What Is Scleroderma? Early Detection for Better Disease Management
Scleroderma is an autoimmune disorder in which the body produces excessive amounts of collagen — the protein responsible for skin strength and elasticity. In this condition, the immune system mistakenly attacks healthy cells and tissues, leading to inflammation and damage in various organs.
The disease can manifest differently from one person to another, depending on the extent and location of tissue involvement. If left untreated, scleroderma can progress to life-threatening complications affecting the lungs, heart, or kidneys.
Overview of Scleroderma
Definition
Scleroderma (from Greek: “skleros” meaning “hard” and “derma” meaning “skin”) is a chronic autoimmune connective tissue disease characterized by the thickening and hardening of the skin and underlying tissues. Although rare, it can have a significant impact on quality of life and, in systemic forms, threaten survival.
Excessive collagen production leads to fibrosis — a process where normal tissue is replaced by dense, rigid connective tissue. This causes the skin to become tight, shiny, and less flexible, and may also involve internal organs such as the lungs, heart, and gastrointestinal tract.
There are two main clinical types of scleroderma: localized and systemic.
Types of Scleroderma
1. Localized Scleroderma
This form affects only the skin and sometimes the tissues underneath it, such as fat, muscle, or bone. It is more common in children and generally does not spread to internal organs.
- Morphea: Appears as one or several oval, waxy patches that start out red or purple, later becoming thick and pale with a surrounding reddish border. These patches may cause itching or discoloration but often resolve slowly over time.
- Linear scleroderma: Characterized by thickened bands of skin, usually appearing on the face or limbs. In children, it can interfere with bone growth and joint movement if not treated early.
2. Systemic Scleroderma (Systemic Sclerosis)
This is the more severe form of the disease, as it can affect internal organs in addition to the skin. Depending on which organs are involved, patients may experience a range of symptoms and complications.

Common Signs and Symptoms
Scleroderma can develop gradually and sometimes goes unnoticed in its early stages. Common symptoms include:
- Hard, shiny skin, especially on the hands, face, or around joints
- Numbness or tingling sensations
- Stiffness and pain in the fingers
- Fatigue and weakness
Skin Manifestations: The most visible signs are tight, thickened skin, often symmetrically distributed. Over time, the skin may lose elasticity, making it difficult to open the mouth or move fingers. Telangiectasia (dilated small blood vessels) and pigmentation changes are also common.
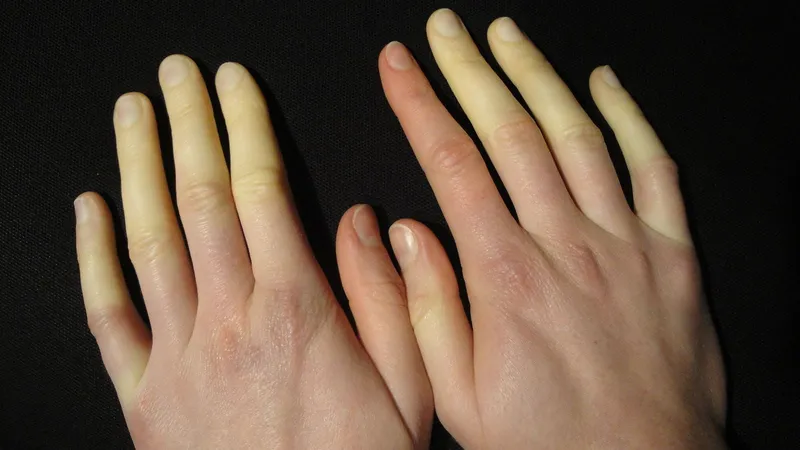
Raynaud’s Phenomenon: One of the earliest and most frequent symptoms, occurring in over 90% of patients. When exposed to cold or stress, small blood vessels constrict excessively, causing fingers or toes to turn white, then blue, and finally red as blood flow returns. Severe cases can lead to ulcers or even tissue necrosis.
Lung Involvement: Pulmonary complications are a major cause of death in systemic sclerosis. Patients may develop interstitial lung disease (ILD) or pulmonary arterial hypertension (PAH), leading to shortness of breath, fatigue, and coughing up blood.
Gastrointestinal Symptoms: Up to 90% of patients experience digestive issues such as acid reflux, difficulty swallowing, bloating, or malabsorption. Long-term complications include esophageal scarring and nutrient deficiencies (e.g., folate, vitamin B12).
Cardiac Manifestations: Although less common, scleroderma can affect the heart muscle and conduction system, leading to arrhythmias, pericarditis, or heart failure. Only about 15% of patients show overt cardiac symptoms, but prognosis worsens when they do.
