Skin Allergies: A Common Skin Condition You Should Know About
Understanding Skin Allergies
What Is a Skin Allergy?
A skin allergy occurs when your immune system overreacts to substances it perceives as harmful — called allergens. These can range from environmental triggers and medications to infections or even your own immune responses.
When the immune system releases histamine and other inflammatory chemicals in reaction to contact with an allergen, it causes redness, itching, and rashes — hallmark signs of an allergic skin reaction.
💡 Tip: Not all rashes are allergic. Conditions like eczema, psoriasis, or fungal infections can look similar. Always consult a dermatologist for proper diagnosis.
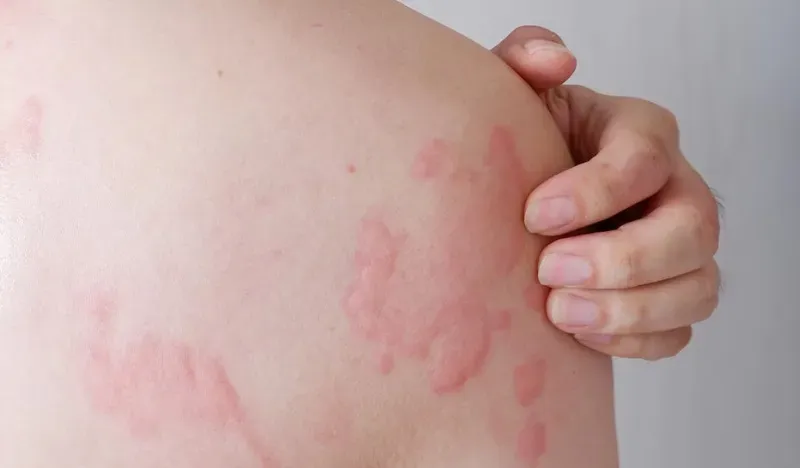
Symptoms of Skin Allergy
Common Signs and Symptoms
Typical skin allergy manifestations include:
- Redness and rash
- Itching or burning sensation
- Swelling
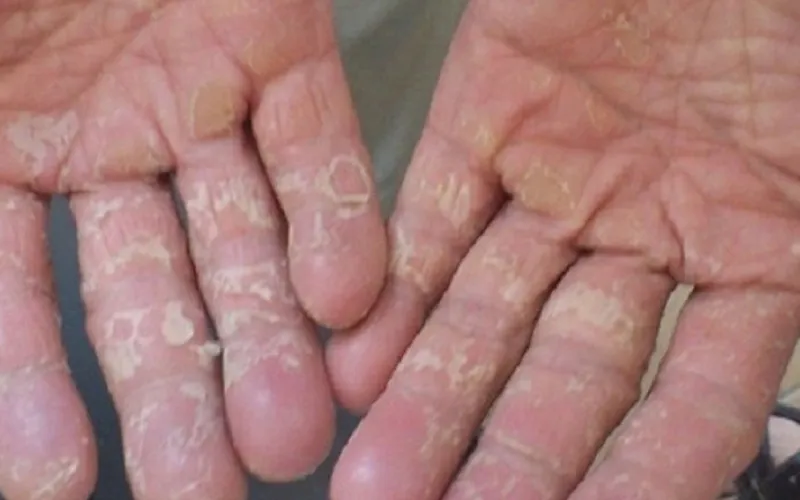
- Peeling or scaling
- Cracked or dry skin
In allergic contact dermatitis (ACD), the main symptom is intense itching, while pain may result from broken skin or infection. Visible changes range from mild redness and tiny blisters to large swollen areas or even oozing lesions.
Rashes often appear in patterns that reveal the source of exposure — for instance:
- Linear streaks on arms or legs (from brushing against poison ivy)
- Redness around the eyes or wrists (from cosmetic products or watch straps)
Hands are the most commonly affected area since they frequently come in contact with allergens. Airborne allergens, such as perfume sprays or cleaning products, typically affect exposed areas like the face and neck.
Symptoms usually develop within 24–48 hours after exposure but may persist or worsen with repeated contact.
When to See a Doctor
It can be challenging to pinpoint the exact cause of a skin allergy, as patch testing only identifies substances you’re sensitive to — not when or where contact occurred.
If you experience persistent itching, swelling, or rash that doesn’t improve with over-the-counter creams, you should seek medical advice. Early diagnosis helps reduce complications and speed up recovery.
Causes of Skin Allergies
Common Triggers Include:
- Nickel: Found in jewelry, jean buttons, cosmetics, and soaps
- Sunscreens and insect repellents
- Topical medications such as antibiotic or anti-itch creams
- Perfumes and fragrances
- Household detergents and cleaning agents
- Plants, including poison ivy and pollen
- Pet dander
- Certain foods (e.g., peanuts, shellfish, milk, eggs)
- Insect bites or stings
- Rubber or latex, commonly found in gloves, balloons, and elastic clothing
- Chemical compounds used in industrial or cosmetic products
You’re more likely to develop allergic skin conditions if you already have eczema (atopic dermatitis), poor blood circulation, recurrent genital itching, or frequent exposure to moist environments like swimming pools.
Risk Factors for Skin Allergy
Who Is at Risk?
