Hemolytic Anemia: Causes, Symptoms, and Treatment Options
Blood is a vital fluid that sustains every organ in the human body. It consists of two main components — blood cells and plasma. Among the three primary blood cell types (red blood cells, white blood cells, and platelets), red blood cells (RBCs) play the essential role of transporting oxygen.
Hemolytic anemia occurs when red blood cells are destroyed (a process called hemolysis) faster than the bone marrow can replace them. Normally, an RBC lives about 120 days in circulation, but in hemolytic anemia, this lifespan is dramatically shortened.
The treatment plan varies for each individual, depending on the underlying cause, disease severity, and overall health status. Early diagnosis is crucial to prevent serious complications.
Understanding Hemolytic Anemia
What is hemolytic anemia?
Anemia is generally defined as a condition in which the blood has a lower-than-normal amount of hemoglobin — the oxygen-carrying protein inside RBCs — leading to reduced oxygen delivery to tissues and organs.
Hemolytic anemia specifically refers to a group of disorders in which RBCs are prematurely destroyed and removed from the bloodstream before their normal lifespan ends. The body responds by producing more red cells in the bone marrow, but in many cases, production cannot keep up with the rate of destruction.
Hemolytic anemia may develop suddenly (acute) or progress gradually (chronic). It can range from mild and symptom-free to life-threatening, depending on the cause.
Symptoms of Hemolytic Anemia
Symptoms vary widely from person to person and depend on how rapidly the red blood cells are being destroyed. Some individuals experience only mild fatigue, while others develop severe, acute symptoms.
Common signs and symptoms include:
- Anemia-related symptoms: Fatigue, dizziness, shortness of breath (especially on exertion), pale or yellowish skin, and heart palpitations.
- Hemolysis-related signs: Jaundice (yellowing of the skin and eyes), dark-colored urine, and in acute episodes, red or tea-colored urine due to free hemoglobin. Fever and chills may occur in severe cases.
- Enlargement of organs: The liver (hepatomegaly) and spleen (splenomegaly) may become enlarged as they filter out the damaged red cells.
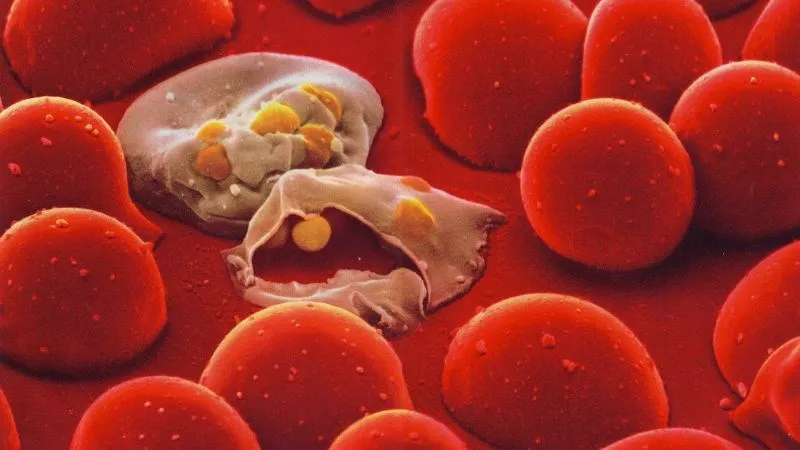
- Symptoms related to the underlying cause: For example, patients with malaria may experience cyclical chills and fever, while those with inherited disorders may show skeletal deformities or delayed growth.

Possible Complications
If left untreated or poorly controlled, hemolytic anemia can lead to serious health issues, including:
- Acute hemolytic crisis: A sudden destruction of large numbers of RBCs, leading to severe anemia, organ oxygen deprivation, and potential failure of vital organs like the heart, brain, or kidneys.
- Heart failure: The heart must pump harder to compensate for the reduced oxygen-carrying capacity of the blood. Over time, this strain can weaken the heart muscle and cause chest pain or heart failure.
- Kidney damage: Free hemoglobin released from destroyed red cells can accumulate and damage kidney tissues, eventually leading to chronic kidney disease.
