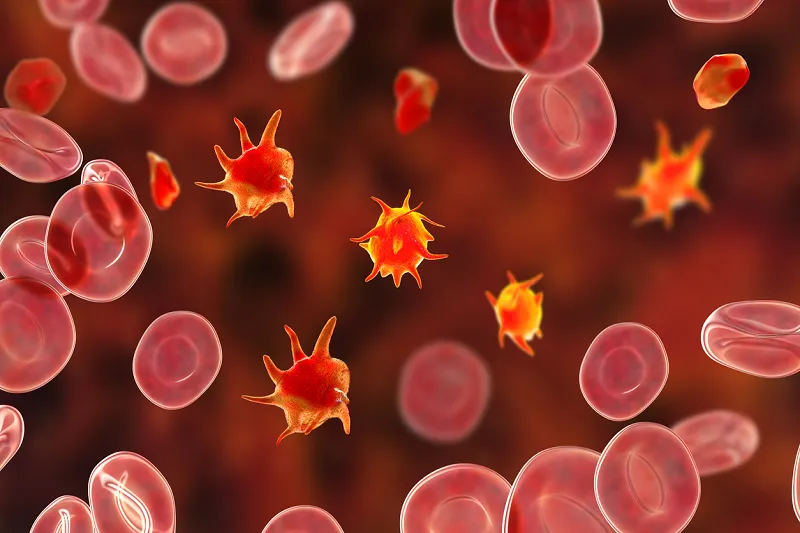
Platelets are small, disc-shaped cells produced in the bone marrow that help stop bleeding by forming clots at sites of injury. When platelet numbers fall below normal levels, the blood cannot clot effectively, leading to prolonged or spontaneous bleeding episodes.
In immune thrombocytopenia, the immune system generates antibodies that attach to platelets, marking them for destruction—primarily in the spleen. These same immune responses can also suppress platelet production from megakaryocytes in the bone marrow. As a result, the blood fails to clot properly due to the reduced platelet count.
Types of ITP
ITP can occur in both children and adults and is generally classified in two major forms:
- Primary ITP: Occurs when the immune system itself is the underlying cause, without any associated condition. This form accounts for roughly 80% of all ITP cases and is considered an autoimmune disease.
- Secondary ITP: Develops as a result of another disorder—such as chronic infections (e.g., HIV, hepatitis C), autoimmune diseases (like lupus), or hematologic cancers.
Classification by Disease Course
Clinicians further categorize ITP based on its duration and clinical progression:
- Acute ITP: Platelet levels return to normal (above 150,000/mm³) within 3 months and do not relapse.
- Persistent ITP: The condition fails to achieve complete remission or relapses within 3–12 months after diagnosis.
- Chronic ITP: Platelet deficiency persists beyond 12 months, often requiring ongoing monitoring or treatment.
Symptoms of Immune Thrombocytopenia
Because platelets play a vital role in blood clotting, symptoms of ITP are primarily related to bleeding tendencies. The severity varies widely between individuals—from mild skin bruising to life-threatening hemorrhages. Common signs and symptoms include:
- Skin bleeding (petechiae or purpura): Small red or purple spots, patches, or larger bruises that appear spontaneously and may change color over time (from red to blue to yellow).
- Mucosal bleeding: Such as nosebleeds, bleeding gums, or eye hemorrhages.
- Hematuria: Blood in the urine.
