What Is Allergic Dermatitis? Causes, Symptoms, and Prevention Principles
Overview of Allergic Dermatitis
Allergic dermatitis is a group of inflammatory skin disorders triggered by hypersensitivity reactions. It is generally divided into two categories:
1. Atopic Dermatitis
Atopic dermatitis is a chronic and relapsing skin condition characterized by itchy, eczematous lesions. It commonly begins in infancy and tends to occur in individuals with a personal or family history of allergic diseases such as urticaria, asthma, allergic rhinitis, or drug allergies.
2. Allergic Contact Dermatitis
Allergic contact dermatitis is a delayed hypersensitivity reaction, in which the skin becomes sensitized to specific allergens. The condition can present acutely with redness, swelling, and vesicles (small blisters), or progress into a chronic form with persistent inflammation and thickened skin after long-term exposure.
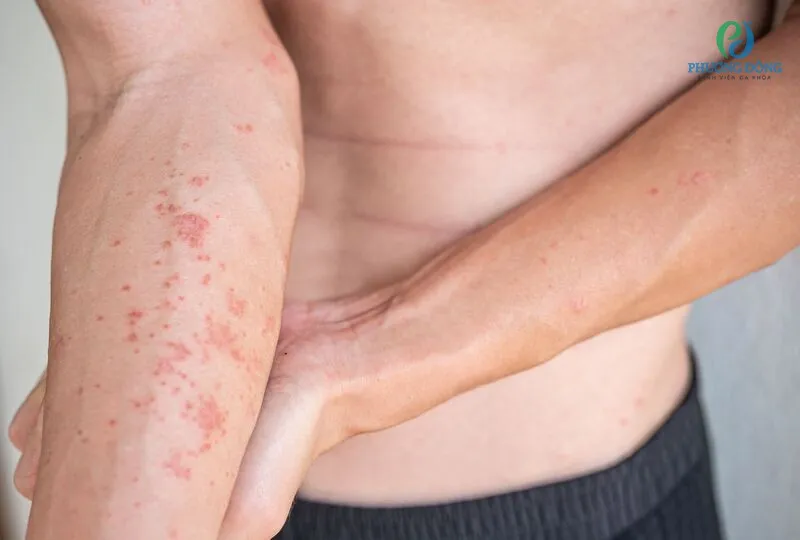
Symptoms of Allergic Dermatitis
Atopic Dermatitis
The condition usually appears during the first few months of life.
- Acute stage: The skin may become red, swollen, and oozing, sometimes accompanied by small blisters or crust formation.
- Chronic stage: Repeated scratching or rubbing leads to dry, thickened, and lichenified patches.
- Location: The distribution varies by age. In infants, lesions are typically found on the scalp, face, neck, and extensor surfaces of the limbs. In older children and adults, they often affect the flexural areas such as the neck, elbows, and knees.
- Itching: Persistent and intense itching is the hallmark symptom. It often worsens when exposed to allergens, dry air, sweating, wool clothing, or emotional stress.
Allergic Contact Dermatitis
The most prominent symptom is itching. Skin lesions evolve from redness to blistering and crusting, usually appearing on or near the hands, but they may also occur anywhere the allergen has come into contact with the skin.
Possible Complications
Allergic dermatitis, particularly atopic dermatitis, can lead to several complications:
- Secondary bacterial infection: Persistent scratching may cause oozing and open wounds, allowing bacteria (commonly Staphylococcus or Streptococcus) to infect the skin, sometimes resulting in impetigo or crusted eczema.
- Eczema herpeticum: Also known as Kaposi’s varicelliform eruption, this is a widespread infection caused by the herpes simplex virus. It presents with clusters of blisters, fever, and swollen lymph nodes, and may affect the eyes or even become life-threatening.
- Fungal or non-herpetic viral infections can also occur.
- Some patients may develop cataracts in their twenties or thirties.
When to See a Doctor
You should seek medical attention if you experience any of the following:
- Severe itching that disrupts sleep or daily activities;
- A rash that becomes widespread or more severe;
- Skin lesions that do not improve within three weeks;
- A rash affecting sensitive areas such as the face, mouth, or genitals.
Early diagnosis and treatment are essential to prevent complications, reduce flare-ups, and speed up recovery.
