Discoid Lupus Erythematosus (DLE): Symptoms, Causes, and Prevention
Understanding Discoid Lupus Erythematosus
Lupus erythematosus is a chronic autoimmune disease that can damage different parts of the body, but in DLE, the effects are limited to the skin. Dermatologists classify lupus-related skin lesions into three types:
- Acute cutaneous lupus erythematosus (ACLE)
- Subacute cutaneous lupus erythematosus (SCLE)
- Chronic cutaneous lupus erythematosus (CCLE)
Among them, DLE is the most common form of CCLE, typically presenting as round or coin-shaped (discoid) plaques that may lead to skin atrophy, pigmentation changes, or permanent scarring.
While both discoid lupus and systemic lupus can cause skin rashes, DLE lesions are more severe and disfiguring, but they generally do not involve internal organs. However, systemic lupus can cause life-threatening complications involving the kidneys, heart, lungs, or nervous system.
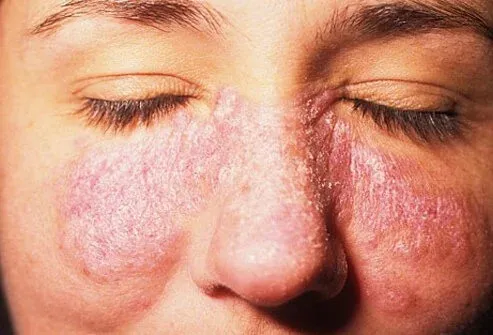
Common Signs and Symptoms
The first sign of discoid lupus is often a reddish or pink rash that gradually darkens. Lesions may appear anywhere on the body, but they are most common on the face, scalp, neck, and ears, areas frequently exposed to sunlight.
Typical skin changes include:
- Circular or coin-shaped lesions with well-defined borders
- Scaling or thickened patches on the scalp
- Crusting or blistering, especially around the elbows or fingertips
- Thinning skin in the affected area
- Pigmentation changes — darker (hyperpigmentation) or lighter (hypopigmentation) patches
- Permanent hair loss (scarring alopecia) in severe cases
- Brittle or curved nails
- Ulcers on the lips or inside the mouth
- Chronic scarring that may persist even after lesions heal
Important: Although DLE mainly affects the skin, chronic lesions — especially on the scalp — can cause irreversible hair loss and long-term pigment changes that may impact emotional well-being and self-confidence. Early diagnosis and sun protection are crucial.
Flare-ups are often triggered by UV exposure and may subside over time. The disease does not directly damage internal organs, but improper management can result in permanent disfigurement.
Possible Complications
While most cases of DLE remain limited to the skin, about 5–10% of patients may eventually develop systemic lupus erythematosus (SLE). Possible complications include:
- Scarring alopecia (permanent hair loss with visible scarring)
- Anemia or blood disorders
- Blood clots (thrombosis)
- Arthritis or muscle inflammation
- Hypertension
- Kidney involvement (lupus nephritis)
- Neurological issues such as seizures or depression
- Pleuritis or pericarditis (inflammation of the lung or heart lining)
- Pancreatitis or mesenteric vasculitis
- Optic neuritis (inflammation of the optic nerve)
- Skin cancer from long-standing, untreated lesions
- Vitamin D deficiency due to prolonged sun avoidance

When to See a Doctor
If you have not been diagnosed but notice any of the following, it’s time to see a dermatologist or rheumatologist:
- Circular or coin-shaped rashes on the face, ears, or scalp
- Thickened, scaly skin that doesn’t improve
- Unexplained hair loss
- Fragile or discolored nails
- Pigmentation changes in sun-exposed areas
If you have already been diagnosed with discoid lupus, monitor yourself closely and seek immediate medical attention if you develop any of these warning signs of flare-up or progression to systemic lupus:
- Sudden rash after sun exposure
- Joint or muscle pain
- Chest pain or shortness of breath
- Seizures or confusion
- Blurred or double vision
- Severe abdominal pain or vomiting
Causes of Discoid Lupus Erythematosus (DLE)
Discoid lupus erythematosus (DLE) is an autoimmune connective tissue disorder, meaning the immune system mistakenly attacks the body’s own skin and connective tissues. The exact cause of DLE remains unclear, but most researchers agree it results from a complex interaction between genetic susceptibility and environmental triggers.
Importantly, DLE is not contagious — it cannot spread through touch, blood, or any form of contact.
What Happens in the Body
In patients with DLE, immune cells become overactive, attacking healthy skin cells and causing inflammation, scaling, and scarring. Ultraviolet (UV) radiation often acts as a trigger, damaging skin cells and prompting the immune system to respond abnormally.
Risk Factors for Discoid Lupus Erythematosus
Who Is at Risk?
Anyone can develop discoid lupus, but the disease most commonly affects women aged 20–40 years. It is rare in children and occurs more frequently among people with darker skin tones.
Epidemiological studies show that:
- African American women are up to four times more likely to develop DLE than Caucasian women.
- Native American and Asian populations also show a higher prevalence compared to Europeans.
Genetic and Environmental Triggers
Certain genetic variations may increase the risk of developing DLE, especially when combined with environmental stressors.
Genetic Factors: TYK2, IRF5, and CTLA4 gene variants have been linked to systemic lupus erythematosus and may predispose individuals to discoid lupus as well.
Environmental and Lifestyle Triggers:
- Ultraviolet (UV) exposure: The most common trigger for lupus skin flares.
- Smoking: Associated with more severe and treatment-resistant disease.
- Certain medications: Including some antihypertensives, antibiotics, or antifungal drugs.
- Chronic stress or infection: May activate immune dysregulation.
- Skin trauma: Physical injuries or burns may initiate local lesions (Koebner phenomenon).