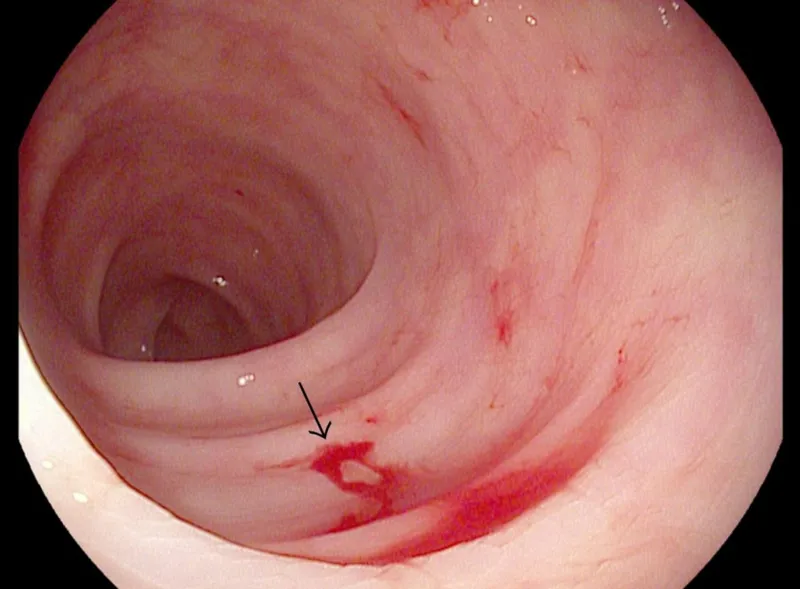
- Internal bleeding: In severe cases, bleeding may occur in vital organs, such as the gastrointestinal tract (vomiting blood, black tarry stools), uterus (prolonged menstrual bleeding), or rarely the brain and meninges—events that can be life-threatening emergencies.

Because ITP symptoms can resemble those of other medical conditions (such as leukemia, aplastic anemia, or viral infections), proper diagnosis always requires professional medical evaluation and blood testing.
Possible Complications of ITP
While many individuals manage ITP successfully, the condition can occasionally lead to serious complications, especially if left untreated or poorly controlled:
- Recurrent bleeding from the nose, gums, or urinary tract.
- Prolonged or heavy menstrual bleeding (menorrhagia lasting longer than 7 days).
- Gastrointestinal or intracranial hemorrhage.
- Paradoxical blood clots (thrombosis) — though rare, certain treatments such as corticosteroids or thrombopoietin receptor agonists can increase clotting risk.
- Bone marrow or blood cancers, which may coexist with or mimic ITP.
- Bone marrow suppression due to prolonged use of immunosuppressive drugs.
- Cardiovascular complications such as myocardial ischemia due to altered blood viscosity.
- Pregnancy-related risks: Women with ITP may face excessive bleeding during delivery. Although ITP rarely harms the baby, newborn platelet counts should be checked immediately after birth.
When to See a Doctor
You should seek medical attention promptly if you experience unusual symptoms or notice any changes in your health. Specifically, contact your healthcare provider if:
- You develop new or worsening symptoms such as unexplained bruising, bleeding gums, nosebleeds, or blood in urine or stool.
- You already have a diagnosis of immune thrombocytopenia and, despite regular monitoring, begin to experience new signs of bleeding or fatigue.
- Your symptoms interfere with daily life — for example, persistent bleeding, prolonged menstrual periods, or severe tiredness.
- You notice sudden neurological changes, such as severe headache, confusion, or visual disturbances, which may indicate internal bleeding.
⚠️ Important Medical Warning: Never ignore new or worsening bleeding symptoms, especially if they occur suddenly or without trauma. Early diagnosis and prompt treatment can prevent serious complications such as intracranial hemorrhage, gastrointestinal bleeding, or life-threatening anemia. Regular follow-up with a hematologist is essential for individuals diagnosed with ITP.
Causes of Immune Thrombocytopenia
What Causes ITP?
Immune thrombocytopenia results from an abnormal immune response in which the body mistakenly produces antibodies that attack its own platelets. While the precise trigger remains unclear, it is understood that immune dysregulation—often influenced by infections, autoimmune diseases, or certain medications—plays a central role.
In most adults, ITP develops without a clearly identifiable cause and is classified as primary ITP. However, in other cases, it may arise secondary to an underlying condition or external factor.
Secondary Causes and Triggers
Secondary ITP can be associated with several medical conditions and external triggers, including:
- Viral infections: Chickenpox (varicella), hepatitis C, Epstein–Barr virus, parvovirus B19, and HIV are all known to trigger immune-mediated platelet destruction.