Causes of Allergic Dermatitis
What Causes Allergic Dermatitis?
Allergic dermatitis arises from a complex interaction between genetic predisposition, immune system abnormalities, and environmental triggers. The causes differ slightly between atopic dermatitis and allergic contact dermatitis.
1. Atopic Dermatitis
Environmental Factors
Environmental exposure plays a major role in the onset and progression of atopic dermatitis.
- Pollution: Airborne pollutants and irritants can damage the skin barrier, making it more vulnerable to allergens.
- Common allergens: Household dust, pet dander, fabrics, bedding, and other domestic materials can trigger flare-ups.
- Early-life environment: The condition tends to be more closely shared among siblings than between parents and children, suggesting that environmental factors in early childhood significantly influence disease development.
Genetic Factors
The precise genetic cause of atopic dermatitis remains unclear; however, heredity plays a substantial role.
- Around 60% of children born to one parent with atopic dermatitis will develop the condition.
- If both parents are affected, the likelihood can reach up to 80%.
- Genetic variations that affect the skin barrier proteins and immune regulation are thought to contribute to disease susceptibility.
2. Allergic Contact Dermatitis
Allergic contact dermatitis develops when the skin becomes sensitized to specific external substances. Common triggers include:
- Metals: Such as chromium, cobalt, and nickel, often found in jewelry or industrial materials.
- Medications and dyes: Certain colorants, ointments, and oil-based preparations can act as allergens.
- Adhesives and synthetic materials: Including plastic, rubber, and glues.
- Plants: Contact with certain plants may provoke allergic reactions.
- Sunlight: In some individuals, exposure to UV light can enhance or trigger dermatitis.
Risk Factors for Allergic Dermatitis
Who Is at Risk?
- Individuals with a family history of allergic dermatitis or other allergic conditions are more likely to develop the disease.
Factors That Increase Risk
Several elements may heighten the likelihood or severity of allergic dermatitis, including:
- Genetic predisposition to allergic conditions;
- Impaired skin barrier function, which allows allergens and irritants to penetrate more easily;
- Immune system dysregulation, leading to exaggerated inflammatory responses;
- Environmental exposures such as dust, mold, and air pollution.
Diagnosis and Treatment of Allergic Dermatitis
Diagnostic Methods and Clinical Evaluation
1. Atopic Dermatitis
Clinical Diagnosis
The clinical presentation of atopic dermatitis varies according to age.
In Infants:
- Symptoms often appear within the first three weeks after birth, usually as acute eczema progressing from redness and itching to small, fragile vesicles that ooze and form crusts.
- Secondary infection and lymph node enlargement may develop after several days.
- Commonly affected areas include the cheeks, but lesions may also occur on the scalp, forehead, neck, and extensor surfaces. When infants start crawling, eczema often appears on the knees.
- Some infants may react to foods such as milk, chicken, beef, or seafood; symptoms usually improve once the offending foods are eliminated.
- The condition is chronic and recurrent, with flare-ups triggered by tooth eruption, vaccinations, infections, environmental or climate changes.
- In most cases, eczema resolves spontaneously by 18–24 months of age.
In Children:
- Infantile eczema may evolve into localized or widespread erythematous papules, erosions, or vesicular lesions, often with secondary infection.
- Common sites include the popliteal and antecubital folds, neck, eyelids, and forearms.
- Exacerbations are frequently triggered by animal dander, wool clothing, or exposure to allergens.
- Malnutrition may occur if lesions cover more than 50% of the body surface.
- Approximately half of affected children experience spontaneous remission by age 10.
In Adolescents and Adults:
- Lesions typically present as itchy papules, vesicles, or thickened lichenified plaques.
- Common sites include flexural areas (elbows, knees), neck, periorbital region, and umbilical area.
- The palms and soles are often affected, especially in adults (20–80% of cases).
- Additional findings may include nipple eczema and periorbital dermatitis.
- When exposure to allergens, stress, or environmental changes persists, the condition tends to become chronic.
Other Clinical Features:
- Dry skin (xerosis) due to transepidermal water loss.
- Hyperkeratosis, keratosis pilaris, ichthyosis, and sparse eyelashes.