- Chronic fatigue and reduced quality of life: Persistent anemia reduces physical endurance and concentration, impairing both work performance and daily activities.
When to See a Doctor
You should consult a doctor immediately if you experience:
- Any unexplained fatigue, jaundice, or dark urine
- Shortness of breath, palpitations, or chest discomfort
- Worsening of previously stable anemia symptoms
- If you have been diagnosed with immune thrombocytopenia (ITP) or another blood disorder and develop new or unusual symptoms
- Any signs that interfere with your ability to function or perform daily activities
Causes and Risk Factors of Hemolytic Anemia
Hemolytic anemia can arise from a wide range of underlying mechanisms, but all share one common feature — premature destruction of red blood cells.
Clinically, hemolytic anemia is broadly divided into two main categories based on its origin: inherited (genetic) and acquired (developed later in life). Understanding the distinction between these two forms is crucial for accurate diagnosis and treatment.
1. Inherited Hemolytic Anemia
Inherited hemolytic anemias result from defects in the red blood cells themselves, usually caused by mutations in one or more genes that control their structure or metabolism. These defects weaken the RBC membrane, alter hemoglobin structure, or disrupt enzyme activity — all of which make the cells more fragile and prone to destruction.
Common inherited forms include:
Sickle Cell Disease (Sickle Cell Anemia): A genetic disorder in which abnormal hemoglobin (HbS) causes red blood cells to take on a rigid, sickle-like shape. These cells break down easily and block small blood vessels, leading to pain crises and organ damage.
Thalassemia: A group of inherited conditions characterized by abnormal hemoglobin production. The imbalance of hemoglobin chains results in fragile, short-lived RBCs and varying degrees of anemia.
Red Blood Cell Membrane Disorders. Structural abnormalities of the RBC membrane, including:
- Hereditary spherocytosis
- Hereditary elliptocytosis
- Hereditary pyropoikilocytosis
- Hereditary stomatocytosis (exocytosis disorder)
These defects alter the shape and flexibility of red cells, leading to their early destruction in the spleen.
Enzyme Deficiencies: RBCs rely on enzymes to maintain membrane integrity and protect against oxidative damage. Two important enzyme deficiencies include:
- Pyruvate kinase deficiency (PKD) – leads to reduced energy (ATP) production in RBCs.
- Glucose-6-phosphate dehydrogenase (G6PD) deficiency) – makes cells highly sensitive to oxidative stress, which can trigger hemolysis after certain foods (like fava beans) or medications.

2. Acquired Hemolytic Anemia
In contrast to inherited types, acquired hemolytic anemia develops due to external factors that damage otherwise normal red blood cells. The destruction may occur inside the bloodstream (intravascular) or in the spleen and liver (extravascular).
Common causes include:
Autoimmune Hemolytic Anemia (AIHA): The immune system mistakenly produces antibodies that attack the body’s own RBCs. This can occur in autoimmune diseases such as lupus, rheumatoid arthritis, or ulcerative colitis.
Drug-Induced Hemolytic Anemia: Certain medications can trigger immune-mediated destruction of red cells. Examples include:
- Quinidine
- Penicillin
- Methyldopa
- Ticlopidine
- Clopidogrel
Mechanical Hemolysis: Physical trauma can rupture red cells — for example, in patients with mechanical heart valves, vascular malformations, or after severe burns.
Hypersplenism (Overactive Spleen): An enlarged or overactive spleen may destroy healthy RBCs faster than normal, leading to anemia and low platelet counts.
Bone Marrow Disorders and Blood Cancers: Conditions like leukemia, lymphoma, or bone marrow failure can impair RBC production and increase their fragility.
Transfusion Reactions: When incompatible blood is transfused, the recipient’s immune system attacks the donor RBCs, causing rapid hemolysis — a medical emergency that can lead to shock or kidney failure.
Paroxysmal Nocturnal Hemoglobinuria (PNH): A rare acquired genetic defect of blood-forming stem cells that causes chronic intravascular hemolysis, especially during the night.