- Autoimmune diseases: Particularly systemic lupus erythematosus (SLE), which frequently coexists with ITP.
- Chronic lymphocytic leukemia (CLL): Malignant immune cells may disrupt normal platelet regulation.
- Drug-induced ITP: Certain medications can trigger an immune reaction against platelets.
- Severe bacterial infections (sepsis): May lead to secondary immune thrombocytopenia or platelet consumption.
Medications Linked to ITP
Several drug classes have been associated with immune-mediated platelet reduction, including:
- Medications for heart disease, infections, or seizure disorders.
- Heparin, a common anticoagulant used to prevent or treat blood clots. (Heparin-induced thrombocytopenia, or HIT, is a distinct but serious immune reaction requiring immediate attention.)
- Certain chemotherapy or radiation therapies that suppress bone marrow function.
Other Medical Triggers
Some medical procedures and conditions have also been reported to contribute to ITP development, such as:
- Cardiac bypass surgery, which can alter immune activation pathways.
- Radiation therapy involving the bone marrow, which may impair platelet production.
Risk Factors for Immune Thrombocytopenia
Who Is at Risk?
In the United States, approximately 30,000 new cases of ITP are diagnosed each year. About 70% of adult patients are women, and most are younger than 40 years at the time of diagnosis. In contrast, ITP in children is often acute and self-limiting, typically developing after a viral infection and resolving within months. Both boys and girls are affected equally in pediatric cases.
Factors That Increase Risk
Several factors are known to raise the likelihood of developing ITP:
- Gender: Women, particularly those of childbearing age, are more commonly affected.
- Autoimmune background: People with other autoimmune disorders—such as rheumatoid arthritis or lupus—have an elevated risk.
- Recent viral infection: Especially in children or young adults.
- Genetic predisposition: Although rare, certain HLA gene variants have been linked to immune dysregulation leading to platelet destruction.
- Medication exposure: Prior use of heparin or immunomodulatory drugs may increase vulnerability.
Diagnosis and Treatment of Immune Thrombocytopenia (ITP)
Diagnostic Evaluation
Diagnosing immune thrombocytopenia requires a comprehensive clinical assessment and laboratory testing to exclude other potential causes of low platelet counts. Because ITP is essentially a diagnosis of exclusion, doctors must first rule out secondary thrombocytopenia due to infection, bone marrow disease, or medication effects.
Key diagnostic tests include:
- Complete blood count (CBC): Reveals low platelet levels with otherwise normal white and red blood cells.
- Peripheral blood smear: Helps rule out clumping, abnormal cell morphology, or other hematologic disorders.
- Bone marrow aspiration/biopsy: Considered essential in uncertain cases or when patients fail to respond to initial therapy. It typically shows normal or increased megakaryocytes (the cells that produce platelets).
Additional tests may be ordered to identify underlying causes or associated conditions:
- Viral studies: Anti-HCV, HBsAg, anti-HIV, and serologic testing for Helicobacter pylori.
- Autoimmune screening: ANA, anti-dsDNA, LE cell, thyroid antibodies (TSH, FT3, FT4), and direct or indirect anti-platelet antibodies.
- Hemolysis and anemia evaluation (if applicable): Serum iron, ferritin, reticulocyte count, haptoglobin, bilirubin, LDH, and Coombs test.
Treatment Approaches for Immune Thrombocytopenia
The treatment of ITP depends on disease severity, bleeding risk, platelet count, and the patient’s overall health. Some mild cases, especially in children, resolve spontaneously without intervention, while others require long-term therapy to maintain safe platelet levels.
1. Observation and Monitoring
Patients with mild symptoms—such as only minor bruising or petechiae and platelet counts above 50,000/mm³—may not need immediate treatment. Instead, they are closely monitored for any signs of bleeding progression.