Kidney Involvement: Renal crisis is a rare but life-threatening emergency associated with sudden severe hypertension and acute kidney failure. Immediate medical attention is crucial to prevent irreversible damage.
Musculoskeletal and Genital Symptoms: Joint pain, tendon inflammation, and muscle weakness are frequent, especially in the hands and knees. Men may experience erectile dysfunction, and women often report vaginal dryness and discomfort during intercourse due to tissue fibrosis.
Possible Complications
If untreated or poorly controlled, scleroderma may lead to severe complications, including:
- Raynaud’s phenomenon and digital ulcers
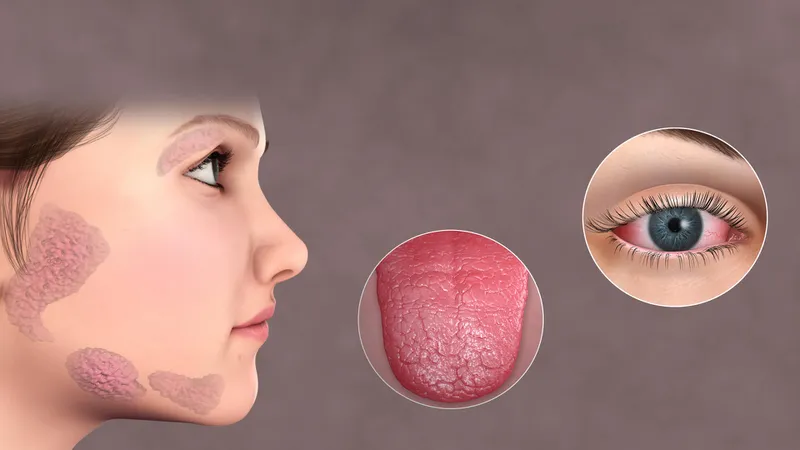
- Sjögren’s syndrome (dry eyes and mouth)
- Pulmonary hypertension and interstitial lung disease
- Heart failure and conduction abnormalities
- Kidney crisis and chronic renal failure
- Gastrointestinal malabsorption
- Immune dysfunction and increased cancer risk
When to See a Doctor
Seek medical advice promptly if you notice:
- Persistent skin thickening or stiffness
- Difficulty swallowing or breathing
- Blue or pale fingers in response to cold
- Swelling or pain in the joints
- Chest pain, fatigue, or unexplained weight loss
Call emergency services if you experience chest tightness, severe shortness of breath, or acute kidney symptoms (sudden rise in blood pressure, reduced urine output).
Causes of Scleroderma
What Causes Scleroderma?
The exact cause of scleroderma remains unclear, but researchers believe it results from a complex interaction between genetic, environmental, and immune factors. In essence, the immune system — which normally protects the body from infection — mistakenly triggers chronic inflammation, stimulating fibroblasts to overproduce collagen, leading to tissue thickening and scarring.
While the underlying trigger is not fully understood, several mechanisms are thought to contribute:
- Autoimmunity: The immune system attacks the body’s own connective tissue, causing inflammation and fibrosis.
- Vascular dysfunction: Small blood vessels are damaged early in the disease, leading to poor circulation and ischemic injury.
- Abnormal collagen synthesis: Excess collagen deposition in the skin and internal organs leads to the characteristic stiffness and loss of elasticity.
Risk Factors for Scleroderma
Who Is at Risk?
Scleroderma can occur in anyone, but certain groups have a higher risk of developing the condition:
- Age: Most cases develop between 30 and 50 years old. It is rare in children and older adults.
- Gender: Women are four times more likely than men to develop localized or systemic scleroderma.
- Ethnicity: People of African descent are at higher risk of developing more severe and early-onset forms, particularly those involving the lungs and skin.
Genetic and Environmental Influences
1. Genetic predisposition: Having a first-degree relative (parent, sibling, or child) with scleroderma increases your risk up to 13 times. Certain genetic markers, such as HLA class II alleles, are associated with a greater likelihood of autoimmune activation.
2. Environmental triggers: Long-term exposure to silica dust, organic solvents (e.g., trichloroethylene, benzene), or vinyl chloride has been linked to the onset of scleroderma. These substances can damage the blood vessel lining and trigger an abnormal immune response, leading to fibrosis.
3. Hormonal factors: The predominance of scleroderma among women suggests that estrogen and hormonal regulation may influence immune activation and collagen synthesis.
Diagnosis and Evaluation of Scleroderma
Because scleroderma is a multi-organ disease, diagnosis often requires a multidisciplinary approach involving dermatologists, rheumatologists, pulmonologists, and cardiologists. The goal is to confirm the diagnosis, determine the extent of organ involvement, and monitor disease progression.