Diagnosis and Treatment of Discoid Lupus Erythematosus
How DLE Is Diagnosed
Diagnosis typically begins with a detailed medical history and thorough skin examination. Doctors look for telltale signs such as round, scaly plaques, pigment changes, and scarring.
In most cases, DLE can be diagnosed clinically, but to confirm the diagnosis or rule out other skin conditions, your doctor may recommend:
- Skin biopsy: A small sample is examined under a microscope to detect inflammation and immune deposits.
- Blood tests: To assess for the presence of antinuclear antibodies (ANA) or other markers that might suggest progression to systemic lupus.
Treatment for Discoid Lupus Erythematosus
While there is no permanent cure, DLE can be managed effectively. Early treatment helps prevent scarring and stop new lesions from developing.
1. Sun Protection and Lifestyle Modifications
Because UV light is a major trigger, sun avoidance is the cornerstone of DLE management.
- Apply broad-spectrum sunscreen daily, even indoors if near windows.
- Avoid outdoor activities during peak sunlight hours (10 a.m.–3 p.m.).
- Wear wide-brimmed hats, sunglasses, and long sleeves when outdoors.
- Avoid smoking and manage stress levels through relaxation techniques.

2. Topical Medications
Topical therapy is usually the first-line treatment for DLE.
Commonly used topical medications include:
- Topical corticosteroids (creams or injections): Help reduce inflammation and suppress immune activity.
- Topical calcineurin inhibitors (e.g., tacrolimus, pimecrolimus): Suitable alternatives when long-term steroid use causes skin thinning.
Treatment strategy:
- During flare-ups: Strong or very potent corticosteroids are applied for about 2 weeks to control inflammation.
- Maintenance phase: Milder corticosteroids or calcineurin inhibitors are used long-term to prevent relapse while minimizing side effects.
3. Oral Medications
When skin lesions are widespread or unresponsive to topical therapy, systemic medications may be required.
Options include:
- Oral corticosteroids: Used short-term to control acute flares. Long-term use is avoided due to side effects such as skin thinning, weight gain, and osteoporosis.
- Antimalarial drugs: Such as hydroxychloroquine, chloroquine, or quinacrine — often effective for chronic lupus skin lesions and relatively safe for long-term use.
- Immunosuppressants: Including azathioprine or methotrexate, prescribed when corticosteroids or antimalarials are ineffective or not tolerated. These drugs help reduce immune overactivity and inflammation.
Lifestyle Tips and Prevention of Discoid Lupus Erythematosus (DLE)
Living with discoid lupus erythematosus requires consistent skin care, sun protection, and lifestyle adjustments. While there is no known way to prevent the disease entirely, healthy daily habits can help control flare-ups, protect your skin, and slow disease progression.
Healthy Lifestyle Habits to Manage Discoid Lupus
Adopting a protective lifestyle is one of the most important parts of managing DLE.
1. Protect your skin from the sun
- Avoid direct sunlight whenever possible, especially during peak UV hours (10 a.m. – 4 p.m.).
- Apply a broad-spectrum sunscreen (SPF ≥ 50) generously on all exposed areas, and reapply every 4 hours or after sweating or swimming.
- Wear long-sleeved clothing, UV-protective fabrics, and wide-brimmed hats when outdoors.
- Use UV-filtering window films at home and in your car.
- Avoid tanning lamps and prolonged exposure to fluorescent or halogen lights, which can also trigger lesions in photosensitive individuals.
2,. Quit smoking and avoid alcohol
Smoking not only worsens lupus skin lesions but also reduces the effectiveness of medications such as hydroxychloroquine. Alcohol may interfere with your immune response and increase the risk of liver toxicity if you’re taking certain lupus medications.
3. Manage medication use wisely
Some prescription drugs can make your skin more sensitive to sunlight. Always ask your doctor whether your medications — such as diuretics, antibiotics, or antifungal agents — could trigger photosensitivity.
Nutrition and Diet Recommendations
Proper nutrition plays a supportive role in managing lupus by strengthening the immune system and promoting healing.
What to eat:
- Focus on fresh, whole foods: lean protein (chicken, fish), whole grains, fruits, and vegetables.
- Include omega-3 fatty acids (found in salmon, sardines, tuna, flaxseed, and walnuts) to help reduce inflammation.
- Get enough vitamin D from foods such as salmon, sardines, beef liver, egg yolks, shrimp, mushrooms, oatmeal, and yogurt — especially if you avoid sun exposure.

What to avoid:
- Highly processed foods, fried or greasy dishes, and sugary beverages.
- Excessive salt and refined carbohydrates, which can promote inflammation.
- Alcohol, as it can interact with medications and aggravate liver strain.
Preventing Flare-Ups and Disease Progression
Although DLE cannot be completely prevented, you can significantly reduce flare frequency and severity with consistent care.
Effective prevention strategies include:
- Apply broad-spectrum sunscreen daily (SPF 30 or higher), reapplying every few hours.
- Avoid sun exposure during midday hours.
- Limit exposure to indoor fluorescent lighting if it worsens your skin sensitivity.
- Wear protective clothing — long sleeves, gloves, and wide-brimmed hats.
- Do not scratch, pick, or touch active lesions to avoid scarring or infection.
- Avoid smoking and alcohol completely.
- Limit cosmetic use; always patch-test new products or seek medical advice before applying them.
- Consult your doctor before starting any new medications to ensure they won’t worsen lupus symptoms.
Living Well With Discoid Lupus
While discoid lupus erythematosus is a chronic disease, most patients can lead healthy, active lives with the right precautions.
- Stay consistent with dermatology and rheumatology check-ups.
- Keep a symptom diary to identify your flare triggers.
- Follow your medication schedule carefully.
- Maintain a balanced lifestyle with proper sleep, stress control, and a nutritious diet.