Regular follow-up visits and repeated CBC testing help physicians decide when to initiate therapy.
2. Emergency Management
Emergency treatment is required if platelet counts drop below 10,000/mm³ or if the patient develops serious bleeding (e.g., intracranial or gastrointestinal hemorrhage).
Common emergency therapies include:
- Intravenous immunoglobulin (IVIG) or high-dose methylprednisolone to rapidly suppress immune destruction of platelets.
- Platelet transfusion may be used temporarily to control active bleeding, though its effect is often short-lived.
3. First-Line Therapy (Acute Phase)
The mainstay of treatment for acute ITP is corticosteroids, which help reduce immune-mediated platelet destruction:
- Prednisone is typically prescribed for 2–4 weeks, then gradually tapered once platelet counts recover.
- Dexamethasone may be used as an alternative in short, high-dose cycles.
4. Relapse or Refractory Cases
If symptoms return after initial recovery, treatment generally mirrors the acute-phase regimen. In life-threatening relapse, patients may again require IVIG or pulse corticosteroid therapy.
5. Chronic, Steroid-Resistant, or Dependent Cases
For patients who either fail to respond to corticosteroids or relapse repeatedly, several second-line treatments are available:
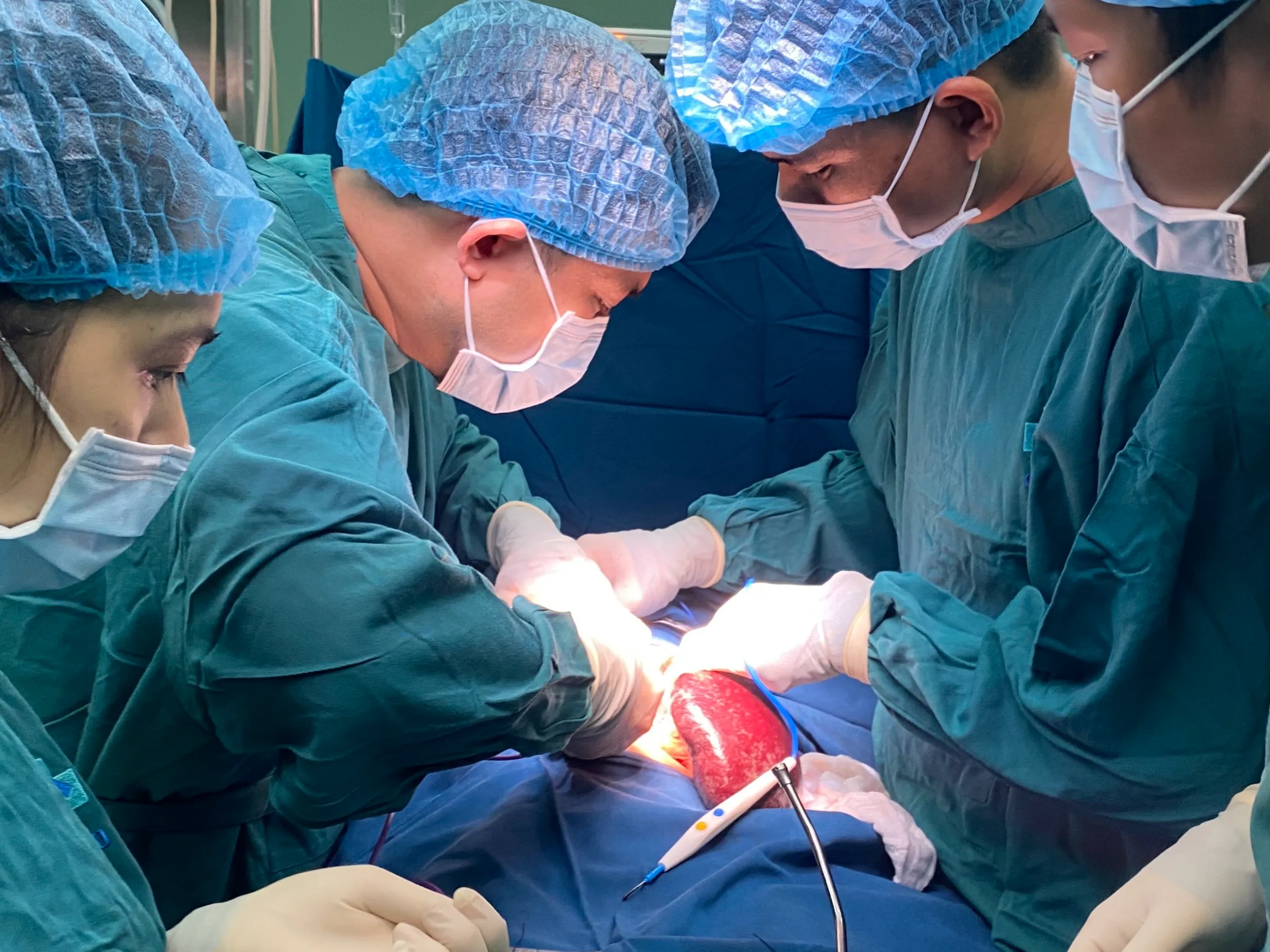
- Splenectomy: The spleen is the primary site of platelet destruction. Removing it often leads to a rapid and lasting response in 60–70% of patients. Laparoscopic splenectomy is preferred due to lower surgical risks (~0.2% complication rate).
- Rituximab: A monoclonal antibody that targets B cells, thereby reducing the production of anti-platelet antibodies. It offers a non-surgical option for patients unsuitable for splenectomy.
- Thrombopoietin receptor agonists (TPO-RAs): Such as eltrombopag and romiplostim, which stimulate platelet production in chronic ITP.
Prognosis:
- In children, the outlook is excellent—around 80% recover fully, and only 20% develop chronic disease. Severe bleeding is rare.
- In adults, up to 80% progress to chronic ITP, with a 1–5% risk of intracranial hemorrhage, emphasizing the need for consistent monitoring and individualized therapy.