Diagnostic Tests May Include:
Blood tests: To detect autoantibodies such as ANA (antinuclear antibodies), anti-centromere, and anti-Scl-70 (topoisomerase I), which help confirm the autoimmune origin.
Pulmonary function tests: Assess how well the lungs are working and detect early interstitial lung disease or pulmonary hypertension.
Skin biopsy: A small tissue sample from affected skin may be examined under a microscope to assess collagen deposition and fibrosis.
Gastrointestinal endoscopy: Recommended if symptoms like acid reflux or swallowing difficulties suggest esophageal involvement.
Imaging studies:
- Chest X-ray or CT scan: Evaluate lung scarring or fibrosis.
- Echocardiogram (heart ultrasound): Check for pulmonary hypertension or heart involvement.
- Electrocardiogram (ECG): Detect arrhythmias or conduction abnormalities.

Treatment Approaches for Scleroderma
Although there is no known cure for scleroderma, modern therapies aim to control symptoms, prevent organ damage, and slow disease progression. Treatment must be individualized, based on disease type (localized or systemic) and affected organs.
1. Treatment for Localized Scleroderma
Localized forms like morphea and linear scleroderma primarily affect the skin and underlying tissues.
- Topical corticosteroids:
Applied to reduce inflammation and prevent further skin thickening. - Moisturizers and emollients:
Keep the skin hydrated and prevent cracking. - Phototherapy (UV light treatment):
May help soften skin lesions and improve pigmentation. - Methotrexate or oral corticosteroids:
Used for widespread or deep lesions, especially in linear scleroderma involving the face or limbs, to reduce fibrosis and prevent deformity.
2. Treatment for Systemic Scleroderma
The management of systemic sclerosis focuses on treating the involved organs, controlling autoimmune activity, and improving quality of life.
Medication Options:
- Immunosuppressive drugs: Methotrexate, mycophenolate mofetil, or cyclophosphamide help reduce immune system overactivity and slow fibrosis.
- Calcium channel blockers (e.g., nifedipine): Improve blood flow and relieve Raynaud’s phenomenon.
- Proton pump inhibitors (PPIs): Such as omeprazole or pantoprazole, used to treat gastroesophageal reflux (GERD) and prevent esophageal scarring.
- Antibiotics: Amoxicillin or ciprofloxacin may be prescribed to treat bacterial overgrowth causing chronic diarrhea or bloating.
- Corticosteroids: Low doses may relieve joint or muscle inflammation. However, high doses should be avoided due to the risk of triggering a scleroderma renal crisis, a life-threatening complication.
- Pulmonary hypertension therapy: Bosentan, sildenafil, or prostacyclin analogs may be used to improve blood flow in the lungs.
- Physical and occupational therapy: Help maintain mobility, prevent contractures, and improve daily functioning.
Supportive Lifestyle and Self-Care Measures
Protect your skin from cold exposure and trauma.
Avoid smoking, which worsens vascular damage.
Eat a balanced diet rich in antioxidants, calcium, and omega-3 fatty acids.
Practice regular stretching and gentle exercise to maintain joint flexibility.
Manage stress through meditation, yoga, or counseling — emotional well-being directly affects immune balance.
Summary Scleroderma remains a challenging disease, but early diagnosis and a multidisciplinary treatment plan can significantly improve outcomes and quality of life. While the condition cannot yet be cured, medical advances continue to enhance symptom control and long-term survival.
⚕️ Remember: If you experience persistent skin tightening, Raynaud’s phenomenon, or unexplained fatigue, seek medical evaluation as early intervention can prevent irreversible damage
Lifestyle & Prevention of Scleroderma
Healthy Habits to Help Slow the Progression of Scleroderma
Lifestyle habits:
Attend regular medical check-ups and monitor any unusual symptoms or signs.
Get an annual flu vaccination.
Quit smoking and avoid alcohol consumption.
Consult your doctor before taking any medication or supplement.
Engage in regular, moderate exercise suitable for your physical condition.
Maintain a positive attitude and stay socially connected with others.
Dietary habits: Follow a diet low in animal fats and processed foods to support overall health.
Effective Prevention Methods for Scleroderma
Since the exact cause of scleroderma remains unknown, there are no specific measures to prevent the disease completely. However, maintaining a healthy lifestyle can help reduce the risk of complications and promote better overall well-being.
Adopt healthy habits by exercising regularly, avoiding a sedentary lifestyle, balancing work and rest, eating a nutritious diet, and scheduling periodic health check-ups to monitor your condition and protect your long-term health.