Infections and Toxins
- Malaria and Babesiosis (parasite infections) directly invade and destroy red blood cells.
- Heavy metal poisoning, such as lead or copper exposure, can also cause hemolysis.
Who Is at Risk of Hemolytic Anemia?
While anyone can develop hemolytic anemia, certain individuals face a higher risk. These include:
- Newborns with maternal-fetal blood group incompatibility (such as Rh or ABO incompatibility)
- Patients who have undergone organ or bone marrow transplantation
- People with artificial heart valves or vascular malformations
- Individuals exposed to toxic chemicals or radiation
- Those with autoimmune diseases, malignant conditions, or parasitic infections
Factors That Increase the Likelihood of Developing Hemolytic Anemia
As mentioned above, hemolytic anemia can occur at any age and in any gender. The likelihood increases in the presence of:
- Family history of genetic blood disorders
- Autoimmune diseases that trigger immune-mediated RBC destruction
- Use of certain medications that can induce hemolysis
- Exposure to infections or toxins that damage red blood cells
- Underlying bone marrow or metabolic disorders
Diagnosis and Treatment of Hemolytic Anemia
Diagnostic Methods for Hemolytic Anemia
Patients suspected of having hemolytic anemia may undergo various laboratory tests to support diagnosis. In addition to a complete blood count (CBC), the following tests may be performed:
- Coombs test (Direct Antiglobulin Test): Detects autoimmune hemolytic anemia.
- Reticulocyte count: Evaluates bone marrow response and red blood cell production.
- Haptoglobin test: Low haptoglobin levels may indicate red blood cell destruction.
- Lactate dehydrogenase (LDH) and bilirubin tests: Elevated levels suggest hemolysis.
- Peripheral blood smear: Assesses the shape and size of red blood cells.
- Hemoglobin electrophoresis: Identifies abnormal hemoglobin variants.
In some cases, additional tests may be recommended to determine the underlying cause of hemolytic anemia more precisely.
Treatment Options for Hemolytic Anemia
Patients with mild hemolytic anemia may only require regular monitoring without active treatment. However, individuals with more severe conditions need appropriate medical interventions. Common treatment options include:
- Blood transfusion for severe anemia.
- Corticosteroids to reduce inflammation and immune-mediated hemolysis.
- Intravenous immunoglobulin (IVIG) therapy to strengthen the immune system.
- Rituximab as an immunotherapy option in certain cases.
- Splenectomy (surgical removal of the spleen) to reduce red blood cell destruction.
- Immunosuppressive therapy to limit immune system attacks on red blood cells.
Lifestyle and Prevention of Hemolytic Anemia
Healthy Habits to Manage Hemolytic Anemia
If you are diagnosed with hemolytic anemia, maintaining healthy lifestyle habits can help slow disease progression. Recommended measures include:
- Follow your doctor’s treatment plan closely.
- Report any unusual symptoms to your healthcare provider.
- Avoid exposure to cold environments; wear warm clothing to maintain body temperature.
- Protect yourself from infections by avoiding contact with sick individuals, washing hands regularly, and consuming well-cooked food and boiled water.
- Monitor for signs of infection, especially after splenectomy surgery.
- Avoid alcohol, tobacco, and stimulants.
Nutrition Guidelines
A healthy, balanced diet plays an important role in supporting your recovery:
- Eat plenty of antioxidant-rich foods such as fruits and vegetables — blueberries, cherries, tomatoes, squash, and bell peppers.
- Avoid alcohol, smoking, and excessive caffeine.
- Reduce salt, sugar, and fatty foods, and maintain a healthy weight.
- Consume well-cooked food and avoid raw vegetables to prevent infection.
Preventive Measures for Hemolytic Anemia
To lower the risk of developing hemolytic anemia, consider the following preventive strategies:
- Regular health check-ups for early detection.
- Newborn screening to identify genetic conditions that may cause hemolytic anemia.
- Adhere to prescribed treatments and medical advice.
- Exercise regularly and maintain a healthy body weight.
- Eat a nutritious, hygienic diet to prevent infections.
- Ensure children receive full vaccinations according to the national immunization schedule.