Lifestyle and Prevention Tips for ITP
Daily Habits and Self-Care
Although there is currently no definitive way to prevent ITP, patients can adopt healthy lifestyle practices to reduce complications and support treatment outcomes:
- Follow your doctor’s instructions carefully and attend all scheduled follow-up appointments.
- Report new symptoms such as unexpected bleeding, fatigue, or dizziness immediately.
- When platelet counts are below 50,000/mm³, avoid activities with a risk of injury or bleeding (e.g., climbing, cycling, contact sports).
- When platelets exceed 50,000/mm³, light exercise such as walking, yoga, or gentle stretching is encouraged—but avoid high-impact sports like boxing, football, or basketball.
- Avoid medications that impair platelet function, including aspirin, ibuprofen, naproxen, and warfarin, unless explicitly approved by your doctor.
- Patients who have undergone splenectomy should watch for signs of infection and may require preventive antibiotics.
- Avoid alcohol, smoking, and recreational drugs, which can worsen platelet suppression or interfere with treatment.
Nutrition for People with ITP
A balanced diet supports immune regulation and overall health.
Recommended dietary habits include:
- Eating foods rich in antioxidants and vitamins: colorful fruits and vegetables such as berries, cherries, tomatoes, pumpkin, and bell peppers.
- Reducing salt, sugar, and saturated fats to maintain healthy weight and cardiovascular function.
- Avoiding raw or undercooked foods to reduce infection risk, especially in immunosuppressed patients.
- Drinking boiled or filtered water and maintaining proper food hygiene.
Preventive Measures and Health Maintenance
Although ITP cannot be fully prevented, you can minimize risks and complications by:
- Getting regular health checkups and blood tests to detect abnormalities early.
- Adhering to prescribed treatments and avoiding self-medication.
- Maintaining a healthy body weight and engaging in safe, regular physical activity.
- Following a nutritious and hygienic diet to strengthen immune function.