- Exfoliative cheilitis (scaling lips).
- Ocular complications: recurrent conjunctivitis, Dennie–Morgan infraorbital folds, periorbital hyperpigmentation, and posterior subcapsular cataracts.
- Dermographism (white skin writing) is sometimes observed.
Laboratory Findings (Paraclinical Tests)
- Elevated serum Immunoglobulin E (IgE) levels.
- Histopathology: Spongiosis and parakeratosis in the epidermis; infiltration of lymphocytes, monocytes, mast cells, and occasionally eosinophils in the dermis. In chronic lichenified lesions, epidermal hyperplasia is observed.
- Allergen identification through skin prick tests and patch testing.
Diagnostic Criteria (Hanifin & Rajka, 1980)
Major Criteria:
- Pruritus (itching).
- Typical lesion distribution: flexural lichenification in children, facial and extensor involvement in infants, linear or diffuse lesions in adults.
- Chronic or relapsing dermatitis.
- Personal or family history of atopy (e.g., asthma, allergic rhinitis, atopic dermatitis).
Minor Criteria:
- Xerosis, ichthyosis, keratosis pilaris, accentuated palmar creases.
- Hand and foot eczema.
- Nipple eczema, lip dermatitis, pityriasis alba, neck folds.
- Worsening with environmental or emotional factors.
- Itching after sweating.
- Elevated serum IgE.
- Periorbital hyperpigmentation.
- Dennie–Morgan folds.
- Conjunctivitis, keratoconus, posterior subcapsular cataract.
Diagnosis requires at least three major and three minor criteria.
2. Allergic Contact Dermatitis
Clinical Diagnosis
The presentation depends on disease severity, duration, and exposure level.
- Acute phase: Clearly defined erythematous and edematous plaques with vesicles or bullae. Ruptured vesicles exude fluid and form crusts. Severe itching is the predominant symptom.
- Subacute phase: Scaly, erythematous patches with small papules or dry skin.
- Chronic phase: Lichenified, thickened skin with deepened lines, fine scaling, and scattered papules. Lesions may spread and appear symmetrical.
Lesions usually appear within 48 hours after allergen exposure, and on subsequent contacts, symptoms occur more rapidly.
Removing the allergen leads to improvement, while re-exposure causes relapse.
Site-Specific Manifestations
- Scalp: Dry scaling, dandruff-like flakes, and itching; resolves after avoiding the allergen.
- Face: Redness, vesiculation, and oozing — often linked to cosmetics, medications, or sunlight exposure.
- Eyelids: Swelling, conjunctivitis, often due to topical eye medications.
- Earlobes: Commonly caused by nickel-containing earrings; dry, scaly, and itchy lesions.
- Lips: Dry, cracked, and scaly lesions, sometimes painful or swollen.
- Hands: Most frequently affected site. Acute lesions are vesicular and exudative, while chronic ones are dry and fissured. Often seen in dentists, cooks, or cleaners exposed to chemicals.
- Feet: Chronic dermatitis involving the dorsum and toenails.
- Genital area: Swelling, vesicles, and oozing in males (scrotum, foreskin) or females (labia majora).
- Airborne or volatile allergens: Cause symmetrical lesions on exposed skin areas; differentiation from photoallergic dermatitis is necessary.
Differential Diagnosis
- Irritant contact dermatitis
- Atopic dermatitis
- Seborrheic dermatitis
- Palmoplantar psoriasis
Histopathology
- Acute lesions: Pronounced spongiosis with intercellular edema and lymphocytic infiltration.
- Chronic lesions: Spongiosis with epidermal hyperplasia and lymphocytic infiltration in the dermis.
Patch and Prick Tests
Used to confirm and identify the causative allergen.
Effective Treatment for Allergic Dermatitis
Atopic Dermatitis
Treatment Principles
- Restore and protect skin barrier.
- Prevent or manage infections.
- Reduce inflammation and itching.
- Educate and counsel patients on proper skincare and trigger avoidance.
Topical Therapy
- Bathing: Use mild, non-alkaline cleansers and lukewarm water daily, followed by immediate application of moisturizers or emollients.
- Topical corticosteroids:
- Mild potency (e.g., hydrocortisone 1–2.5%) for infants.