- Individuals with a family history of allergic diseases
- People frequently exposed to chemical irritants at work or home
Factors That Increase Risk
- Certain foods (e.g., nuts, milk, seafood)
- Sudden weather changes
- Pet hair or fur
- Medications
- Chemical substances
- Mold or damp environments
- Insect bites or stings
Diagnosis and Treatment of Skin Allergies
How Skin Allergies Are Diagnosed
Clinical Evaluation and Testing
In most cases, contact dermatitis can be diagnosed through a detailed clinical examination and patient history. Doctors often consider various aspects such as the patient’s occupation, hobbies, household chores, travel habits, clothing materials, use of topical medications or cosmetics, and even spousal or family activities that might involve shared allergens.
A useful diagnostic step is the “use test,” in which the suspected allergen (for example, a perfume or shampoo) is applied to an unaffected area of the skin — usually the forearm — to observe whether a reaction occurs. This simple method helps confirm whether a product is responsible for the allergy.
When allergic contact dermatitis (ACD) is suspected but not clearly identified, a patch test is recommended. In this test, small patches containing trace amounts of various allergens are applied to the upper back using adhesive discs or chambers (such as Finn Chambers).
A modern version of this procedure, the Thin-layer Rapid Use Epicutaneous Test (TRUE TEST®), uses preloaded panels containing the most common contact allergens. These can be applied and interpreted by any trained healthcare provider. The skin beneath the patches is evaluated at 48 and 96 hours after application for visible reactions.
Interpreting Results
A false positive may occur when a substance causes irritation rather than a true allergic reaction, or when cross-reactivity happens between related allergens. Conversely, a false negative can occur if the tested allergens do not include the true trigger or if the allergic site was not properly represented.
Accurate diagnosis therefore requires correlating the test results with the patient’s exposure history and clinical findings.
Effective Treatments for Skin Allergies
When an allergic reaction occurs, the goal is to relieve symptoms, prevent infection, and restore the skin barrier.
Avoid scratching, even though the itching can be intense, as this may worsen inflammation or lead to infection.
Home Remedies and Over-the-Counter (OTC) Options
You can try several home and OTC treatments to ease discomfort:
- Hydrocortisone cream (1%) to reduce inflammation
- Calamine lotion to soothe itching and dry oozing blisters
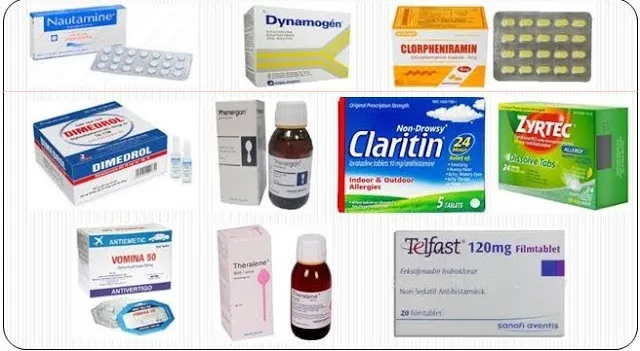
- Oral antihistamines (such as cetirizine, loratadine, or diphenhydramine)
- Cool compresses or cold baths
- Oatmeal baths to relieve irritation
Prescription Treatments
If symptoms persist, your doctor may prescribe stronger medications:
- Topical corticosteroids of medium to high potency (e.g., triamcinolone 0.1% ointment or betamethasone valerate 0.1% cream) for mild to moderate ACD
- Oral corticosteroids (e.g., prednisone 60 mg daily for 7–14 days) in cases with severe or widespread blistering
- Systemic antihistamines (e.g., hydroxyzine or diphenhydramine) to reduce itching and improve sleep
- Wet-to-dry dressings with saline or Burow’s solution to soothe and dry oozing areas
Combination therapy — such as topical steroids, antihistamines, and barrier-repair emollients — often provides the best results.
Lifestyle and Prevention for Skin Allergies
Healthy Habits for Managing Skin Allergies
Following your doctor’s instructions is key to effective recovery.
In most cases, allergic skin reactions gradually subside, but symptom control and prevention of recurrence are essential.
You can manage your condition better by:
- Wearing loose, breathable clothing
- Applying cool compresses or taking cool showers
- Using calamine lotion and hydrocortisone cream for mild irritation
- Avoiding direct sunlight or UV exposure if your skin is inflamed or sensitive
- Reporting any abnormal reactions to your doctor during treatment
Regular medical checkups help monitor disease progression and allow your doctor to adjust treatment when necessary.
Psychological well-being also plays a major role in recovery — staying positive, sharing your feelings with family, or engaging in relaxing hobbies such as reading or caring for pets can greatly reduce stress-related flare-ups.
Preventing Skin Allergies
To minimize flare-ups and prevent recurrence, consider these preventive strategies:
- Avoid known allergens or substances that previously caused irritation
- Use protective gloves when handling chemicals or detergents
- Practice supportive care such as cold compresses and antihistamines
- Apply corticosteroids (topical or oral as prescribed) to control inflammation
- Avoid sunlight exposure if you have photoallergic contact dermatitis
- Moisturize daily to keep the skin barrier strong and resilient