- Medium potency (desonide, clobetasone butyrate) for children and adults.
- High potency (clobetasol propionate) for thickened or lichenified areas.
- Apply cautiously on thin skin (e.g., face), using low-strength ointments for short durations.
- Topical antibiotics or corticosteroid–antibiotic combinations for secondary infection.
- Soothing solutions: Burrow’s solution (Jarisch), potassium permanganate 1:10,000, or saline compresses.
- Moisturizers: Urea 10%, petrolatum for xerosis.
- Keratolytics: Salicylic acid 5–10%, ichthyol, tar preparations.
- Topical calcineurin inhibitors: Tacrolimus (0.03–0.1%)—highly effective but may cause initial irritation and are relatively expensive.
Systemic Therapy
- Antihistamines (H1 blockers):
- Chlorpheniramine 4 mg, 1–2 tablets/day.
- Fexofenadine 180 mg once daily.
- Cetirizine 10 mg once daily.
- Antibiotics: First-generation cephalosporins for Staphylococcus or Streptococcus infections, used for 10–14 days.
- Systemic corticosteroids: Short-term use only for severe flare-ups.
- Prednisolone 10–20 mg/day for 7 days, then taper.
- Other options: Cyclosporine or methotrexate in refractory cases.
Allergic Contact Dermatitis
General Principles
- The most critical step is identifying and eliminating the allergen; symptomatic therapy alone is ineffective without this.
Treatment Approach
- Severe or widespread acute dermatitis: Short course of systemic corticosteroids (e.g., prednisolone 15–20 mg/day for 3 days, taper to 5 mg/day for 3 days, then stop).
- Topical corticosteroids: Choice depends on disease stage and site.
- Mild lesions: low- to medium-potency agents.
- Thick or chronic plaques: stronger formulations for limited duration.
Lifestyle and Prevention of Allergic Dermatitis
Healthy Habits to Help Control Allergic Dermatitis
Lifestyle Recommendations
Adopting proper skincare and hygiene habits plays a crucial role in managing allergic dermatitis and preventing flare-ups.
- Keep the affected skin clean: Gently cleanse the skin and avoid exposure to allergens, dust, smoke, or polluted environments.
- Avoid harsh products: Minimize the use of cosmetics, fragrances, and strong soaps that can irritate sensitive skin.
- Choose comfortable clothing: Wear breathable, soft fabrics such as cotton. Avoid wool or rough-textured materials that may cause itching.
- Protect your skin: Use protective clothing and sunscreen when exposed to sunlight or cold wind.
- Use lukewarm water when bathing: Hot water can strip natural oils and worsen dryness. Keep the skin hydrated after bathing.
- Monitor skin changes: If new or worsening symptoms appear during treatment, contact your dermatologist promptly for advice.
Nutritional Recommendations
A balanced diet supports skin health and reduces allergic sensitivity.
- Eat nutrient-rich foods: Include plenty of fruits, vegetables, whole grains, and foods high in vitamins, minerals, and fiber.
- Avoid potential allergens: Refrain from consuming foods known to trigger allergies such as seafood, peanuts, milk, soy, eggs, and certain types of fish.
- Stay hydrated: Drink adequate amounts of water daily.
- Limit irritants: Avoid alcohol, caffeine, and stimulants that can aggravate inflammation.
Effective Prevention Strategies
Preventive measures are essential for reducing the frequency and severity of allergic dermatitis flare-ups.
- Understand your condition: Patients should be educated about their disease, its triggers, treatment options, and possible risks and benefits.
- Eliminate or minimize triggers: Maintain a clean, well-ventilated living space free of dust and pet dander. Avoid wool fabrics and emotional stress when possible. Cotton clothing is generally recommended.
- Use protective gear: When handling irritants—such as household cleaning products—wear gloves or protective clothing.
- Moisturize regularly: Apply emollients daily, especially in winter, two to three times a day to strengthen the skin barrier.
- Bathe with care: Use mild, fragrance-free cleansers and apply moisturizer immediately after bathing to retain moisture.
- Practice targeted food avoidance: Eliminate specific foods only if allergy testing confirms sensitivity.
- Be cautious with pets: Allergens from plants or the environment can cling to animal fur and trigger reactions upon contact.
